There follows a guest post from our in-house doctor drawing on his long experience of working in NHS hospitals to explain why the NHS won’t be resuming normal service for a good while yet. Some of the problems it’s facing were unavoidable, but others were of the NHS’s own making.
In this week’s update, I’m deviating from my usual format of assessing Covid hospital data published by the NHS. It is clear to any objective analyst that we are on the downslope of the Omicron wave, which has fallen far short of predictions by epidemiological experts. Over half of all patients with positive Covid tests in English hospitals do not have Covid as the primary reason for admission, and this proportion has been rising steadily since the new year. There is no reason to believe this trend won’t continue.
This week I turn to the ‘recovery phase’ – where the NHS tries getting back to business as usual. Readers will be wearily familiar with senior NHS figures appearing on the media lamenting the unprecedented pressure the NHS faces. As with many facets of the information space over the last two years, this is partly true. The NHS is under unprecedented pressure – but much of that pressure is self-generated and self-perpetuated, arising from the structure of the system, or from choices made by management.
In this article I will put forward 10 reasons why the machine will not fire on all cylinders for some time, if ever. This is a subjective and observational analysis, not backed up by published data and open to challenge. Some of my points relate to cultural change, where data is hard to collate. On other points, internal data does exist but will never be widely shared or published. I hope this piece will help readers understand why we are where we are – and help them to decipher official announcements in the coming months.
- Loss of efficiency due to Covid protocols: Regulations in respect of Covid testing and periods of self-isolation before surgery are hampering efforts to restore normality. Operating Theatre utilisation rates in many trusts are running at 70% capacity. If a patient tests positive for Covid and is cancelled at short notice, it is not possible to fill the slot because waiting patients don’t fulfil the self-isolation criteria. So, the theatre slot remains empty and is wasted despite the huge backlog.
- Poor management of chronic conditions in the community: Many patients arrive for surgical pre-assessment ill prepared for an operation. This causes postponement and short notice cancellations. The need to optimise poorly controlled underlying conditions before surgery consumes yet more medical resources. In normal times, chronic disease management is the function of the Primary care sector, i.e. GPs.
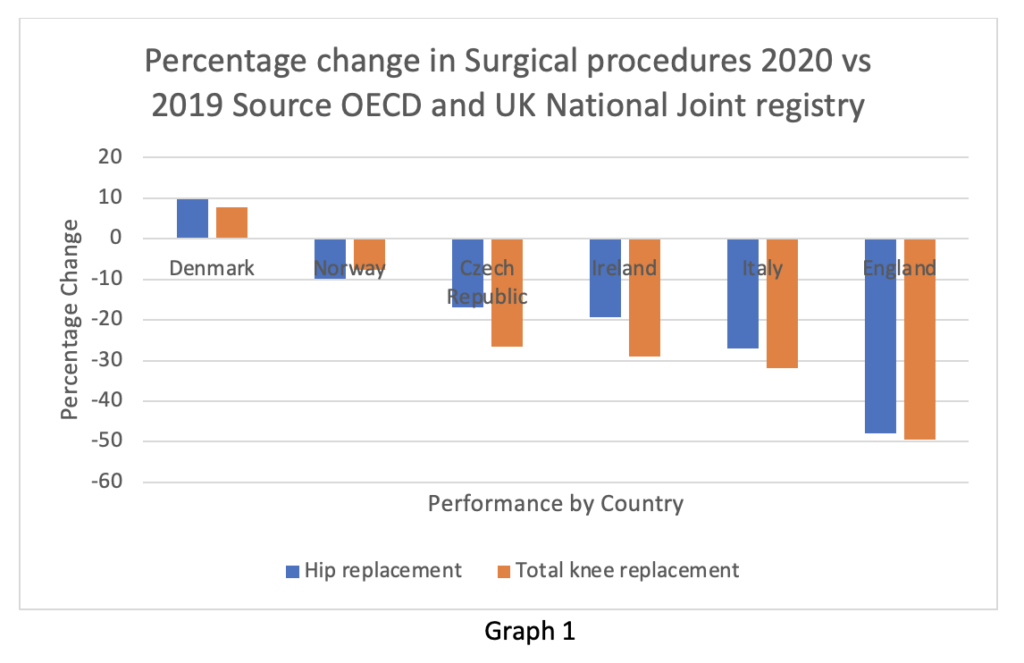
I can’t resist using at least one graphic this week. Graph 1 (reproduced from the Spectator) shows the change in procedure volume for hip and knee replacements in various European countries. The data is from 2020 and not complete, but it is a reasonable approximation of the trend. Readers may wonder why England seems to perform badly in comparison to our peers when the NHS is the envy of the world.
- Cohorting of patients: In 2020 discussions took place about how best to minimise in-hospital transmission of Covid. At the time, these were very reasonable concerns. Broadly speaking, the options split into admitting Covid patients only to specifically designated hospitals, or admitting Covid patients to all hospitals but separating them into specially controlled areas. The latter solution was preferred. Accordingly, most hospitals now have green, amber and red zones depending on the testing status of each patient. Patients testing positive for Covid while in hospital therefore need to be moved into Covid only ‘red wards’, while negative patients are in green zones and patients waiting for results in amber. When moving patients around hospital (on trips to the radiology or endoscopy department, for example), infection control protocols are mandatory. Zoning regulations play havoc with specialist nursing rotas and are in any event of questionable effectiveness in reducing in-hospital spread of Covid. With the advent of the much less dangerous Omicron variant and the knowledge that over 50% of patients have incidental Covid (plus the reasonable expectation that this percentage will continue to rise), there is a good argument for scrapping this system. Nevertheless, it will be hard to revert to normal practice any time soon, for reasons I expand on below.
- Cultural shift in relation to ‘safe working’: This metric is hard to measure, but I am convinced ‘safetyism’ is a real phenomenon. By inculcating a culture of fear in the workforce about the risk of catching Covid, friction is introduced into every facet of normal organisational function. Simply put, everything takes longer than it should because of restrictive protocols imposed by infection control departments stemming from an overabundance of caution. The ostensible and commendable purpose is to reduce the spread of in-hospital infection. The side effect is to make routine tasks like wading through treacle – everything takes longer, so fewer patients can be processed per unit of time. The overall effect is similar to throwing a handful of sand into a gearbox.
- Exploitation of ‘safe working’ by health unions: Readers will be familiar with trade unions exploiting ‘health and safety’ regulations in industries other than health. The long running dispute between the RMT union and South Western Railway about the necessity for guards on trains is one example. Arguments about provision of PPE, enhanced rest periods for staff and extended periods of sick leave do have a rational basis, but trade unions push legitimate concerns to extremes and are frequently antagonistic to management. Such behaviour exacerbates the general difficulty in returning to business as usual. The British Medical Association is frequently the most egregious transgressor in this area. Institutionally left wing, its main purpose appears to be permanent opposition to the government of the day rather than supporting coalface clinicians in delivering best medical care.
- Difficulty in discharging patients from hospital: The phenomenon of ‘bed blocking’ is well known in the NHS and the reaction to Covid has exacerbated the problem. Care homes are still licking their wounds from spring 2020 when the NHS forcibly discharged patients known to be infected with Covid into the care system. Unlike the NHS, most care homes are privately run entities, and not protected by Crown Indemnity from risk of prosecution. Not surprisingly, many homes are reluctant to take previously Covid positive patients from hospitals. Workforce shortages in the care sector, worsened by vaccination mandates, add to the problem. As a consequence, the number of ‘purple patients’ continues to mount – designated medically fit for discharge but stuck in a hospital bed. But there are still not enough of them to require housing in the temporary Nightingale facilities, which remain largely empty.
- Vaccine mandate antagonism: The mainstream papers are reporting today that the vaccine mandate for healthcare workers is about to be scrapped – if true, this is excellent news. If someone was actively trying to mess up the healthcare system, I can’t think of a better way to do it than forcing workers to take a drug they believe to be unnecessary. For clarity, I am fully vaccinated and boosted because I consider it reduces my personal risk of becoming seriously ill with Covid. On the other hand, I completely understand colleagues who take a different view. The data shows that vaccination does not prevent transmission of the virus, hence I don’t understand how vaccinated staff pose less of a risk to patients than the unvaccinated. Regardless of the data, the issue has provoked serious conflict between individuals and between staff and management in the health service, which will persist long after the argument has been resolved and the mandate binned. In a team sport like healthcare, this has profoundly adverse effects. The vaccine mandate plan will not have been conceived by politicians, but probably within the U.K. Health Security Agency. The faceless medical bureaucrats responsible for this policy really should have the courage to explain themselves in public – I won’t hold my breath.
- Long Covid: Post viral fatigue is a well-known phenomenon. It usually resolves within a few weeks. Long Covid is probably a variant of this. The symptoms attributed to ‘Long Covid’ are legion. Unfortunately, in the absence of a specific objective test for the condition, the diagnosis is purely clinical and largely made on the basis of self-reported, non-specific symptoms by the patient. A recent study from Oxford using xenon to track gas exchange in the lungs has suggested some abnormality in gas transfer in a small number of patients, but the precise mechanism and characterisation of ‘Long Covid’ remains opaque. The potential for exploitation is obvious and requires no further comment.
- Workforce ‘enthusiasm fatigue’: A grumbling workforce in the NHS is nothing new, but the last two years have worn many of the best people down. Fresh haranguing by managers to meet arbitrarily-imposed targets in the face of even more pointless regulation reinforces a sense of institutional indifference. Many employees have become demotivated and sullenly resistant, choosing to do the bare minimum rather than resign or retire. Achieving unprecedented productivity gains in these circumstances is probably unrealistic.
- Workforce shortages: Workforce shortages in critical skill sets has long been a problem in the NHS. Covid has accelerated this trend by precipitating early retirement among senior staff, incentivising career changes for those considering it anyway and encouraging some highly skilled staff such as ICU nurses to seek redeployment into less stressful specialties. I understand applications to study medicine and nursing have risen recently – attributed to the crisis inspiring young people to contribute to their communities. This is welcome, but one should point out the very long lead time between enrolling on a course and becoming an experienced clinical decision-maker (minimum 15 years in most medical specialties). I’d be surprised if the rate of new entrants compensates for the brain drain at the other end of the age spectrum.
I apologise to readers for a fairly dismal and dense piece today. I do believe these points to be an accurate summary of the challenges faced by coalface clinicians in their efforts to retrieve the situation. None of these issues will be widely aired in the mainstream media. The extent to which we ‘learn to live with Covid’ will depend not only on lifting of restrictions on wider society, but on liberating real doctors and nurses from burdensome and pointless professional regulations. Based on my prior experiences, I’m far from optimistic at this point.












To join in with the discussion please make a donation to The Daily Sceptic.
Profanity and abuse will be removed and may lead to a permanent ban.