A study published this week in the Journal of the American Medical Association (JAMA) has found that the risk of myocarditis (heart inflammation) after receiving an mRNA Covid vaccine (Pfizer or Moderna) was dramatically increased across many age groups and was highest after the second vaccination dose in young men.
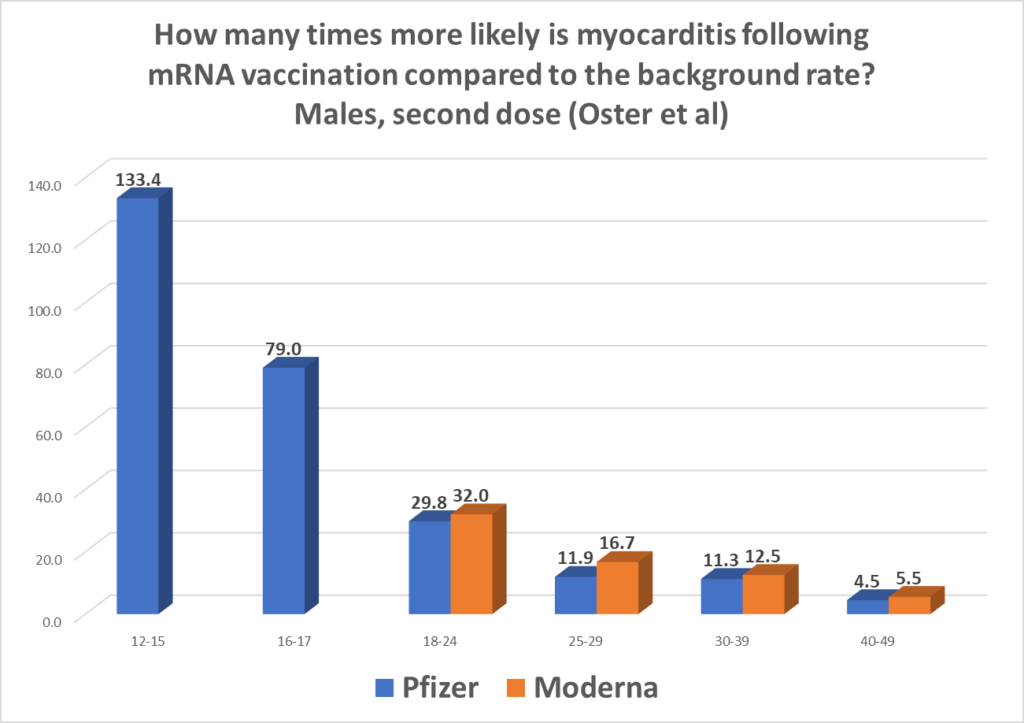
The study found myocarditis reports were highest after the second vaccination dose in males aged 12 to 15 years at 70.7 per million Pfizer doses, compared to an expected rate of 0.53 per million, amounting to a 133-fold increase; in males aged 16 to 17 years at 105.9 per million Pfizer doses, compared to an expected rate of 1.34 per million, amounting to a 79-fold increase; and in young men aged 18 to 24 years at 52.4 per million Pfizer doses and 56.3 per million Moderna doses, compared to an expected rate of 1.76 per million, amounting to a 30-fold and 32-fold increase respectively. The full results are shown in the table below and a selection are depicted in the chart above.
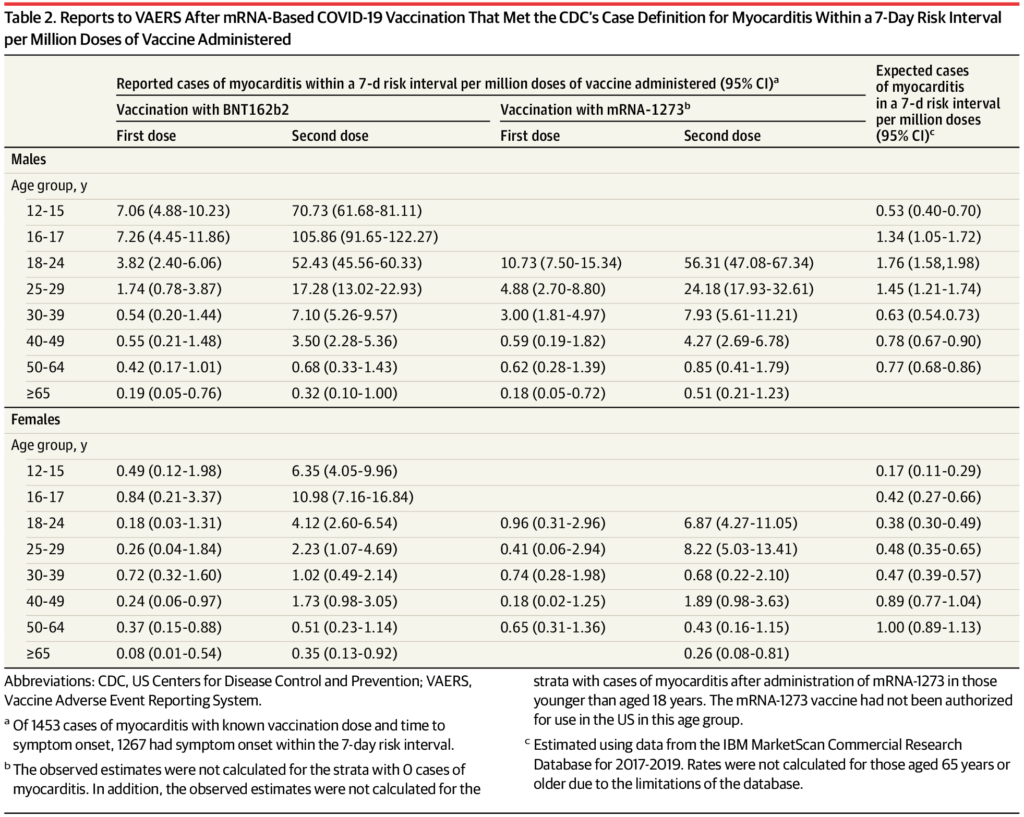
The study comprised a review of reports of myocarditis to the U.S. Vaccine Adverse Event Reporting System (VAERS) that occurred after mRNA Covid vaccination between December 2020 and August 2021 in people over 12 years old. The researchers adjudicated and summarised the reports and compared the rates to expected rates of myocarditis using 2017-2019 data. For those under 30 they conducted medical record reviews and clinician interviews to investigate clinical presentation, test results, treatment, and early outcomes.
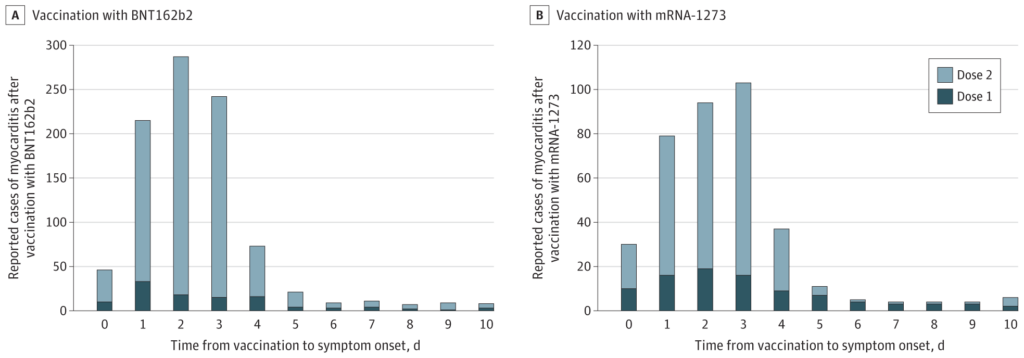
They found that out of 192,405,448 individuals receiving a total of 354,100,845 mRNA-based COVID-19 vaccine doses during the study period, there were 1,991 reports of myocarditis to VAERS, of which 1,626 met their case definition of myocarditis. Among the 1,626 cases, the median age was 21 years and the median time to symptom onset was two days. Males comprised 82% of the myocarditis cases for whom sex was reported, and where timing was reported, 82% occurred after the second vaccination dose.
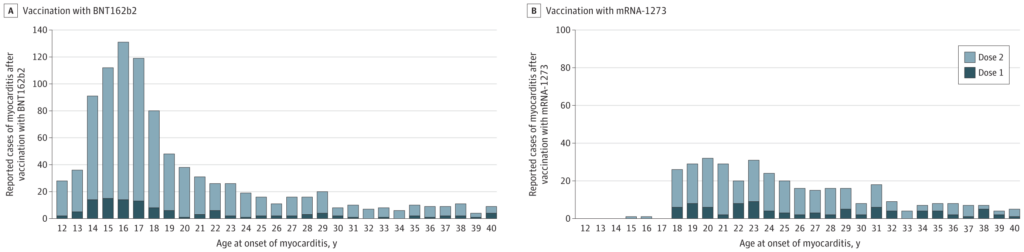
The charts showing myocarditis cases by age and symptom onset are shown below.
Regarding deaths, the researchers write:
Among persons younger than 30 years of age, there were no confirmed cases of myocarditis in those who died after mRNA-based COVID-19 vaccination without another identifiable cause and there was one probable case of myocarditis [in those who died] but there was insufficient information available for a thorough investigation. At the time of data review, there were two reports of death in persons younger than 30 years of age with potential myocarditis that remain under investigation and are not included in the case counts.
The authors note that a difference between vaccine-related myocarditis and virus-related myocarditis was that the former comes on more quickly; they also note that it appears to be milder:
The onset of myocarditis symptoms after exposure to a potential immunological trigger was shorter for COVID-19 vaccine-associated cases of myocarditis than is typical for myocarditis cases diagnosed after a viral illness. Cases of myocarditis reported after COVID-19 vaccination were typically diagnosed within days of vaccination, whereas cases of typical viral myocarditis can often have indolent courses with symptoms sometimes present for weeks to months after a trigger if the cause is ever identified.
The major presenting symptoms appeared to resolve faster in cases of myocarditis after COVID-19 vaccination than in typical viral cases of myocarditis. Even though almost all individuals with cases of myocarditis were hospitalised and clinically monitored, they typically experienced symptomatic recovery after receiving only pain management. In contrast, typical viral cases of myocarditis can have a more variable clinical course. For example, up to 6% of typical viral myocarditis cases in adolescents require a heart transplant or result in mortality.
To what extent are these differences a reporting artefact, where adverse event reports are only made when a reaction occurs within days of a vaccination, but otherwise the link is unnoticed or dismissed?
The authors note that underreporting is likely, “given the high verification rate of reports of myocarditis to VAERS after mRNA-based COVID-19 vaccination”, and therefore “the actual rates of myocarditis per million doses of vaccine are likely higher than estimated”.
Another recent study found post-vaccination myocarditis adverse events were underestimated by the VAERS definition.
A third recent study, from Oxford University, found that myocarditis risk following Covid vaccination was up to 14 times higher than that following COVID-19 infection. It has been suggested that that study underestimated the risk following vaccination. It should also be noted that since vaccination provides little protection against infection the idea that the risk following vaccination is instead of and not as well as the risk following infection is not sound.
Myocarditis is not the only serious side-effect of these vaccines, and the vaccines do not protect well against infection or transmission. This means it is increasingly clear that the current Pfizer and Moderna Covid vaccines do not have the efficacy and safety profile that would make giving them to children and young people worthwhile or ethical.










To join in with the discussion please make a donation to The Daily Sceptic.
Profanity and abuse will be removed and may lead to a permanent ban.
Part 1 of 2
The graph Professor Karl Lauterbach shared on Twitter is actually the perfect vehicle to highlight how dangerously wrong the authorities in the UK (and across the world) were in implementing a leaky vaccine campaign in the midst of a pandemic.
Actually, vaccinating a country against a virus when this virus was already intermingled in the populace was much more than simply dangerous, it was criminal.
The Marek’s virus in the 1970s and the following vaccination programme are perfect examples of how criminally dangerous it is to inoculate in the midst of a pandemic.
When the original strain of Marek’s virus infected chickens in the late 1960’s, it caused them to be sick, but in the vast majority of cases it didn’t kill them. Sick chicken’s decrease poultry farmer’s profits, so a cure was sought.
Big Pharma supplied the cure by coming up with a “leaky vaccine”. A leaky vaccine is a non-sterilising vaccine, that is, it protects only against symptoms/sickness when the inoculated animal or human becomes infected with the virus, it does not actually sterilise or kill the virus.
An animal or person inoculated with a leaky vaccine will be protected from symptoms if infected with the virus, but will still carry and spread this virus to others. This is what happened with Marek’s virus in the chickens. But because the leaky vaccine allowed the virus to freely jump from host to host, it actually selected for more virulent strains of the virus to replicate and spread.
When a virus first shows up in a population, right from the start there are strains present with different levels of virulence. When COVID-19 first appeared, its mutation into strains such as Delta and Omicron was a certainty. It could be said that these strains were there right from the start and were just waiting for the right vehicle by which they could infect host after host.
With the Marek’s virus, the right vehicle for the more virulent strains to spread themselves was the leaky vaccine. Prior to this vaccine, the unlucky chickens that got infected with a more virulent strain of this virus got too sick to move around and spread it to others. We all have in our heads that image of the sick animal or bird laying on its own away from the main herd or flock – and all the others instinctively keeping away from it.
Before the leaky vaccine, nature kept the most virulent strain of Marek’s virus in check by using incapacitation to stop its hosts from spreading it to other birds. Being sick is a pain-in-the-ass, but it’s also nature’s way of stopping individuals from spreading disease throughout their herd.
In quite a short time the leaky vaccine that was supposed to protect the chickens against Marek’s virus had led to the most virulent strain of this virus becoming dominant in the chickens. This strain was so virulent that the chickens that got infected with it almost all died.
Part 2 of 2
This led to the situation where all poultry farmers had no choice but to buy Big Pharma’s leaky vaccine and inoculate their chickens with it. If they didn’t inoculate all their chickens with this leaky vaccine, they’d lose all their birds if they became infected – and they would become infected because wild birds would carry this virulent strain from farm to farm.
At the start the poultry farmers should have let herd immunity deal with Marek’s virus. They’d have suffered profit losses in the short term, but herd immunity would eventually have done-away with the more virulent strains of the virus. And as the original moderate strain of Marek’s virus only made the chickens sick, it’s clear these fowl already had some natural immunity to it. It’s reasonable to assume this natural immunity would have evolved to a point where Marek’s virus didn’t bother the chickens at all – animals, humans and vegetables all carry harmless viruses that don’t do any harm.
As it is, all poultry farmers are now reliant on Big Pharma’s leaky vaccines, or else Marek’s virus will completely wipe out their flocks of birds. Which means steady profits for Big Pharma, and the chicken meat and eggs people eat having far more pharmaceuticals and chemicals than is necessary.
What has Marek’s virus and its leaky vaccine got in common with COVID-19 and its leaky vaccines? Well, “leaky” for a start. Yes, the COVID-19 vaccines are non-sterilising vaccines. Those inoculated with these vaccines can become infected with and carry and spread the COVID-19 virus and its variants – which, if nature was sentient, would have it scratching its head.
The effects that the COVID-19 leaky vaccines have had – and will have – on the population of the UK will be an exact plagiarism of the effect Marek’s virus and its leaky vaccine had on chickens.
It’s one thing, though, for the management of Big Pharma to use fraudulent, inadequate and non-vaccinating “vaccines” to enslave poultry farmers and their flocks of birds as their profit creating milch cows. It’s quite another when they’d coerce concoctions of drugs upon human populations in an attempt to do the same to them.
All the evidence was already there; and some scientists and doctors warned about it. There seems to be no doubt that Big Pharma purposefully used their COVID-19 leaky vaccines in a purposeful attempt to promote the spread of the more virulent strains of this virus. The more that the virulent strains spread and infected people, the more scared they became, and the more the leaky vaccines were accepted and taken.
And here I am just referring to the percentage of the mRNA serums that can be actually called leaky vaccines – the few and far between so-called vaccines that do actually alleviate the symptoms of the virus in people.
The multitude of adverse effects? These are another story of blatantly criminality.
If their intention was to promote the most virulent strains, they’ve done a bloody bad job of it.
Did they?
Here’s what Star says:
“There’s an all-time high “with SARSCov2” hospitalisation rate in Israel where 80% of adults are triple-“vaccinated” and the government of the regime which Albert Bourla of Pfizer loves so much is encouraging people to be “vaccinated” a fourth time.”
I suggest that the reason why we haven’t seen the equivalent of Marek’s (yet) is because the “vaccines” thankfully don’t protect against death (or if they do at all, it is very short-lived). The sheep would never understand that concept.
Many would find it too cruel to even think that sometimes sickness and death have to be accepted to keep the species as a whole healthy.
They fantasise about being in a sanitised world where we can live outside nature and where there will be an immediate magical remedy for all ills and hurts that come along.
And Big Pharma plays this for all it’s worth. And so many people just can not see that this leads to even more pain, hurt, sickness and death.
There’s the very real fact that the rates of autism in the West steadily increased as the usage of vaccines increased. The sheep won’t even question this, let alone demand an investigation into it.
Interesstingly, my wife and I received our Phizer jabs in Januray and early March 2021 and my wife (73 yrs) had a very severe case of Shingles (VZV) about 6 weeks after the 2nd jab. Although we had the Shingles jab 3 years before, she developed a rash that was diagnosed as very severe by theDr and has been left with PHN and is still suffering from that outcome.
Two of our medical consultant friends suggested that there was a link betweent eh Covid vaccine and the VZV and this has now been shown to be a possibilty from several other cases.
Why were vaccines permitted after such a short testing period and which are not like a smallpox vaccine which gives one immunity. These vaccines only seem to arrest the virus.
All the current evidence in the UK points to the HSE being not only untrustworthy, but of being actually willing to dispense, either through incompetence or malice aforethought, drugs that may have been purposefully designed to do harm.
Two new antivirals, supposedly designed to protect against COVID-19, have been in the news recently, ritonavir and molnupiravir. Ritonavir has been rushed out by Pfizer and is rumoured to be nothing more than a dressed-up ivermectin.
A few months ago, June Raine, CEO of MHRA, said about molnupiravir: “Following a rigorous review of the data by our expert scientists and clinicians, we are satisfied that Lagevrio (molnupiravir) is safe.”
Yet William A. Haseltine, a former professor at Harvard Medical School, has advised health authorities to be very careful about approving molnupiravir. He says this is because it has a very high potential for mutagenicity and a strong possibility to cause birth defects and cancerous tumours.
Mutagenicity in this instance is where this drug is feared to have the ability to actually bring about mutations in human cells.
Another greater and far deadlier danger (William A. Haseltine’s words) is molnupiravir’s potential to supercharge mutations in SARS‑CoV‑2 and unleash far deadlier variants of it upon the world.
Molnupiravir seems to be the type of drug you’d associate with the darkest Science Fiction fantasy, yet a few months ago June Raine of MHRA said it had been approved for use – and she said this without this drug having been put through any trials or tests in the UK.
But now the government has backtracked on this statement by June Raine; they have decided to run a full trial on molnupiravir and ritonavir. They are looking for something like 5,000 or 6,000 over-50s to participate in it.
There’s reports that a hydroxychloroquine trial in the UK was fixed to discredit this drug’s ability to treat SARS‑CoV‑2. It’s even been reported that the trial participants may have been overdosed with this drug and the harm this caused was attributed to COVID-19.
The health authorities in the UK have proved beyond doubt that they simply cannot be trusted. Where possible, people should do their own research into any drugs there are offered or prescribed.
I wish your wife and you the very best.
“Ritonavir has been rushed out by Pfizer and is rumoured to be nothing more than a dressed-up ivermectin.”
I guess the obvious name – Pfizermectin – would be a little too obvious.
They would be capable of actually calling it “Pfizermectin” just to sneer at us.
And the sheep would be totally oblivious, munching away on their diet of TikTok videos
The list of expected adverse reactions was conveniently discussed by the US FDA in an October 2020 pre-vaccination meeting.
Immune system interference is in there. Heart and thrombosis issues too. My sister also came down with a prolonged case of shingles. I also had an extremely fit and healthy friend come down with Guillain-Barre Syndrome (extremely rare) post-vaccination. A friend of a friend lost the greater part of a leg through complications to thrombosis post vaccination.
The virus is an RNA virus that can rapildy mutate until it achieves symbiosis with the host (the endemic stage – real time Darwinian selection). The mutation means vaccines do not work. The best that the drug makers can produce is a form of symptomatic relief as with the flu jab. I would not be surprised to find the vaccines are interfering with the symbiotic state, possibly throwing up new variants as the virus adapts to the presence of the anti-viral drug.
The drugs are not vaccines in the sense Joe Public understands. They are called ‘vaccines’ by the makers to allow them to go through clinical testing under less rigorous testing than applies to genetic therapeutics (at least in the US). The mRNA approach is a generic drug delivery mechanism, intended to form the basis for ‘personalised’ drugs which will be a gold mine for Big Pharma. There will be no need for expensive Phase III side effect tests as each drug is personalised (honest). That eliminates a massive cost centre for Big Pharma. It will also eliminate the other potential cost – the class action over adverse reactions. Phase III tresting is also where a substantial proportion( ~90%?) of drug candiates are rejected – being withdrawn by the maker as too dangerous (to their bottom line). Big Pharma has managed to get a massive mRNA trial run at no cost to itself, and with total legal immunity over pesky issues such as deaths of or severe injuries to trial participants.
Not quite. The reason why we haven’t seen the equivalent of Marek’s is because the vaccine pressure on virus evolution is all on the S domain, our natural innate immune system doesn’t target the S domain very much, because the natural response has evolved to target epitopes with the highest stability (i.e. those that do not change).
Mareks is a very unlikely scenareo for the unvaxed with natural immunity, it remains to be seen whether it will become an issue for those who took the jabs.
JC has covered this on his streams, highlighting the genetic domains most important to the innate immune response, to watch for antigenic drift, so far they have remained stable see his streams on twitch or download the latest stream deck/slides at gigaohmbiological.com
They’ve created a population with chronic covid disease. I’m not sure what the results of this will be.
But I don’t think the pharma companies will make more profits out of it (looking at current data) — it looks like the vaccine derived immunity from boosters stops being effective after the fourth dose (barely effective after the third — only a month or two of protection).
I’d like to form an action group where we petition governments worldwide to not buy any drugs from AZ, Pfizer, Merk and the rest; we can’t sue them because they wrote a ‘can’t sue us’ clause into the contracts.
With you on this.
I presume they can be sued for manufacturing contamination or for the so-called ‘bad batches’.
I’m just astounded that people have queued up to take a product with no liability insurance and with secret ingredients.
I wouldn’t be too sure about that.
https://ehden.substack.com/p/leaked-our-governments-secret-contract
Our government also committed that our country:
· “expressly and irrevocably waives any right of immunity … including but not limited to immunity against service of process, immunity of jurisdiction or immunity against any judgment rendered by a court or tribunal, immunity against order to enforce the judgment, and immunity against precautionary seizure of any of its assets.”
· “agrees not to assert any such immunity in any proceeding in connection with this Agreement.”
· “expressly and irrevocably waives the application of any Law in any jurisdiction that may otherwise limit or cap its obligation…”
It continues:
The contract state in article 8.1 that “Purchaser hereby agrees to indemnify, defend and hold harmless Pfizer, BioNTech, each of their Affiliates… and each of the officers, directors, employees and other agents and representatives… from and against any and all suits, claims, actions, demands, losses, damages, liabilities, settlements, penalties, fines, costs and expenses, whether sounding in contract, tort (delict), intellectual property, or any other (losses) caused by, arising out of, relating to, or resulting from the Vaccine, including…prescribing, administration, provision, or use of the Vaccine”
There safety studies, such as they were, were based on fraud so they can stick their clauses up their bum.
psifers medical “trial” showed lower all-cause mortality in the placebo group..
That should’ve been enough to halt the trail
They then jabbed the placebo group!
They also indemnified anyone who assisted the roll out in any way. Right down to the volunteers at the vaccination centres. The leaked contracts show this and the consequences of that is the Government has superceded the rule of law. Treason.
https://ehden.substack.com/p/leaked-our-governments-secret-contract
If you revisit Dr Richard Fleming’s research into “hot batches”, where he has apparently isolated batches of all these gene therapies to show degraded samples with all sorts of detritus visible on the slides; he points out that this becomes a “product” issue where “dirty” goods may induce harm because of careless manufacturing. I don’t underestimate the difficulty of taking this to court , but if it can be done anywhere, the US product liability laws are”it”?
Bit like going after Capone for tax fraud rather than racketeering – “how” doesn’t matter, but “if” and “when” do.
ps. Just read John001 comment – could not agree more.
I’m sure there is a good reason why Pfizer used part of the covid windfall profits to buy up a company specialising in the production of drugs to treat immune system issues, but I can’t quite think what it might be.
A virus will virus.
In any sane world, they should face charges of murder. Maybe if I was being kind, manslaughter.
But I’m beyond being kind.
Never forget, these people want to get kids jabbed.
Human shields. FFS.
Beyond evil is what is happening.
It’s evilness is so gigantic and far-fetched that many people have been blinded to it.
It’s so big that it’s like a person that has never seen the forest because he’s never been out of the forest; he’s always been blinded by the trees from seeing the actual forest or from even knowing he’s in one.
Believe it or not, a fellow once defrauded an American into buying London Bridge from him – as I remember, the American was conned into paying the conman a deposit. If this American had been buying a car he’d most likely have checked that the vendor could legally sell the car.
I suspect it was the psychology of the con that took in the American. Something like London Bridge being such a world-renowned symbol, so well known and so huge, surely nobody would have the nerve or gall to try to sell it unless they had the authority to do so?
Perhaps it’s a similar psychology that is blinding many people to the crime of the plandemic and fake vaccines?
There was an actual London Bridge sale, it got shipped to Arizona.
The story of the con (it may be an urban myth) was that the buyer thought he was buying Tower Bridge (the famous one) rather than the less impressive 1830’s “London Bridge” that was being replaced because it couldn’t take the weight of modern traffic.
The company that negotiated the sale from the City of London (London Bridge company IIRC) had a logo, a picture of the famous Tower Bridge
According to wiki he made his money back to cover all the costs!
https://en.wikipedia.org/wiki/London_Bridge_%28Lake_Havasu_City%29
I see.
If you tell a lie big enough and all that. I believe Goebbels was quoted in a similar vein.
In any sane world, they should face charges of murder. Maybe if I was being kind, manslaughter.
There is no reason to be kind, so let’s stick with (mass) murder. The people who authorised and promoted the use of these highly dangerous products were warned that they were taking major risks, but they chose to listen only to the siren voices of Big Pharma and their own “revolving door” advisors.
Despite mountains of evidence the injections are still being pushed. They are not backing down. As FW states this is evilness so gigantic and far-fetched that people cannot see or get their heads round what is happening.
They can’t back off. If they admit they were wrong they will be lynched.
Pretty much, yes.
Terrific work FW.
Thanks.
Never mind, parents. Observe the Precautionary Principle and have your kids jabbed to save other people from sniffles. You can always hope that it’s the kids next door who suffer the deadly side effects, and not yours.
There’s an all-time high “with SARSCov2” hospitalisation rate in Israel where 80% of adults are triple-“vaccinated” and the government of the regime which Albert Bourla of Pfizer loves so much is encouraging people to be “vaccinated” a fourth time.
This can’t be true can it? Surely the BBC would have picked it up lol
I made a FOI request to OFCOM sometime ago about Covid reporting. I’ll see if I can find the report. Basically what it said is that broadcasters should not spread misinformation about Covid. 2 things were missing –
1. What is misinformation?
2. Who decides 1? Who regulates the regulator?
Figures from the United States show that in the 12- to 20-year-old age group, cases of Myocarditis rose dramatically between 2019 and 2021:
Hello bells.
Totally unconnectedly, with ‘rare’ events such as myocarditis, here in Italy we are all saddened by the sudden death of a twelve year young boy.
A budding athlete, who tragically had the ‘usual’ heart-attack whilst completing a cross country run. He had been passed as completely fit (idoneo) by a sport doctor in November 2021 (a pre-requisite for children to do any sport , here in Italy)
Carlo Alberto Conte, rest in peace.
Il giornaledellitalia.it made this comment (translated)
https://www.ilgiornaleditalia.it/news/cronaca/331444/treviso-carlo-alberto-morto-infarto-vaccinato-covid.html
Was Charles Alberto vaccinated against the virus? Several hypothesis give a possible correlation between tragedy and drug administration. But what is the truth?
From what Il Giornale d’Italia learned, the boy has been subjected to two doses of vaccine and, despite everything, he also had Covid. Sara Scalco Councillor for Culture of the Municipality of Cartigliano (Treviso) confirmed this.
More at all Italian newspapers, where everything is quite controlled & a very safe space. Twelve year old boys did not used to die when I played cross country running in Yorkshire. Define ‘rare’ for me again, guys?
The British Heart Foundation are running an advertisement which “normalises” young people suddenly dropping dead on football pitches.
A charity that purports to specialise in helping people with damaged hearts, normalising heart attacks in children, how disgusting can you get? Like I alluded to in an earlier post on this thread, they do actually believe us ordinary people have the brains of chickens.
Perhaps they might get paid back for this when the hordes start dragging them to trial with the savagery of chickens tearing worms apart?
Yes I know.
When I used to play football way back, players around me used to drop like flies, all the time. Heart attacks, ten a penny.
You lying fuckers.
I wonder if there’s a film where the adverts have a message that’s not the obvious one….
you get a lot of adverts where they have a subliminal message.
Unforgivable. It’s disgusting. There seems to be no limits to how low people will go.
In an age with hyper-vigilance and social media, you’d wonder how they get away with it. I suppose because of conspiracy theories, they can just taint their enemies as suffering from it. A perfect cover.
What a disgrace that film is. People should boycott BHF charity shops and consider leafletting shoppers. Young sportspeople really are dropping dead and we all know why. My guess is the BHF may well belong to one particular pharma outfit. No idea which one.
There is a famous precedent for a conviction of a propagandist for crimes against humanity – Julius Streicher. Something tells me that when Britain’s leading politicians, especially Boris Johnson and possible replacement Tory prime ministers, try to outdo each other tomorrow on Holocaust Memorial Day (both Johnson and Starmer were already wearing commemorative badges in the Commons today), they won’t mention Streicher much, when he would be very much in his element if he were alive today.
They’d call Streicher a Nudger nowadays
Stretcher got his neck nudged. Thankfully.
Pfizer sells heart drugs (tafamidis for example). No doubt they donate to BHF.
I wrote challenging the BHF about facemasks when this crap started. Their reply about following government advice was absolutely shocking.
BHF – a wholly discredited organisation.
HP, they are a charity, so very unlikely to do anything to prejudice that status?
As they say…you couldn’t make it up, yet that is exactly what they’re doing.
Oscarone. Also in Italy. Another 12 year old died of a heart attack on 17 December in Austria. Leo Forstenlechner, keen footballer. Played with SU Inzing U13. He’d recently received the second dose. Previously in perfect health. Didn’t die on the pitch but at home.
This is tragic. My son is 12 and competing in cross country this week.
Obviously he’s not jabbed, but I bet some of the others are. I can only pray for them.
If public health authorities don’t withdraw their approvals despite all the evidence, I feel that’s gross negligence to the point of being criminal.
Indemnified.
The contract state in article 8.1 that “Purchaser hereby agrees to indemnify, defend and hold harmless Pfizer, BioNTech, each of their Affiliates… and each of the officers, directors, employees and other agents and representatives… from and against any and all suits, claims, actions, demands, losses, damages, liabilities, settlements, penalties, fines, costs and expenses, whether sounding in contract, tort (delict), intellectual property, or any other (losses) caused by, arising out of, relating to, or resulting from the Vaccine, including…prescribing, administration, provision, or use of the Vaccine”
https://ehden.substack.com/p/leaked-our-governments-secret-contract
BBRS, don’t agree – I am not a lawyer but have worked with legal issues all my life; public health authorities cannot be “…Affiliates…..agents and representatives”; they are separate legal entities, sometimes in different legal jurisdictions. Surely, even if they have contracted to buy the doses, their relationship is a contractual one between supplier and purchaser (offer,acceptance,consideration = evidence of a contract) – unless they have had some demonstrable part in the development funding for the research for these drugs, pre EUA, and have demonstrable responsibility for the pre/post EUA trials?
Tend to agree with TE, because of the daily disclosure of mounting evidence (the most recent of which is the testimony of US Attorney Renz about the massive hike in adverse reactions amongst US military personnel post jabs, the reporting of which appears far more organised but no less damning than the VAERS reports), this information cannot in law be ignored by any “public” Health Authority surely – to do so risks a prosecution for malfeasance…problem is who is going to file a complaint to whichever body – ?Police/High Court? – to start that process?
We need a “Sir James Goldsmith” with money to burn to kick start this IMHO.
The covid drug ‘contracts’ are not so much contracts as terms of indentured slavery.
On a separate note, if anybody wants a good laugh tonight, check out this piece of nonsense in the Guardian: Why mathematicians sometimes get Covid projections wrong | Kit Yates | The Guardian
Basically trying to offer excuses as to why the likes of Ferguson et al “sometimes” get projections wrong. I think the word this tool was actually looking for was always. They always get projections wrong. A-L-W-A-Y-S. And not just wrong, but spectacularly wrong. Seriously, why are people paid to write this gaslighting, deceitful bullshit?
“sometimes” get projections wrong
always get it wildly out of their own error bars (which are enormous)
Ferguson is consistently and wildly wrong in all of his spreadsheet astrology.
but remember, they are always looking for the worst case scenario for the government. Better question is WHY does the government want the worst case for the excuse of trashing the economy.
I hope this comment isn’t taken the wrong way. I certainly do not wish to offend anyone…………..apart from the Government.
I think it’s time for a re-run of Monty Python’s best episodes. The public need an opportunity to identify complete madness when they see it.
Basically, replace ‘Holy Grail’ by ‘Zero Covid’?
I hope people have seen this doctor’s blog …
https://tcp.art.blog/2021/11/25/all-hail-covid/
“Coronavirus – 1970s Public Information Film”
Coronavirus – 1970s Public Information Film – YouTube
LOL
the car owner virus!
I played rugby from my early teens until my mid thirties. Mostly social grass roots rugby, but because of the way the game was structured in those days we trained with some top players, and were trained by top coaches, some of them household names, at least at the time, especially in the pre season free for all sessions when all were welcomed. I never once in over 20 years of training or playing with overweight fourth teamers well past retirement or elite athletes in their prime playing representative sport at the highest level saw or heard of a cardiovascular incident. Although I did once see a diabetic county player hit one of his teammates in training while having a hypoglycaemic episode. At least that’s what he said.
Fabrice Muamba published a book in 2012 called “I’m Still Standing”. The only reason that he was asked to write a book, and people were interested in reading it, was because what happened to him was so rare.
No can’t be. These vaccines are “incredibly safe” & any suggestion that they might be a risk, especially for young people is “misinformation” ( copyright – Kemi Badenoch Mp 2021 )
the Vaccines (which are no more vaccines than an Asprin curing a headache is a vaccine for said headache) are a modern Miracle. Akin to the electric toning belts Argos used to flog that enabled fat folk to eat a Turkish delight while being hooked up getting perfect abs.
Horrific. Those pushing the ‘vaccines’ and who are in full knowledge of the dreadful side effects must be held accountable and if necessary pay the ultimate price. This is just pure evil.
It was clear from the very beginning, as all those Dr’s voices silenced on social media were shouting about.
Can we dispense with the faulty vaccines and associated nonsense now please Boris?
There Are Now 365 Studies that Prove the Efficacy of Ivermectin and HCQ in Treating COVID-19. Any hospital administrator who mandated the shots to employees to comply with the government mandate for Medicare and Medicaid reimbursement and who refused to allow alternative treatments to be tried, doctors who pushed their patients to take the EUA drug without giving fully informed consent, anyone who forcefully administered the shot, the AMA, AAP, Boards of Health, CDC, FDA, NIH, WHO, scientists who participated in the development, Big Pharma (Pfizer, Moderna, J&J, Astra Zeneca, et. al.), anyone who pushed the sick into nursing homes resulting in deaths, all must be arrested, prosecuted, tried and if found guilty sentenced to prolonged imprisonment and fines or death for intentional homicide. Get your ivermectin before it is too late! https://ivmpharmacy.com
Am I shocked?
This article showing the extremely elevated risk of myocarditis among vaccinated males is much appreciated. However, every myocarditis story should also include a paragraph that gives the mortality risk of the same group dying from the disease Covid.
For healthy children – those without severe pre-existing conditions – this risk is literally 0.0001 percent (six deaths in every 12 million healthy children).
You can’t get any closer to “zero percent risk” than this (at least with four decimal points).
From Mike Yeadon:
I’m not overly worried about “the virus” & cleverer people than me can cogitate on that.
On the other hand I’m very concerned indeed for anyone injected.
Respiratory virus infections are not the same as vaccination because the former ought usually to be restricted mostly to airways.
Injections go all over the body.
Utterly reckless lack of control of disposition, duration or amount of toxic spike protein & multiple pathologies from same
I will testify that the very design of the gene based vaccines was intentionally to harm. Let them defend against that accusation!
Anybody with me on this? I’m thinking ahead to a “Grand Jury” style pre-indictment hearing.
I guess Reiner will probably ask me to cover “the covid19 lies”.
While I could say something about the vaccines, I believe the jury of our peers will probably gain more confidence from hearing a medic speak. So initially I’m restricting my input to what was reasonable to expect based on the design of the vaccines.
Cheers!
Mike
1. Least stable part of the virus. Human immune response to injection hardly bothers with spike.
2. Spike & analogous external proteins of related viruses were known toxins. Spike was shown to be “fusogenic” & to cause thromboembolic problems. Spike is also weakly homologous to many human proteins eg syncytin-1 & cross-reacting immune responses were very likely.
3. No control of disposition, concentration of spike or duration of expression. Huge & intrinsic variability of biological responses as a direct consequence of choice of vaccine design. A conventional vaccine is likely to be more effective & much safer. There are no such products. Why not?
(Note: Novavax isn’t grown medium based vaccine but I believe recombinant).
4. Doesn’t induce protective sIgA (or good T-cell responses??)
5. Repeated injections obviously going to cause neoautoimmune reactions including attack on own immune system including damaged immune surveillance (hence increased virus infections & emergence of latent infections plus risk of missed cancer deletion in early times post mutation.
6. Vaccines to terminate an alleged global pandemic was known to be (a) stupid & risky, failing the first 3 rules for a public health intervention: safety, safety, safety.
Such initiatives will always fail, because long term safety cannot be assured in the timescales of any plausible pandemic. (b) most people are simply not at risk & aren’t targets for vaccines; (c) there are many safe & effective cheap & old generics rationally evaluated.
There’ll be mistakes & omissions plus plenty of time to address.
Irony: A disease that kills the very elderly or those with multiple comorbidities is ‘treated’ with a drug that kills the young and healthy.
Precisely why I’ve told my 22-year-old son who had the ‘cold’ last summer to saty well clear of the ‘clot shots’.