An important pre-print was published last week by Public Health Scotland looking at how all 204,913 people eligible for shielding (the “clinically extremely vulnerable”) – about 3% of the population – have fared during the COVID-19 pandemic. The researchers matched all 160,307 positive cases of COVID-19 (as of January 28th) to individuals in Scotland to form a complete picture of the course of their illness in order to evaluate the effectiveness of the shielding programme.
Their striking conclusion was they found “no evidence that the shielding programme per se reduced COVID-19 rates”, though they allowed for the possibility that “without shielding advice and support the outcome in this group would have been worse”.
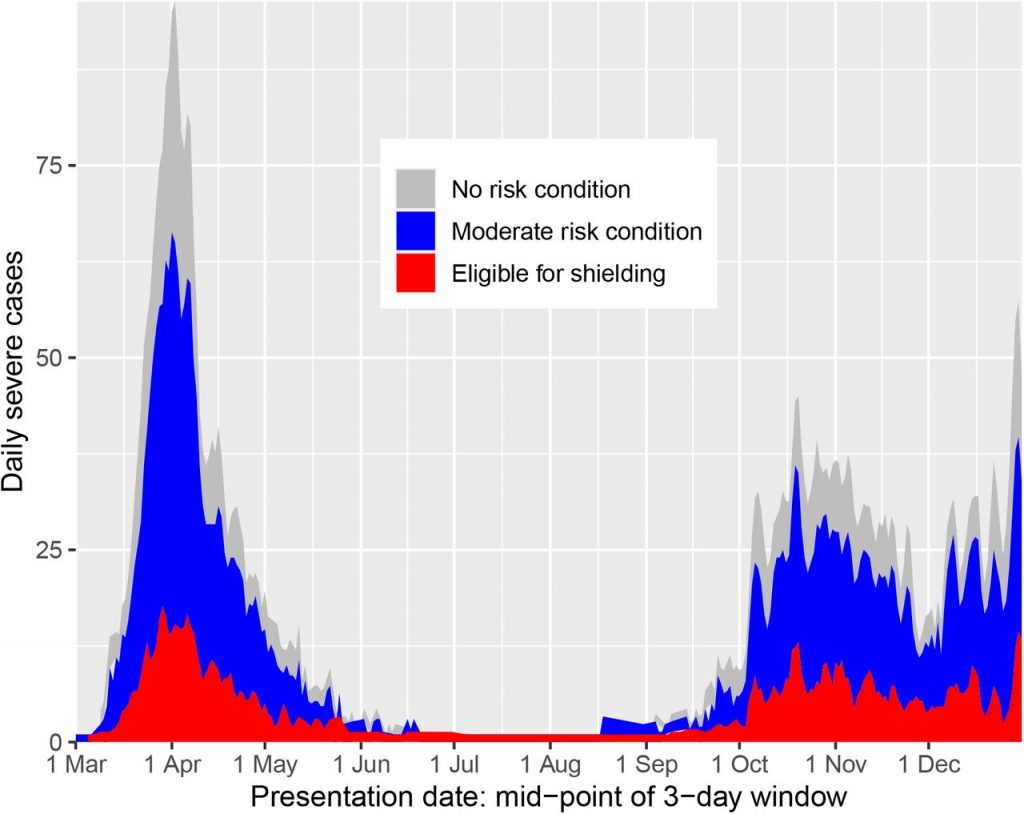
People eligible for shielding were 7.6 times more likely to have a severe case of COVID-19 (defined as requiring intensive care or dying) than the general population with no risk condition (care home residents were excluded from the analysis). This rose to 13.6 times more likely in solid organ transplant recipients (whose immune systems are suppressed by drugs to assist acceptance of the transplant).
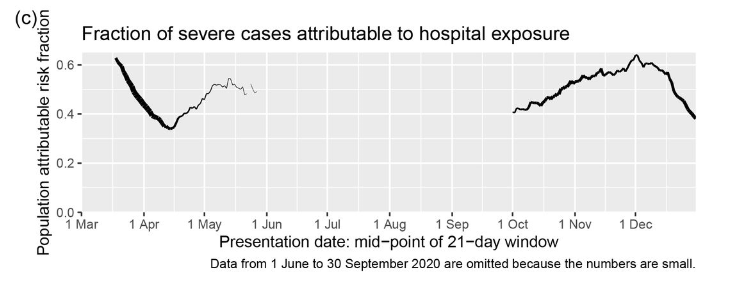
The main problem for shielding was the high rate of infection acquired in hospital, an environment the clinically extremely vulnerable can scarcely avoid. Thirty-six percent of severe Covid cases among this group were linked to recent hospital exposure. This compared to around 50% of severe cases in the general population, peaking at 64% or almost two thirds in December (see graph above). Sharing a household with other (non-shielding) adults was also a major risk factor – again, hard to avoid.
They write:
We have identified two sources of exposure that are associated with severe disease and cannot easily be avoided by those advised to shield: in-patient hospital care, and sharing a household with other adults. We recommend that consideration should be given to special measures to allow these vulnerable individuals to reduce their exposure. This could include special measures to protect these individuals from nosocomial infection, and support for other household members to co-isolate with the vulnerable individual.
The study shows once more the extent to which COVID-19 is a disease caught in hospital, particularly those who have a severe course or die. Since we know from elsewhere that up to 40% of Covid deaths are among care home residents, infections acquired in hospitals and care homes, when added together, account for a substantial majority of COVID-19 deaths. This helps explain why lockdowns, despite the intuitive logic of keeping people apart, are consistently found to have little or no relationship to mortality or infection rates.
The study also underlines the challenges of focused protection of the vulnerable as advocated by the Great Barrington Declaration, with shielding even under lockdown conditions proving difficult. On the other hand, by showing that lockdowns don’t help (and elucidating why), it makes plain that resources should be put into protecting the vulnerable as far as that is feasible and not into confining the healthy population.











To join in with the discussion please make a donation to The Daily Sceptic.
Profanity and abuse will be removed and may lead to a permanent ban.