The latest quarterly report of the Mortality Monitor from the Institute and Faculty of Actuaries, with data to the end of September, brings some encouraging news and some worrying news. The encouraging news is that it shows overall mortality for 2021 so far is about average, meaning Covid has not yet managed to cause more people to die in 2021 than in a typical recent year. The worrying news is that, despite this, mortality in the under-65s is significantly elevated, and it’s not immediately obvious why.
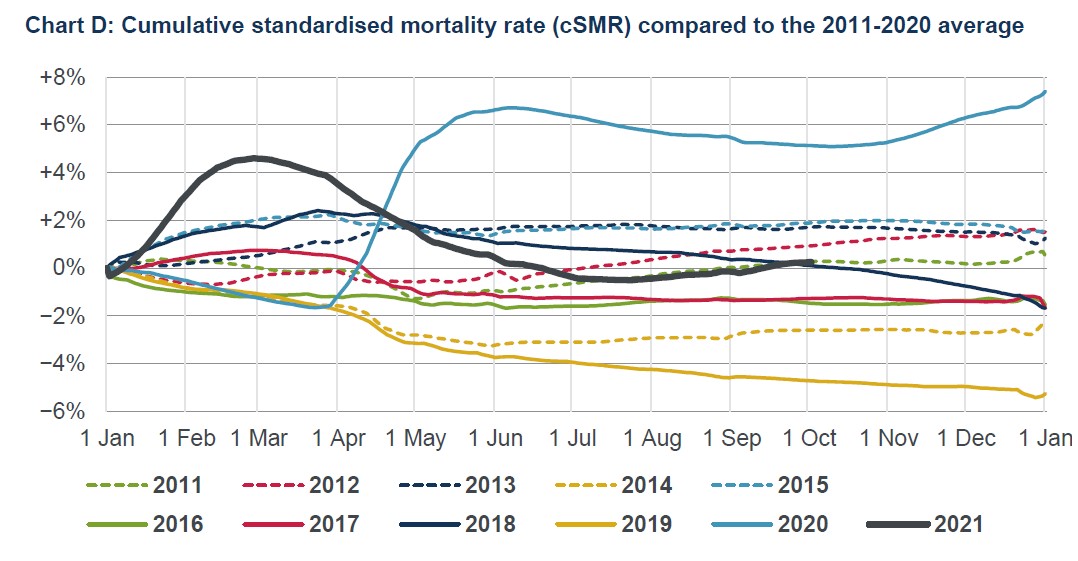
The Mortality Monitor provides graphs and data for the cumulative age-adjusted mortality for England and Wales in 2021 compared to the 2011-20 average. This is a curve that starts at zero on January 1st each year, rises each week that there is above average mortality and falls each week there is below average mortality (see above). It rose at the start of the year during the winter Covid surge then fell as mortality dropped below average in March until, by mid-June, 2021 had below-average cumulative mortality. It started rising again at the end of July, and by the end of September had reached 0.3%, so about average. Note that the 2011-20 average includes the high mortality of 2020, but also the low mortality of 2019. Adjusting the mortality for age ensures that the ageing population is taken into account.
However, while overall mortality is about average, there are big differences by age. Mortality for over-65s is below average (which drives the overall trend, as the large majority of deaths occur in the over-65s), but mortality for under-65s is significantly elevated.
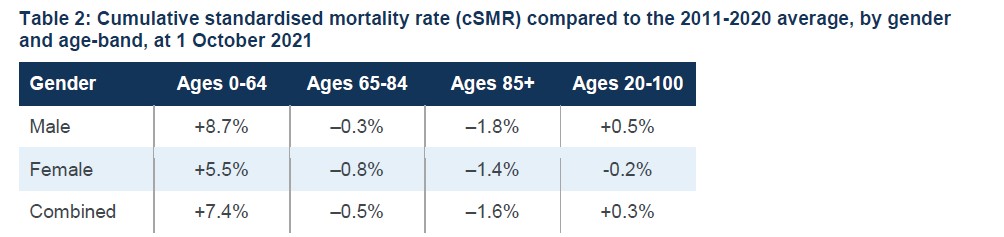
Cumulative mortality is running below average in those aged 65-84 at minus-0.5% and in those aged over 85 at minus-1.6%. But in those aged under 64 it is significantly up at 7.4%.
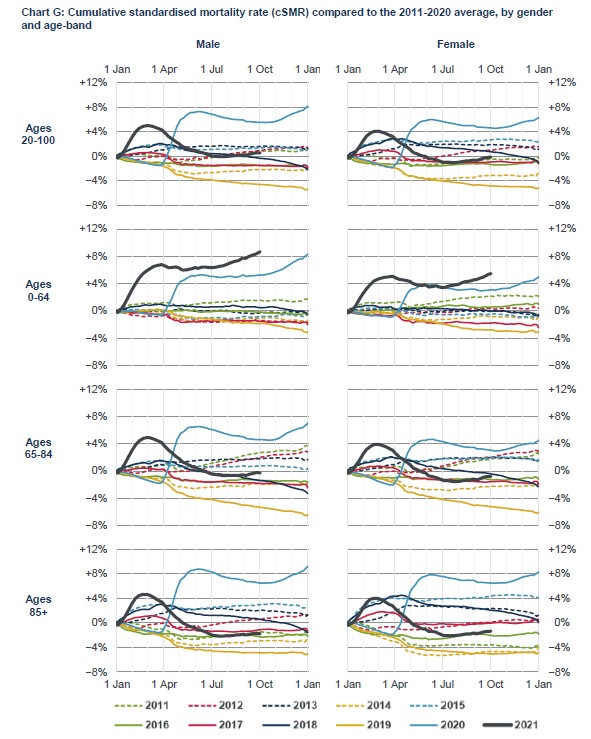
Why is cumulative mortality below normal in the over-65s but elevated in the under-65s? What is killing younger people but not older people? Could it be Covid?
I’ve plotted below ONS data showing excess mortality for England and Wales (using 2015-19 as the baseline and with no adjustment for age) with a breakdown between Covid and non-Covid.
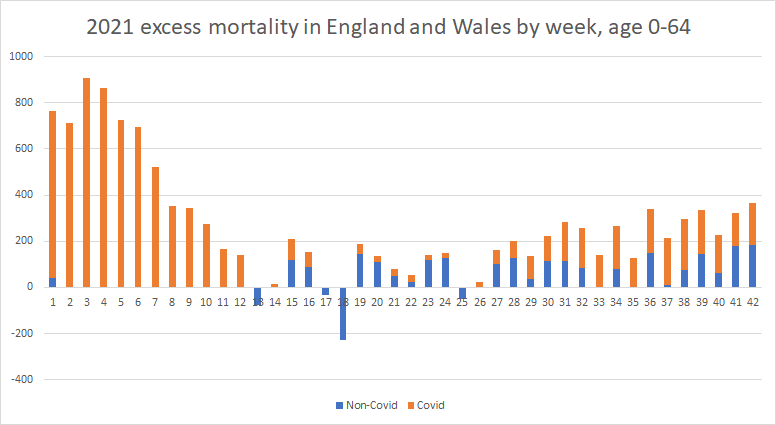
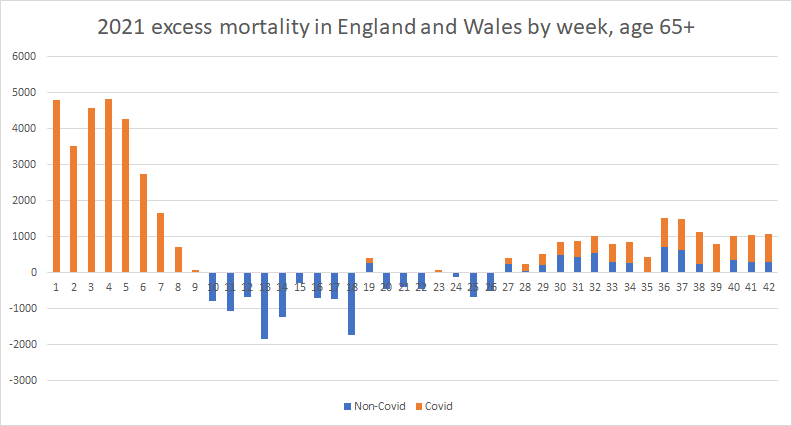
We can see that excess mortality fell more quickly, went lower, rose more slowly, and stayed lower in those aged over 65 than under 65. Covid is credited with around two thirds of the excess since week 27, while just over a third of the excess is non-Covid – since week 27, 1,464 of 3,896 excess deaths in under-65s, or 38%, are non-Covid, while in over-65s, 5,086 of 14,047, or 36%, are non-Covid.
Once these are adjusted for age in the IFA’s figures (and with the 2011-20 baseline), the excess in the over-65s becomes, as we have seen, sub-zero, while the excess in the under-65s remains significantly elevated at 7.4%.
Why are both Covid and non-Covid causes of death having a disproportionately large impact on under-65s? The impact of Covid seems unlikely to be because of the later rollout of the vaccines, as the difference has only become larger as the vaccine rollout has completed in the younger age groups. The lower total vaccine take-up in the younger age groups may be part of the explanation, as might deaths due to missed healthcare and other health impacts of lockdown. Have adverse reactions to vaccines played a role?
While the average overall mortality, driven by below-average mortality in the over-65s, is something to be glad about and a salutary reminder that the pandemic is not causing an elevated loss of life in 2021, the high mortality in the under-65s is concerning. The Government should make a priority of investigating the causes behind this.











To join in with the discussion please make a donation to The Daily Sceptic.
Profanity and abuse will be removed and may lead to a permanent ban.