A pre-print study (not yet peer-reviewed) by U.S. Government researchers shows vaccinated people produce a less comprehensive immune system response following SARS-CoV-2 infection than unvaccinated people.
The researchers examined data from the Moderna Covid vaccine trial and found that, compared to unvaccinated controls, vaccinated participants produced far fewer N-antibodies. These are antibodies against the nucleocapsid protein inside the virus particle, in contrast to S-antibodies against the spike protein that the vaccines target. N-antibodies were detected in 40% (21 of 52) of infected vaccine recipients versus 93% (605 of 648) of placebo recipients. This means those infected after being vaccinated produced N-antibodies at less than half the rate of the unvaccinated.
The researchers found that N-seroconversion (producing N-antibodies following infection) was more likely for infections with higher viral loads. So they checked to see if the difference was due to the vaccinated having milder infections with lower viral loads owing to the vaccine. They found that it wasn’t: for the same viral load the unvaccinated were around 14 times (13.67, 95% confidence interval 5.17-36.16) more likely to have detectable N-antibodies following infection than the vaccinated. Look at the contrasting curves below: the yellow unvaccinated curve is much higher than the blue vaccinated curve, showing that for any given viral load (x-axis) the probability of detecting N-antibodies following infection (y-axis) is much lower for vaccinated than unvaccinated.
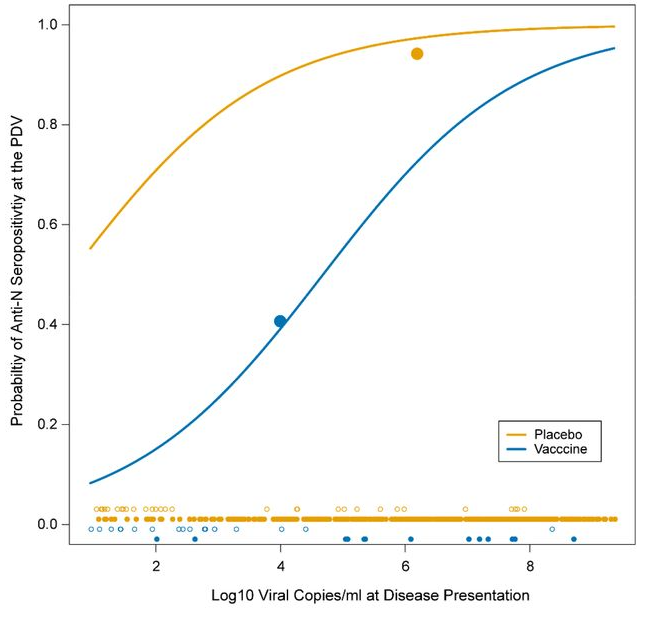
This means that although a vaccinated person may have S-antibodies from the vaccine, following infection he or she is much less likely to gain N-antibodies following infection than an unvaccinated person. This weaker immune response may make him or her more susceptible to future re-infection, particularly by variants which evade the S-antibodies, such as Omicron.
This also means, as the study authors point out, that a population survey of N-antibodies after a vaccination campaign will significantly underestimate the total number of people previously infected, as many of the vaccinated will not have produced N-antibodies following infection. This is likely one reason why the UKHSA reports around 42% of blood donors in England with N-antibodies to the end of February 2022, while the ONS estimates from its infection survey that around 71% of the country has been infected by February 11th (see below). The high infection rate among the vaccinated during the Delta and Omicron waves supports this explanation.
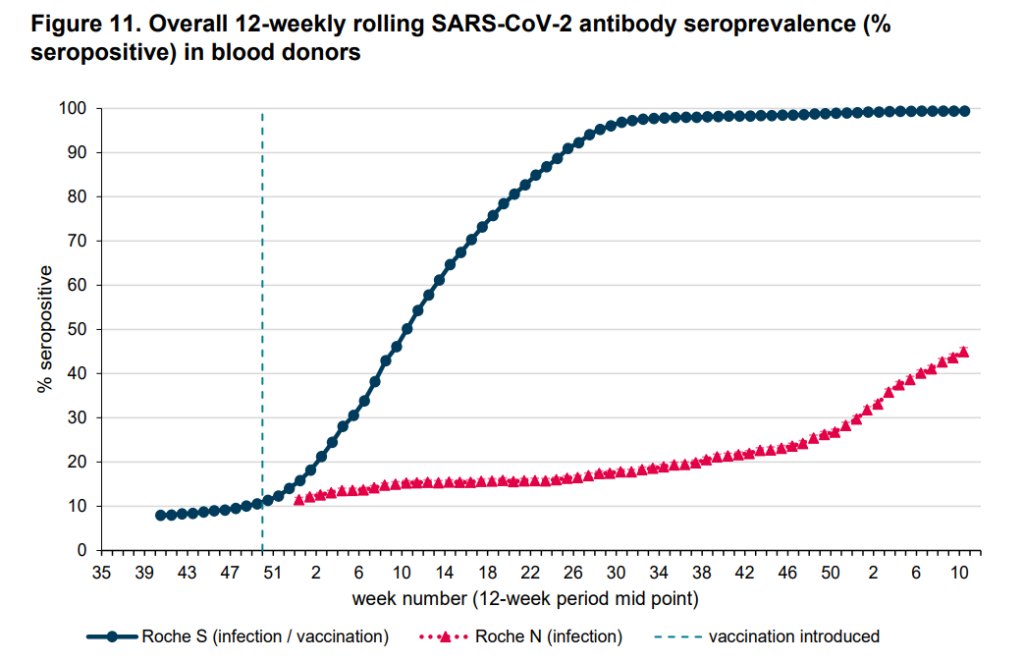
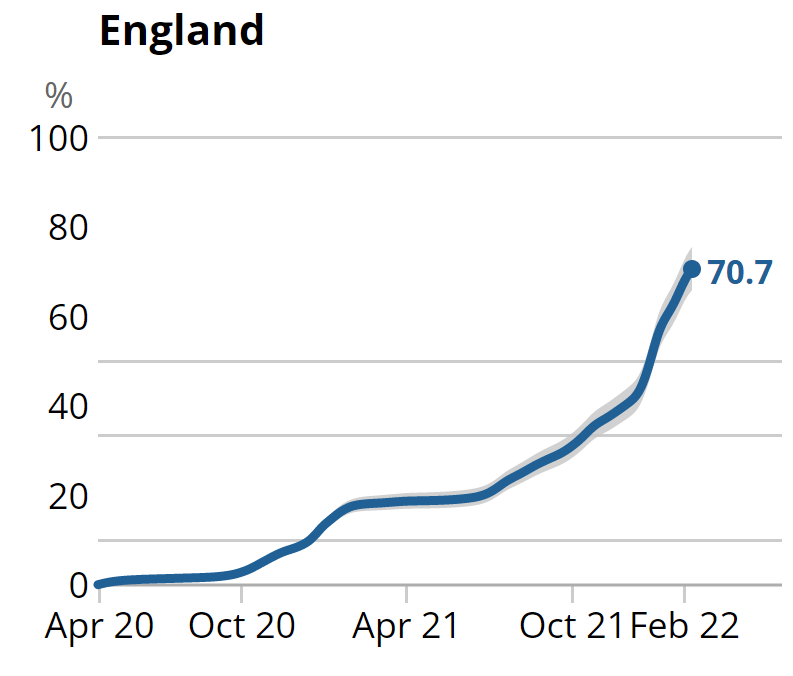
Let’s break those data down into successive Covid waves so we can see how many were infected in each wave according to the ONS and how many developed N-antibodies according to the UKHSA. In the below I’ve read 8% off the antibody graph above for the initial wave and, assuming the same proportion were infected in that wave, added a six point uplift to the cumulative infection total to allow for the pre-April 2020 infections.
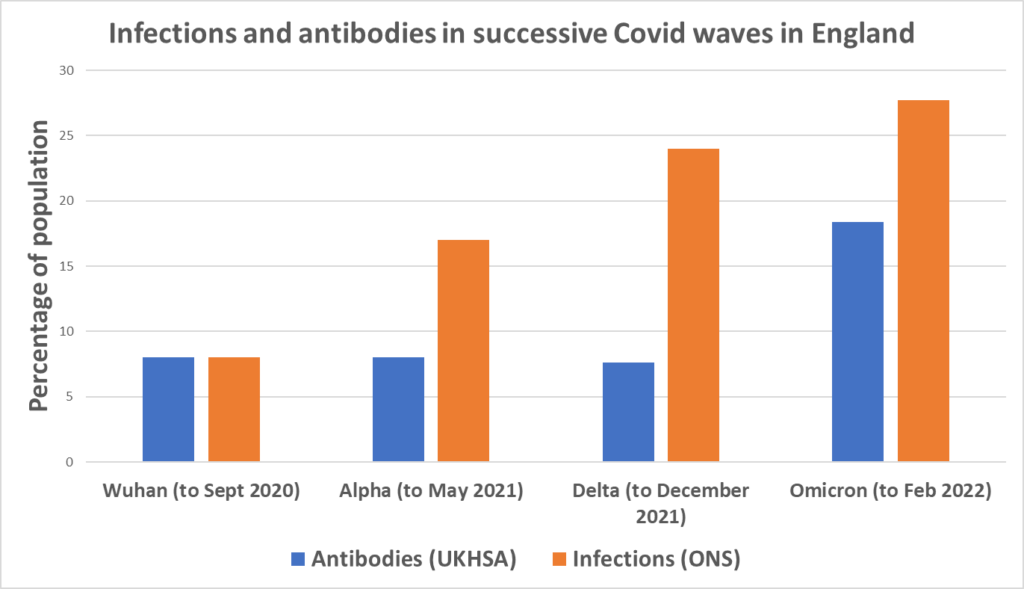
The most striking aspect of this chart is how much bigger the Delta wave was in infections than in antibodies – a result, we can assume, of the vaccines inhibiting N-seroconversion. It’s also notable that the pre-vaccine Alpha wave (almost all the infections for which occurred before February 2021, when very few were vaccinated) was around twice as large in infections than in antibodies, suggesting a relatively low rate of seroconversion despite the lack of vaccines, the reason for which is unclear. Then for Omicron, the ratio between the two gets much smaller, around 1.5, meaning infections were only 50% higher than antibodies. Here are those figures with the ratios.
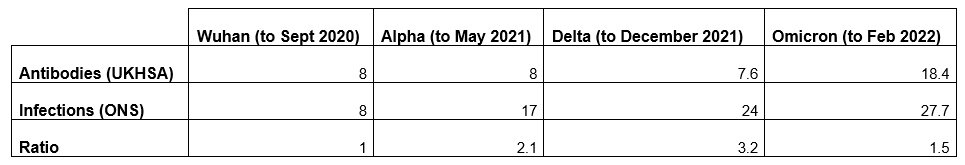
The low ratio of antibodies to infections for Omicron is a strong indicator that the vaccine is no longer inhibiting N-seroconversion. This may be because Omicron is so different to earlier variants; in particular, it has many immune-evading mutations in its spike protein, so that the S-antibodies from the vaccines are largely ineffective against it. This means the immune system must engage with it more comprehensively to fight it off, thus producing N-antibodies. The evasion of S-antibodies, of course, is also why the vaccines do so little to protect against Omicron. The lack of N-seroconversion following infection is likely why many vaccinated people caught Omicron not long after catching Delta. Additionally, the relatively small size of the Omicron wave in South Africa, where vaccination rates are low, adds to the evidence that vaccination played a significant part in driving the Omicron wave in the U.K. and other highly vaccinated countries.
To sum up: antibody surveys appear always to underestimate the number of Covid infections, as a significant proportion fail to seroconvert. This is particularly true following vaccination with vaccines which target a specific protein, such as the current Covid vaccines, though was also true in the pre-vaccination era with the Alpha wave, albeit to a lesser extent. While antibodies are generally a better guide for infections with high viral load, this doesn’t hold following vaccination. Antibody surveys particularly underestimate the size of the Delta wave in populations with high vaccination rates. The vaccine inhibition of N-seroconversion appears to fade with a vaccine-evading variant like Omicron as the wider immune system re-engages.











To join in with the discussion please make a donation to The Daily Sceptic.
Profanity and abuse will be removed and may lead to a permanent ban.