Professor Tim Spector, who leads the ZOE Covid Symptom Study, has done a new video update on vaccines, which is worth a watch. The team has also published a new study (not yet peer-reviewed) about the vaccines and their effect on symptomatic Covid.
The data is broadly encouraging in terms of efficacy. (They don’t address safety, though a previous study did. They also exclude the period immediately after each vaccine dose, so the study tells us nothing about any post-jab spike in infections, which is disappointing.)
One interesting finding is that sneezing becomes more common as a symptom of Covid infection after vaccination than beforehand, which the authors suggest could be a result of our immune system reaction changing. They note this could make the disease more infectious owing to the additional aerosols produced.
A concerning finding was that the elderly (over-60s) were up to three (2.78) times more likely to be infected after being vaccinated (with one dose of any vaccine) if they were frail than if they weren’t. This is unsurprising perhaps, but still indicative of considerably lower protection for those already at higher risk from the disease. Furthermore, a quarter of the vaccinated frail elderly in the study who contracted the virus ended up in hospital, which is not a small proportion (though no figure was given for the hospitalisation rate of unvaccinated frail elderly people against which to compare it).
Vaccine efficacy was also reduced in the obese, another high risk group, and those with an unhealthy diet – see charts below. The baselines are people who are also vaccinated and otherwise similar, but without the particular characteristic mentioned, e.g. the point in the top right shows the additional risk of infection that the vaccinated frail elderly have versus the vaccinated non-frail elderly.
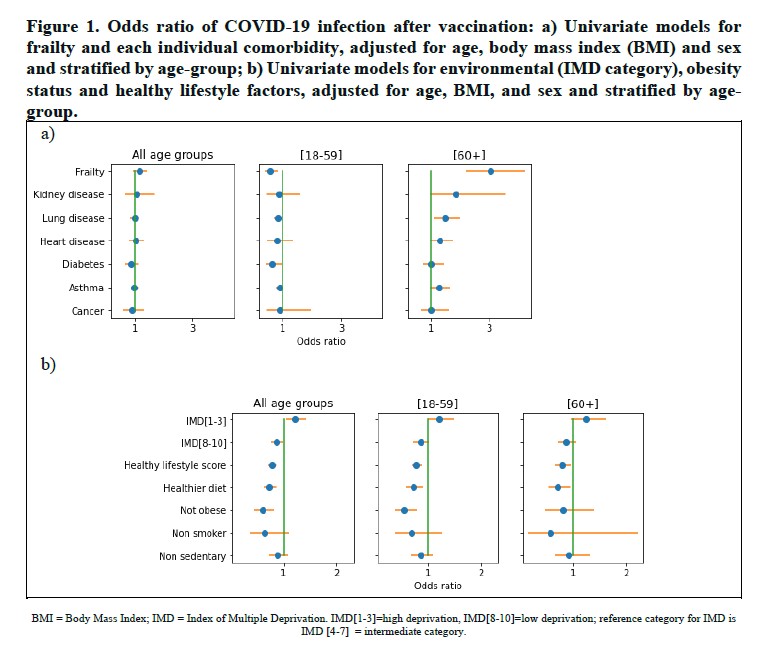
The authors note this means the vaccinated high risk, especially the frail elderly, are still susceptible to infection and serious disease. However, they did find that vaccination cut the general risk of hospital admission by 64% and increased the chance of being asymptomatic by 72% once infected. Infections in vaccinated people were also around half as likely to have more than five different symptoms. Similarly, in infections in vaccinated people, most symptoms were around half as likely to appear (see chart below).
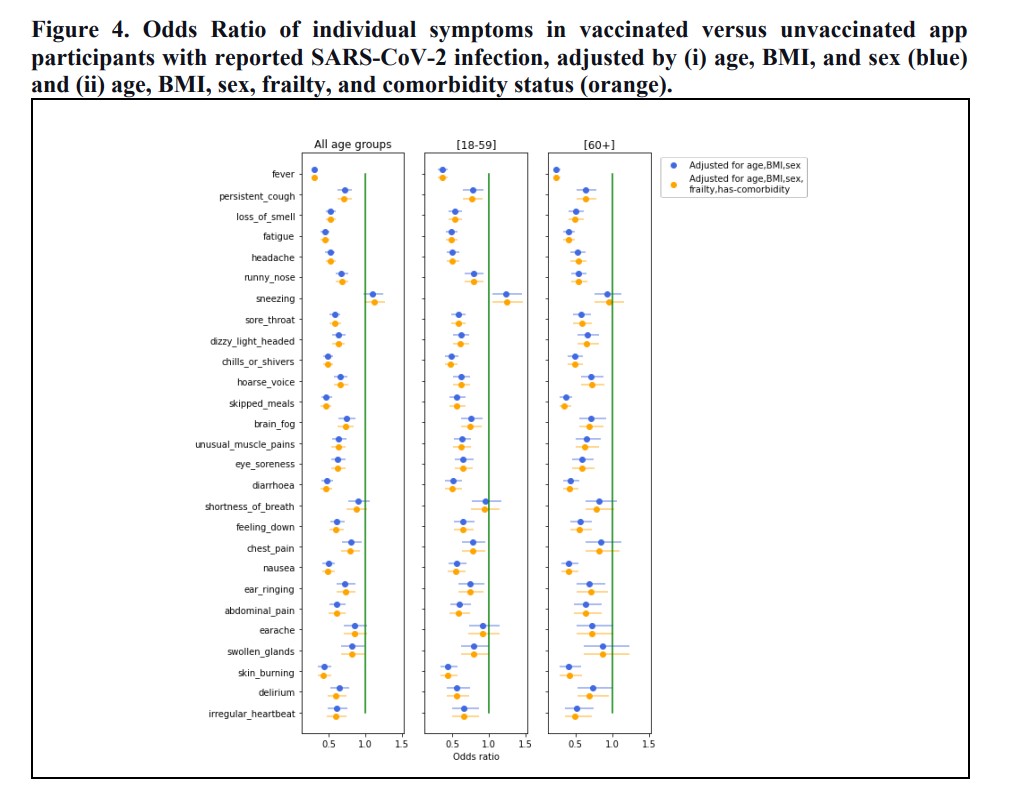
A graph shown as part of this week’s video also gives us a glimpse into the vaccines working almost in real time.
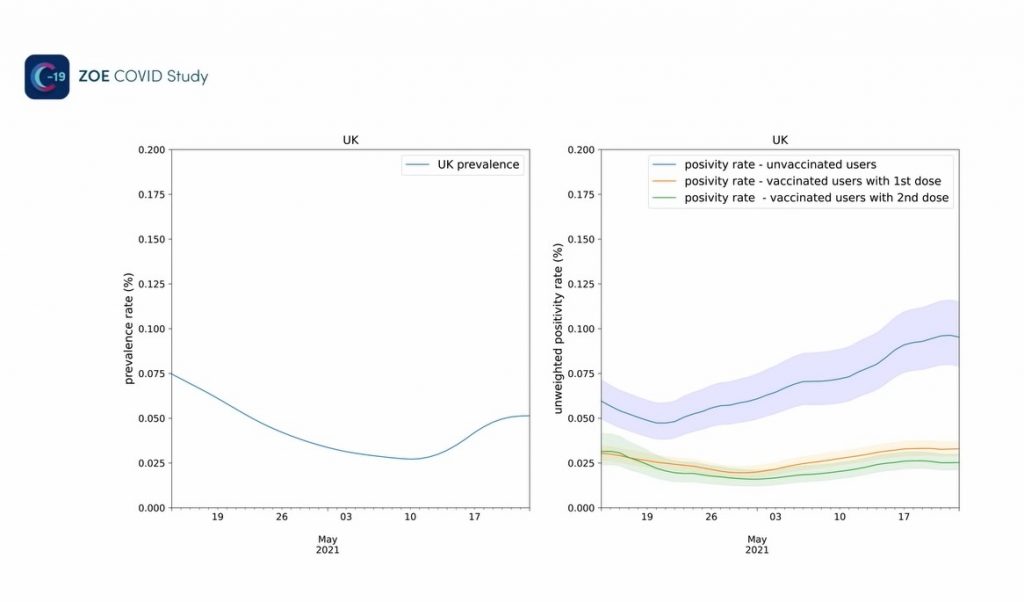
The positivity rate for the unvaccinated here peaks around 0.095% while for the fully vaccinated it peaks around 0.025%. It’s tempting to estimate vaccine effectiveness from those figures (74%) but actually we can’t do that because the data is unweighted, so doesn’t take into account, for instance, that the vaccinated are generally older and the infection rate in older people is usually lower so the vaccine effectiveness would be overestimated. At such low prevalence, false positives also become a big problem, leading to vaccine effectiveness likely being underestimated due to a higher proportion of the infections in vaccinated people being false positives.
Nonetheless, the curves are at least the right way round, with infections in the vaccinated not rising anywhere near as much as those in the unvaccinated in the recent small hump.
This is relative risk, of course. Absolute risk when prevalence is this low is miniscule.
I confess I was rather hoping that the ZOE data would shed a bit more light on vaccine effectiveness than it has done to date. The team have done one study looking at effectiveness in terms of preventing infection, but only after one dose, and like so many of these studies it is confounded by the declining background prevalence so does not give a reliable estimate of vaccine effectiveness.
Which is frustrating because I still don’t feel I can point to a study and say there, that gives a really reliable estimate of how well the vaccines work. There are lots of tantalising hints the vaccines are working well, in terms of preventing infection and serious disease (safety is a separate matter). But it’s not clear exactly how well, once you take out the fact that infections decline anyway. The effectiveness in the high-risk frail elderly also continues to give signs of being lower than we might have hoped given how susceptible they are to the virus.
As Peter Doshi wrote in the BMJ in January – more data please.











To join in with the discussion please make a donation to The Daily Sceptic.
Profanity and abuse will be removed and may lead to a permanent ban.