There follows a guest post from our in-house doctor, formally a senior medic in the NHS, analysing the latest NHS England data packet.
Once a month, the NHS releases a more detailed summary of COVID-19 related data than provided in the regular daily updates. Although the data set is far from complete, the monthly packets provide a better impression of what is really happening in hospitals than the daily snapshot. I find this month’s information particularly interesting. Apologies in advance to readers for reverting to a more data-driven ‘chart fest’ format for my latest contribution – but stick with it, because there are some important messages here which have not been widely reported so far.
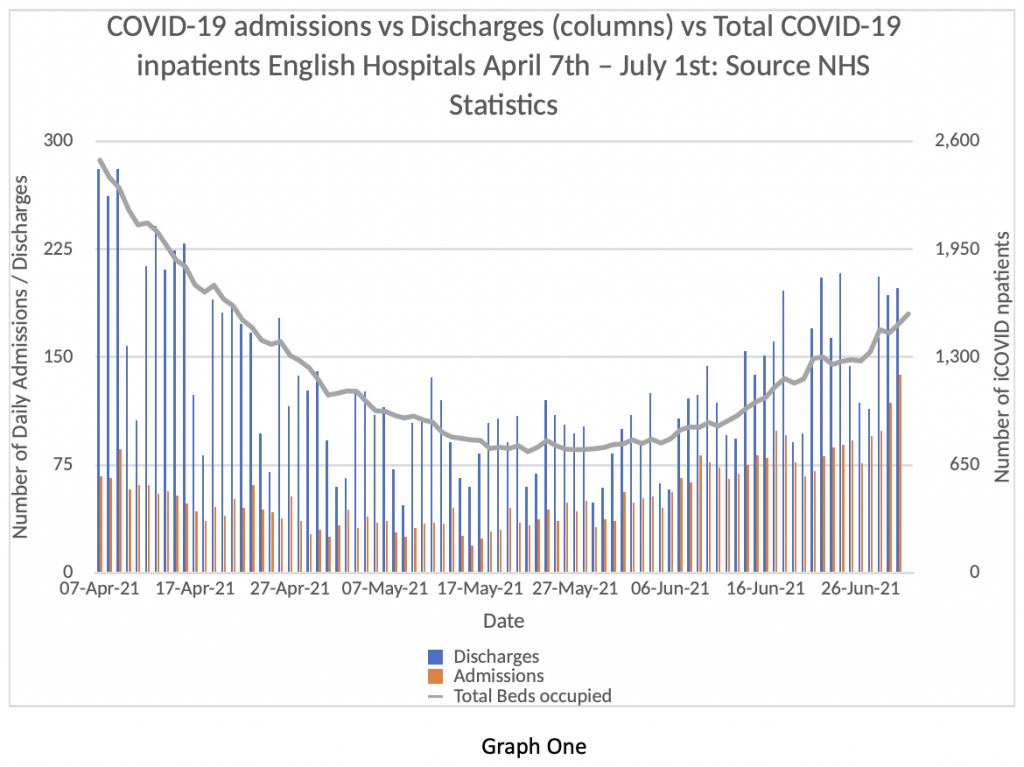
Take a look at Graph One. This rather complicated graphic shows daily admissions in the vertical orange bars and paired daily discharges in the vertical blue bars. Readers will notice that on every day between April 7th and June 30th, there were more discharges than admissions.
The grey line with the secondary y-axis to the right of the chart shows the total number of ‘COVID-19’ patients in hospital on each given day. For the first period from April 7th to May 25th, this was on a falling trend – that’s what one would expect if there were more discharges than admissions each day.
From May 26th to the end of June, however, the total number of patients in hospital ‘with COVID-19’ was on an upward trend – but on each day of the series, there were still more discharges than admissions. How can that be?
I’ve discussed this issue with colleagues and there are only three interpretations we can think of. One is that there are a very large number of patients contracting COVID-19 in hospital who came into hospital without the virus. The second is that some of the ‘discharges’ are in fact patients who were never admitted to hospital at all, but seen in A&E and then sent home. The other is that the data quality is very poor and gives a misleading impression of the true picture.
If the first proposition (a high rate of in-hospital infections) is true, that’s pretty alarming and needs explaining by the NHS. If the second is true – that a high percentage of COVID-19 patients are sent home from A&E – then it should be made clear to the public that the vast majority of patients attending hospital with COVID-19 aren’t even ill enough to warrant admission. If the data is in fact of such low quality as to be uninterpretable, that’s an unacceptable state of affairs at this stage in the process.
I incline to the second explanation – that the majority of discharges are people being sent home after an A&E visit. Figures released today by Public Health England show that only 30% of patients visiting hospitals need to be admitted. That’s the first time I’ve seen this acknowledged, but the NHS must have known about it for months.
Given the continued restrictions on citizen’s rights, the State should be able to provide accurate and detailed information to justify the continued deprivation of liberty. I will return to this point later.
Next, consider Graph Two. We have heard much in the media about the unprecedented pressure the NHS is under with COVID-19 and how worrying it is when cases continue to rise with the Delta variant. Graph Two shows how much pressure the NHS is under with COVID-19 admissions up to July 6th.
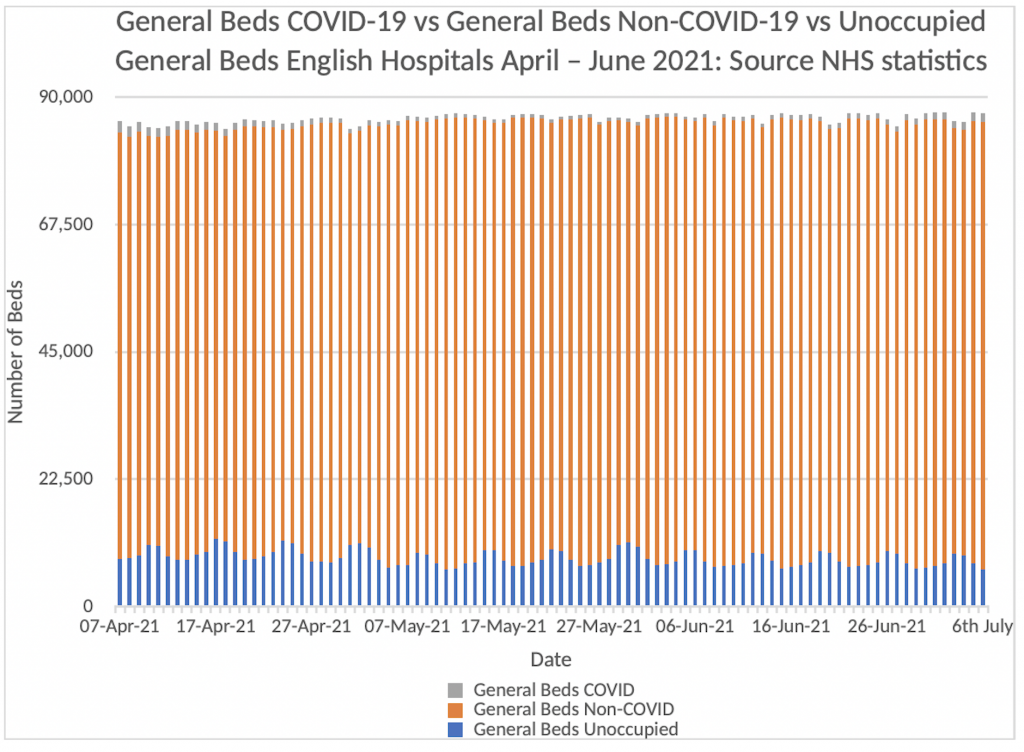
The orange vertical bars that make up the majority of this graph represent the patients in English Hospitals who have NOT tested positive for COVID-19. The Blue bars represent the number of empty beds in the system. The grey bars represent the number of patients in hospital who are COVID-19 positive.
Can you see the grey bars? It’s really quite difficult because they are on top of the orange bars and represent about 1.5% of the total beds available in English Hospitals. At present, we have about 8% of bed capacity spare. Readers can draw their own conclusions about the current “pressure on the NHS from COVID-19” from this graphic. I re-emphasise, these are the official NHS figures released on Thursday July 8th – I am not making this stuff up.
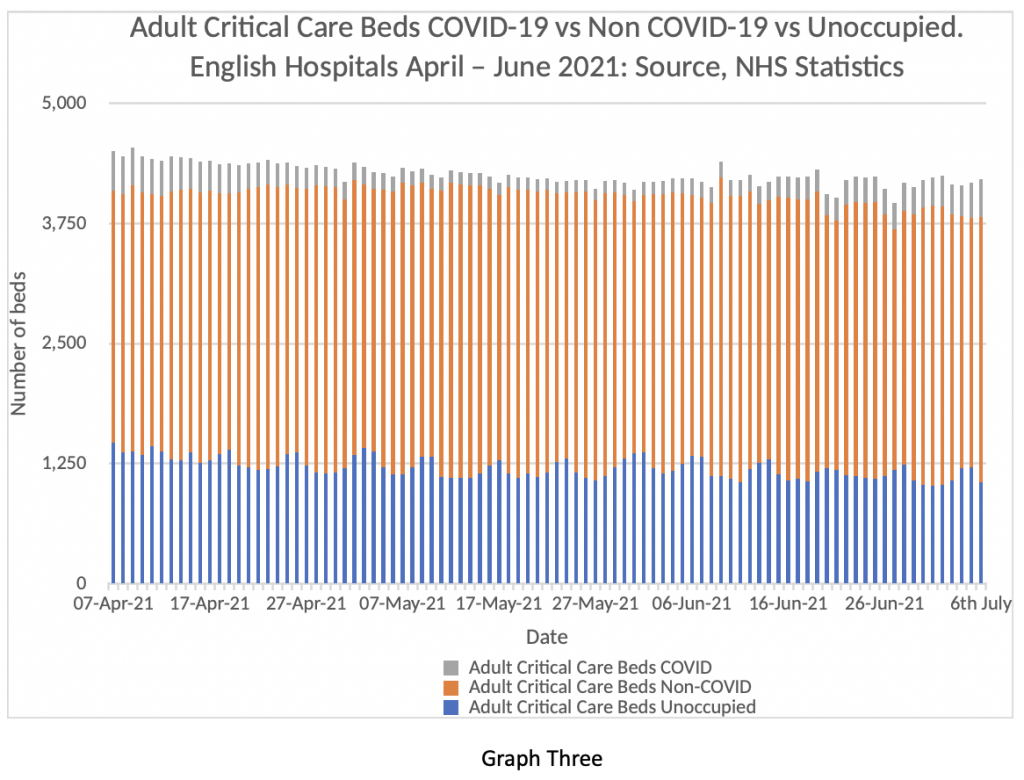
Now consider Graph Three. It’s a similar comparison looking at critical care beds rather than general bed occupancy. Same colour scheme. Blue = spare beds, orange = Non COVID-19 patients, and Grey = COVID-19 patients in critical care. The grey bars are a bit more visible in this graph. For clarity, on July 6th there were 388 COVID-19 patients in critical care in English Hospitals (9%). There were 1,060 spare beds (25%) and 2,761 non COVID-19 patients (66%). That’s a bit more of a strain on the system, but by no means beyond the capacity of the system to cope. Further, when the regional analysis is examined, it is clear that the majority of the burden lies in the North-West and Yorkshire. Leeds in particular has come under strain in the last week and this has been widely reported in the press. However, the situation in Leeds is by no means replicated across the English NHS as a whole – the July 8th data packet shows those areas are outliers and most regions have very low levels of COVID-19 pressure both on general beds and critical care. The PHE figures reveal that of the 1,904 people admitted to hospital in this period, 1,557 (82%) were unvaccinated or had only had one dose. Just 4% of cases had been fully vaccinated with a two-week gap for the effect of full immunity to develop.
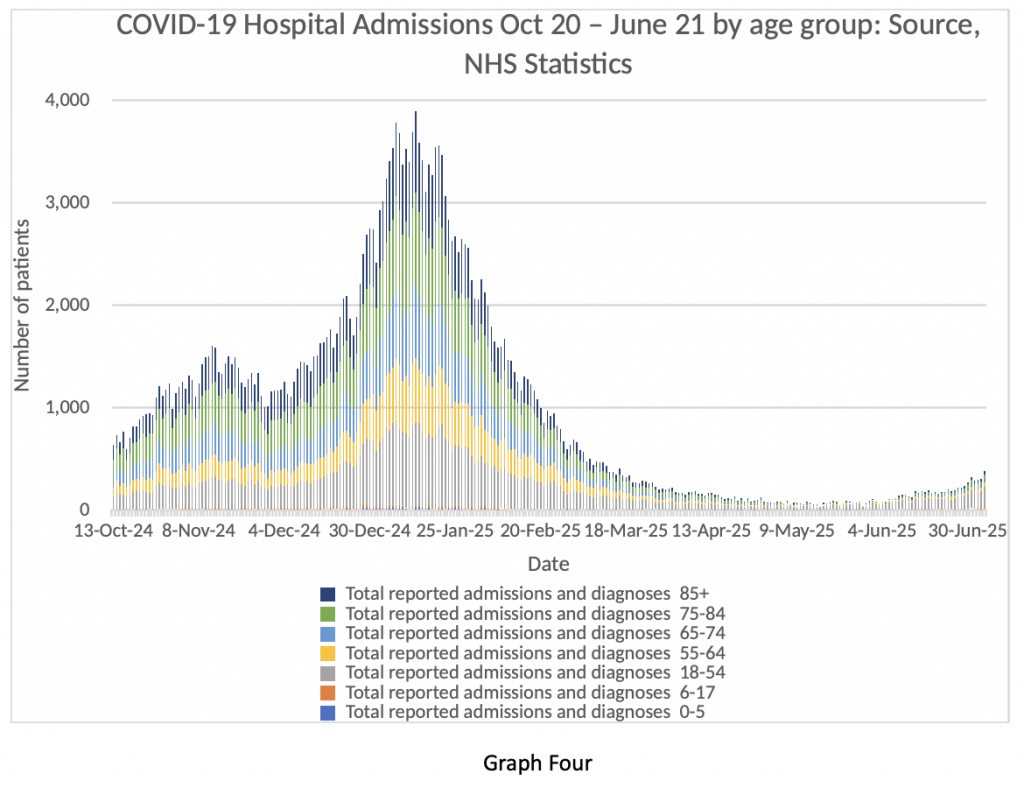
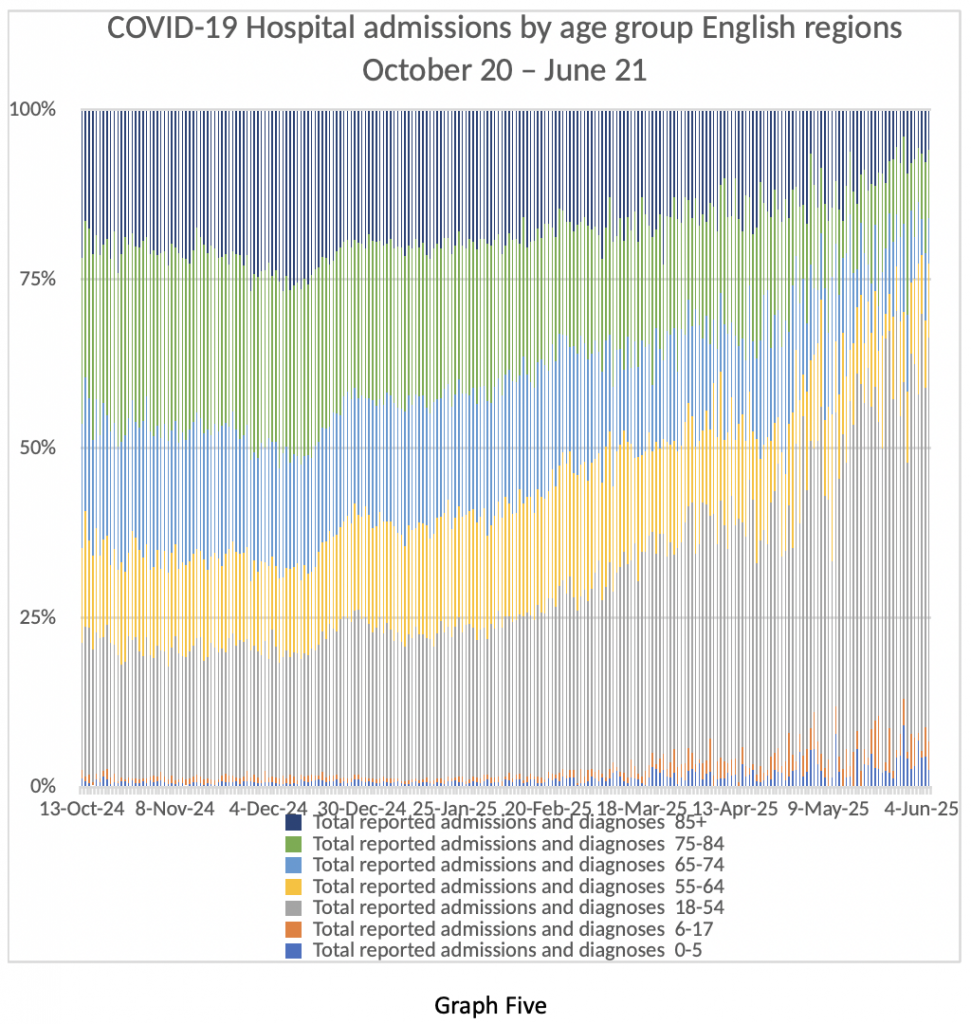
Let’s have a look at Graph Four next. It shows the age breakdown of COVID-19 inpatients from October 2020 to the beginning of July 2021. Quite a ‘busy’ graph, so I will explain. Look at the winter peak, which is obvious. A big spike in dark blue, green, light blue and yellow bands. Those are all patients in the age bracket 55-85+.
Now look at the extreme right-hand side of the graph. That’s the current situation. Very few admissions for the over-55s. What that translates into is shorter lengths of stay in hospital, less demand on critical care, and very few deaths as a result of COVID-19.
Graph Five shows the same data in a slightly different way – age bands of admitted patients as percentages over the same time period. The same point is quite obvious. Older patients who are more likely to be very ill and far more likely to die are being admitted in fewer numbers than in the winter or last spring. Younger patients have milder illness, spend less time in hospital and are very unlikely to die from COVID-19. Further comment is not required.
Finally, I invite readers to consider Graph Six. This graph looks at people taking time off work from their NHS jobs between April 7th and June 30th. The blue bars represent people taking time off due to COVID-19 related absence – that means either showing symptoms of COVID-19 themselves or having come into contact with someone with a positive COVID-19 test. The orange bars represent people taking a day off from their NHS work for non-COVID-19 related reasons.
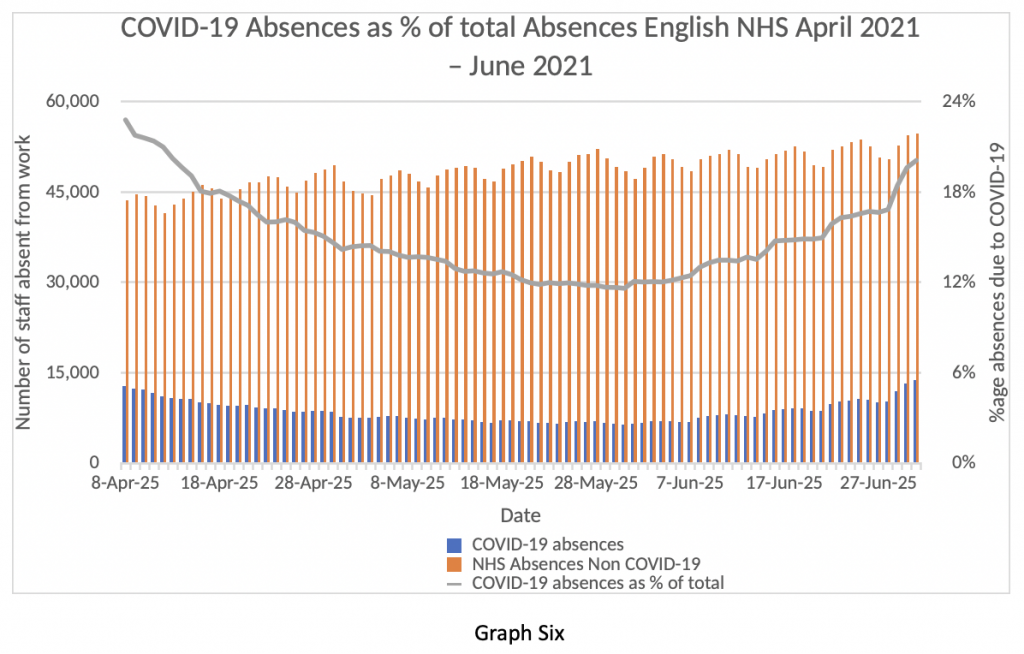
My first observation is that about 50,000 people per day are absent from their jobs in the NHS – that’s about 4% of the total workforce absent every day because of illness – in the middle of summer. Twenty per cent of those absences are “because of COVID-19” – although, actually, they are not “because of COVID-19”. The vast majority of NHS staff are fully vaccinated – so the vast majority of these absences are caused by the Test and Trace rules, not by actual Covid infections.
As I write, the papers are reporting that NHS employees are about to be made exempt from self-isolating if identified as coming into contact with a positive ‘case’. How can the government justify this, while maintaining restrictions for other citizens?
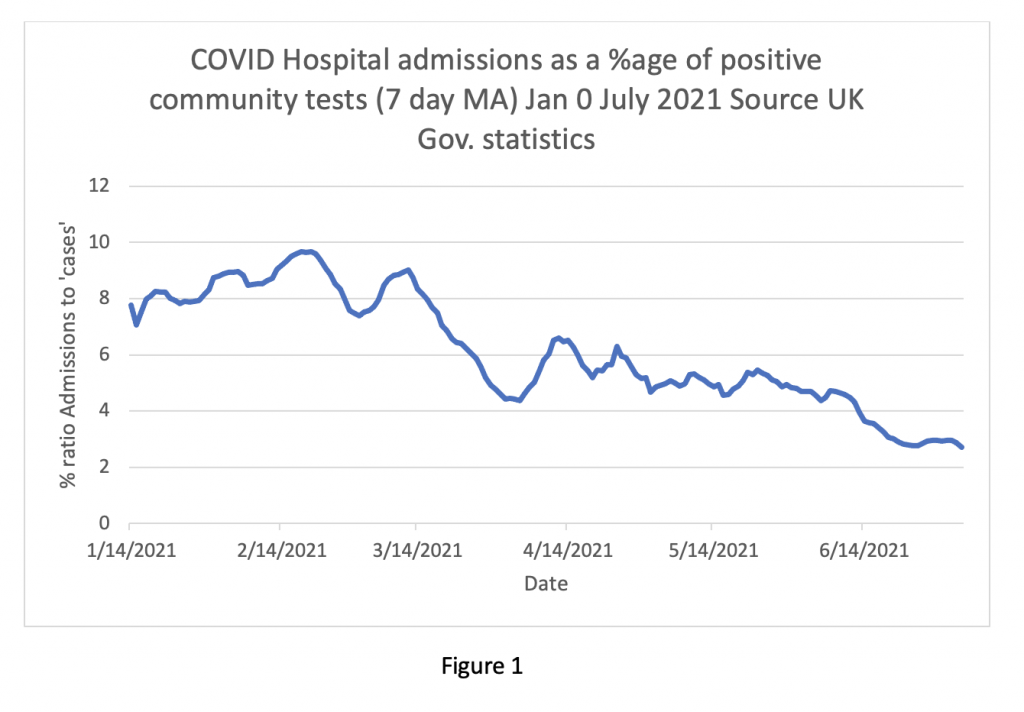
My overall impression of the current data so far is that the ‘Third Wave’ of COVID-19 is much less of a problem than the first two waves. The ratio of admissions to positive tests has fallen from nearly 10% in February to lower than 3% currently (see Figure One below). The vast majority of positive tests are asymptomatic. The symptomatic cases are milder and the majority of patients attending hospital are sent home from A&E. Those admitted have shorter lengths of stay, fewer people need intensive care and deaths are infrequent.
Yet everywhere in the media, warnings of imminent catastrophe from experts on various Government bodies continue to be broadcast. Why?
Am I wrong in my assessment? Is there crucial information I’ve overlooked? Are we about to be suddenly and unexpectedly overwhelmed by a new scary variant with teeth and claws? I’ve been in clinical medicine long enough to know that surprises happen from time to time, but, usually, if all the objective information points one way, then the direction of travel is pretty obvious.
So, what is really going on? Much ink has been spilled hypothesising about the Government’s hidden agenda, as well as that of their advisors, and these theories will be familiar to readers already.
The fundamental problem is the relationship between the NHS, the public and our elected representatives. If the public is encouraged to venerate a taxpayer-funded institution to the extent that it becomes immune to criticism and unresponsive to change, eventually that organisation will become a law unto itself. Elected representatives will be incapable of controlling it. In effect, it becomes a “state within a state”, hungry for an ever-greater share of national resources, resistant to attempts at reform, and keen to exert control over the population.
Contrary to the often-repeated assertion that the U.K. spends less per capita on health than any other European country, when private-sector figures are added in, we spend about the same as our continental neighbours, which all have “mixed health economies”.
The starkest measurable difference between the NHS and our peers in developed countries is in health outcomes – consistently at the bottom of league tables in waiting times, cancer outcomes and other critical areas. The domain in which we really stand out is remuneration – doctors pay in the U.K. is higher than most other European nations. In short, the British taxpayer gets very poor value from a monopolistic state-run healthcare provider. Why is anyone surprised?
NHS talking heads are already changing the narrative, now focusing on waiting lists, the spectre of “long Covid” and a resurgence of familiar respiratory pathogens like influenza to justify extended coronavirus restrictions. I expect the Government to be bounced into reimposing curbs on liberty in the autumn to protect a failing institution that has, objectively, performed poorly and continues to perform poorly in a time of crisis.
It may seem remarkable to Lockdown Sceptics readers, but, to paraphrase Professor Ferguson, I also expect the NHS to keep on getting away with it.












To join in with the discussion please make a donation to The Daily Sceptic.
Profanity and abuse will be removed and may lead to a permanent ban.