A snapshot of data from the beginning of the month in Israel suggests that the Pfizer vaccine is not protecting against infection now the Delta variant is in town, with infections in the vaccinated across all age groups being no less than you’d expect if the vaccine did nothing.

Could there be another explanation here? Possibly. It’s only a snapshot. What if infections in the unvaccinated peaked earlier than in the vaccinated, as ZOE data at one point showed happening in the U.K.?
Talking of ZOE data, in the middle of last week the study updated its methods (described here) which had the result of completely removing the peak in the unvaccinated infections and replacing it with the opposite, a further climb (see below, the old method put the peak around July 1st).
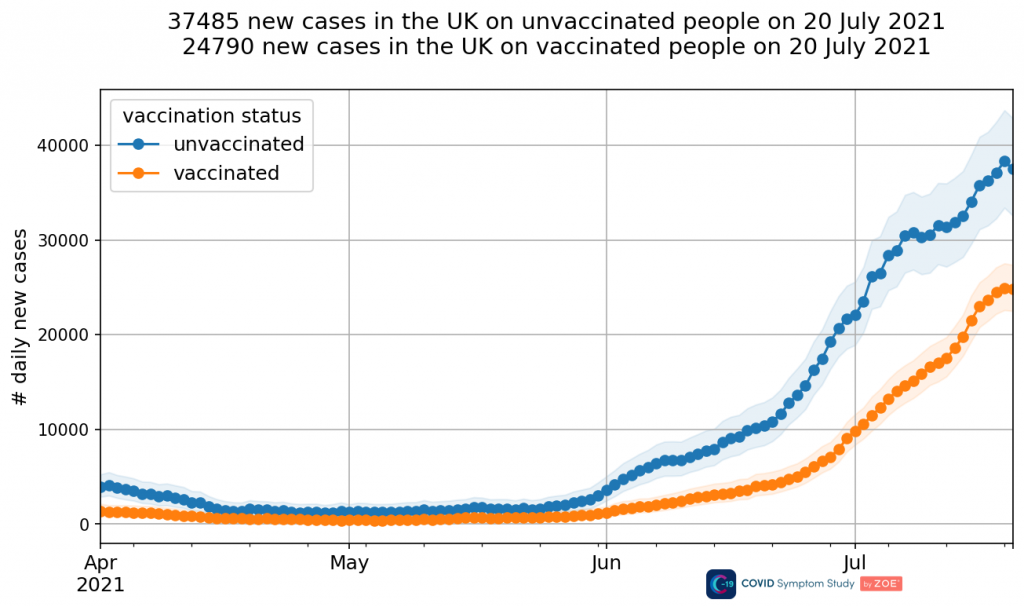
It’s hard to know what to make of such a radical change. One of the main takeaways for me is that it’s difficult to see how one can really trust ZOE data now or rely on it for anything. If it can change so radically from one day to the next, overturning the former trend, then how can it be relied on at all? If it was so wrong before, what confidence should we have that it’s correct now? It’s hard to shake the feeling that it was changed because it didn’t look right to someone, and was changed until it looked right. They even state: “We can see our updated methods align more closely to trends observed in Government confirmed cases.”
But back to Israel. New statistics from the Israeli Health Ministry are not quite so alarming as the above snapshot suggests, but they’re not far off. They suggest that the Pfizer vaccine is only 39% effective against the Delta variant, dropping to 16% for those vaccinated in January. The Times of Israel reports:
New Health Ministry statistics indicated that, on average, the Pfizer shot — the vaccine given to nearly all Israelis — is now just 39% effective against infection, while being only 41% effective in preventing symptomatic Covid. Previously, the Pfizer-BioNTech vaccine was well over 90% effective against infection. …
The Israeli statistics also appeared to paint a picture of protection that gets weaker as months pass after vaccination, due to fading immunity. People vaccinated in January were said to have just 16% protection against infection now, while in those vaccinated in April, effectiveness was at 75%.
Doctors note that such figures may not only reflect time that has passed since vaccination, but also a bias according to which those who vaccinated early were often people with health conditions and who are more prone to infection, such as the elderly.
While it may be true that the more frail were in the earlier cohort, even so 16% is very low, frail or not, and that will be an average, with some higher than that (the less frail among the early vaccinated perhaps) and some lower still.
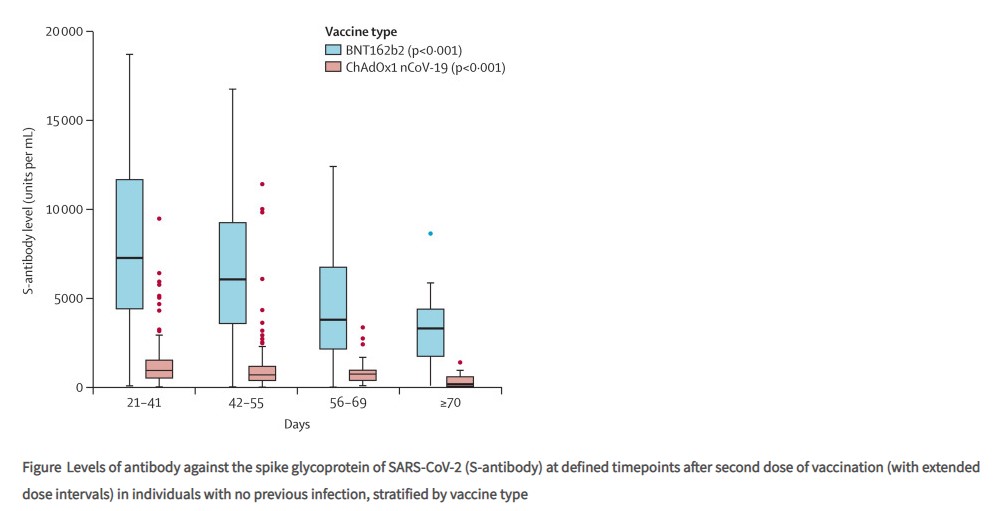
A new study in the Lancet has shown that antibodies from the vaccines notably decline over the course of three months (see below), which may support the idea of declining efficacy over time – though as the authors point out, antibody levels don’t by themselves determine real world effectiveness because “memory B-cell populations appear to be maintained”.
Some Israeli scientists are unhappy about the way the data is being used by their Government to imply that boosters and new restrictions are needed, saying the definition of serious illness has been changed and the statistics, which are dealing in small numbers, don’t take into account the different propensity of vaccinated and unvaccinated people to be tested for Covid.
Others, however, are sceptical about the efficacy of the vaccines. The modelling team at University College London is now working on the assumption that the vaccines have basically zero effectiveness against infection by the Delta variant. However, they also somewhat incongruously assume they are 85.5% effective at preventing transmission. Neither figure is supported by any obvious references so it’s not clear how seriously to take these estimates.
Meanwhile, the team at Public Health England (PHE) has had its study on vaccine effectiveness against the Delta variant published in the NEJM. The pre-print estimated AstraZeneca effectiveness (two doses) against infection with the Delta variant at 59.8%, but with new data this is up to 67%. It estimates Pfizer efficacy against Delta at 88%. Why this is so different to the latest Israeli data (39%) has been a matter of some discussion. The Swiss Doctor (SPR) suggests it is because the PHE data is out of date, coming from April and May when prevalence was low. The infection rate in the unvaccinated will also be skewed upwards by the cohort being younger (younger people have higher infection rates regardless of vaccination status) and it’s unclear how fairly PHE’s adjustments have allowed for that.
Separately, it was reported last week that Australian socialite Anthony Hess, who is fully vaccinated, spread the virus to 60 people during a busy weekend in Los Angeles, most of whom were also fully vaccinated. However, Hess didn’t develop symptoms until several days later and L.A. is currently experiencing a surge so it’s not clear how it can be known that Hess was the index case for all the other infections. Nonetheless, the fact that most of those infected were fully vaccinated illustrates the lack of protection provided by vaccination.
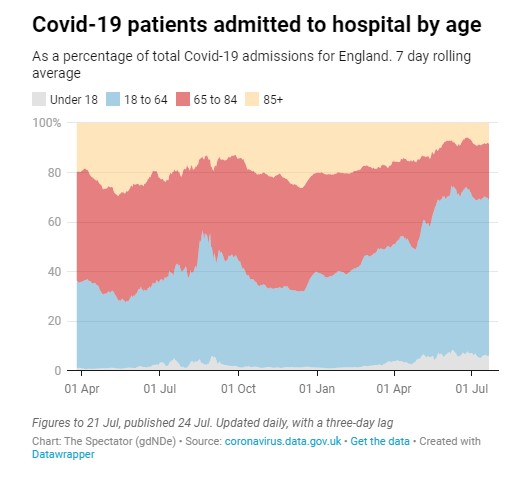
The Swiss Doctor argues that while the vaccines’ effectiveness against infection looks to be fairly weak, effectiveness against serious disease and death is more robust. This can be seen, for example, in the graphs below, where the proportion of hospitalised cases seems heavily dependent on the vaccination coverage (though a confounder may be how large earlier waves were).
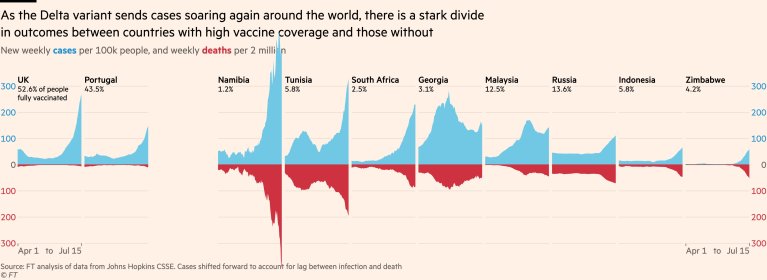
The sharp drop in the proportion of older people being hospitalised since spring in the U.K. (the 65-84 cohort’s share has dropped from 40% to 22% while the 18-64 cohort’s share has grown from 37% to 64%) is also an indicator of protection from serious disease (see below), as older people have higher vaccine coverage.
A recent piece on the Daily Sceptic suggested that evidence from the ratio of the positivity rate to the hospitalisation rate in Scotland shows the vaccines are not reducing serious illness. However, this assumes that there are no confounders in the positivity rate for the recent surge, when in fact there may be, not least the huge increase in mass lateral flow testing since March. This would depress the positivity rate (as more healthy people are being tested even though they are unlikely to have it) and so would give a false impression that the infection-to-hospitalisation ratios of the earlier surges are being matched.
The evidence is now mounting that the vaccines are not as effective at preventing infection as the trials and other early studies indicated, not least the big outbreaks in highly vaccinated countries such as Bahrain, Seychelles, Maldives and Chile. This incidence data is supported by the fact that the vaccines don’t produce mucosal IgA antibodies, which are known to be important in combatting infection in the early stages. However, the vaccines do produce IgG antibodies in the blood and also to some degree a T cell response, which may explain their apparent efficacy against serious disease and death.
Unfortunately, the growing evidence for the lack of vaccine efficacy against infection and transmission is leading many to conclude that vaccine boosters and more restrictions are needed in the face of the Delta and other variants. But this is the wrong conclusion.
The most important conclusion should be that vaccination offers little to no benefit to other people, so no one (least of all children) should be vaccinated in the wrongheaded belief they will protect others. Neither can there be any justification for coercing the population to be vaccinated through vaccine passports and the like, as vaccination is a personal choice that protects the vaccinated person only.
The fact that the vaccines appear to prevent serious disease and death should be sufficient to allow life to return to normal now that all the vulnerable are vaccinated. In truth, even if the vaccines didn’t prevent serious disease we should return to normal because there is no evidence restrictions are effective in reducing infections or deaths. And even if restrictions were effective there is no evidence they do more good than harm. And even if there was such evidence that doesn’t mean the state is entitled so egregiously to suspend the population’s liberties indefinitely to prevent the spread of a relatively mild (fatality rate under 0.1% for most of the population) contagious disease. But those are arguments for another time.
We locked down last winter to wait for a vaccine. Now we have our vaccine, we must return to normal, before lockdown becomes a way of life, and humanity becomes stunted by its own disproportionate fear of disease and death.











To join in with the discussion please make a donation to The Daily Sceptic.
Profanity and abuse will be removed and may lead to a permanent ban.