A new study from Public Health England (PHE) and Cambridge University was published in the Lancet last week, claiming to find that the Delta variant “doubles a patients’ risk of hospitalisation compared to the Alpha variant”, as the Telegraph reported (as did the BBC).
Reviewing over 40,000 sequenced positive PCR test results from England between March 29th and May 23rd, 2021, the researchers found that 2.2% of Alpha infections (764/34,656) and 2.3% of Delta infections (196/8,682) were hospitalised within 14 days of their first positive test. However, once they adjusted for factors such as age, ethnicity and vaccination status they found the risk of hospitalisation from Delta more than doubled compared with Alpha (a 2.26-fold increase).
The authors took the opportunity to use the results to stress the importance of being vaccinated, noting that only two per cent of those hospitalised were double vaccinated. However, this data is out of date, as more recent data from the main Delta surge suggests that vaccine efficacy against Delta infection may be as low as 15%.
The finding that Delta is more than twice as serious as Alpha is surprising as official data shows that hospitalisations have been much lower with Delta than Alpha. Data in the PHE technical briefings on the variants of concern shows that between February 1st and August 15th, 2.9% of sequenced Alpha infections resulted in an overnight hospital stay, compared with 1.9% of sequenced Delta infections. Technical Briefing 21 (the most recent) acknowledges this but adds that “a more detailed analysis indicates a significantly greater risk of hospitalisation among Delta cases compared to Alpha (see page 50 of Variant Technical Briefing 15)”.
Technical Briefing 15 quotes the findings, then in pre-print form, which are now published in the Lancet study (I criticised an earlier version of the claim here).
March 29th to May 23rd, the study period, is notable for being a period of low prevalence in England, when there were only around 2,000 reported infections a day (compared to a peak of around 50,000). In the over-60s in that period there were only 100-200 reported infections per day.
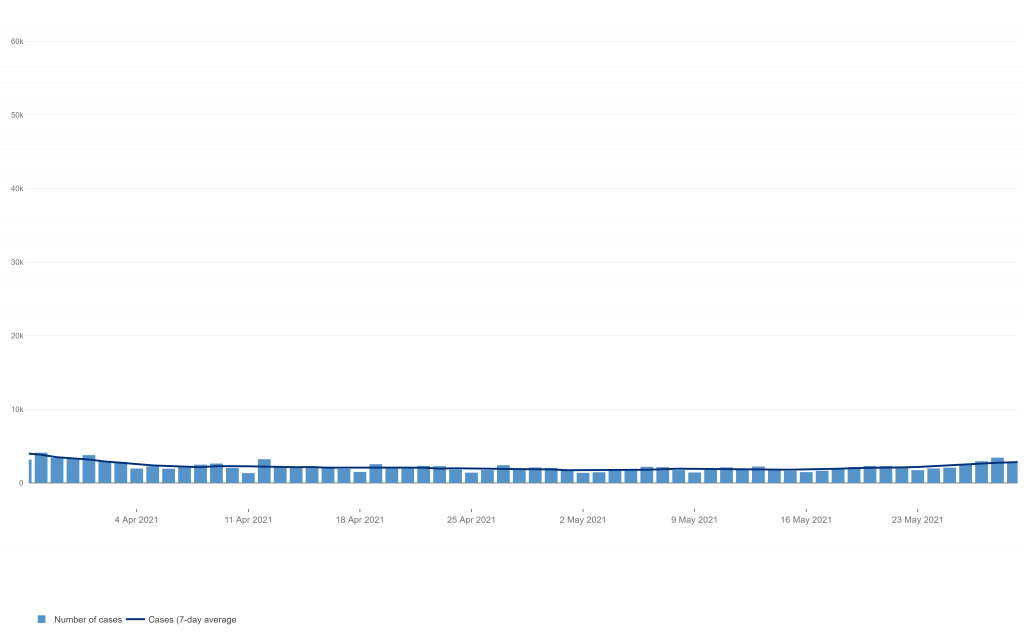
This is important because it means that what we are looking at in this study is Alpha as a spent force once it is no longer spreading fast and infecting large numbers of people. In other words, it is an exhausted variant to which herd immunity has been established in the population – which is why it declined sharply from the end of December in England and never resurged as restrictions were lifted. Delta, on the other hand, was the new variant on the block at this point, about to begin its own surge, so at an entirely different epidemiological stage and much more capable of finding susceptible people.
So once again we find PHE comparing the characteristics of a fresh, new variant to an exhausted, old variant and claiming to tell us something absolute about the properties of the two. PHE is still on record from June claiming that Delta is “64% more transmissible” than Alpha, an analysis that only looked at exhausted Alpha versus fresh Delta and failed to spot that Alpha’s secondary attack rate had dropped from 15.1% in December to 10% in May. Delta hit 13.5% in May but never got as high as Alpha’s winter peak rate and has been declining since, dipping below 11% by July.
A similar problem besets the new study. Alpha now may be less serious than Delta, but it’s not a fair comparison as it’s like comparing a pensioner with an athlete.
Look at Technical Briefing 8 from April. There, the case fatality rate of Alpha over the winter (October 1st to March 31st) was stated as 2.3%. This fatality rate is significantly above the hospitalisation rate for Delta in the latest figures of 1.9%, and is the same as the hospitalisation rate for Delta in the new study. On these figures, Alpha in the winter was much more serious than Delta now. It was also much more serious than Alpha post-winter, as its case fatality rate halved after February 1st to 1.2%.
We’re not given variant hospitalisation data prior to February 1st, but the winter surge was dominated by Alpha. Dr Clare Craig has calculated that between December 1st and April 30th the case hospitalisation rate during the Alpha surge was as high as 9%, many times higher than the 2.2% for Alpha quoted in the new study. Since May 1st, corresponding to the Delta surge, it’s been 2.3% (in line with the figures from the study).
A number of factors may have contributed to this lower recent hospitalisation rate: a higher proportion of younger people being infected, protection through vaccination, and the fact that it is summer rather than winter, among others. The study authors evidently agree, which is why their study purports to adjust for these factors to find that, underneath it all, Delta doubles the risk of hospitalisation compared with Alpha.
However, by comparing Delta in its prime to Alpha in its dotage the comparison is not valid and tells us nothing useful. It’s hardly surprising that Delta when new is more serious than Alpha when old – if large numbers of people were still susceptible to Alpha it would have had a resurgence of its own, not died away. But that doesn’t mean Delta is more serious than Alpha was in its winter prime, which is the only relevant comparison – and the one which most people assume is being made.
I would criticise the study authors for being misleading, but it’s not clear to me that those carrying out this research recognise that variants do not have the same epidemiological properties or clinical features when they’re new and when they’re old. This seems to be a crucial lesson about the behaviour of this virus (and presumably other similar viruses) which our ‘experts’ are being very slow at picking up.











To join in with the discussion please make a donation to The Daily Sceptic.
Profanity and abuse will be removed and may lead to a permanent ban.