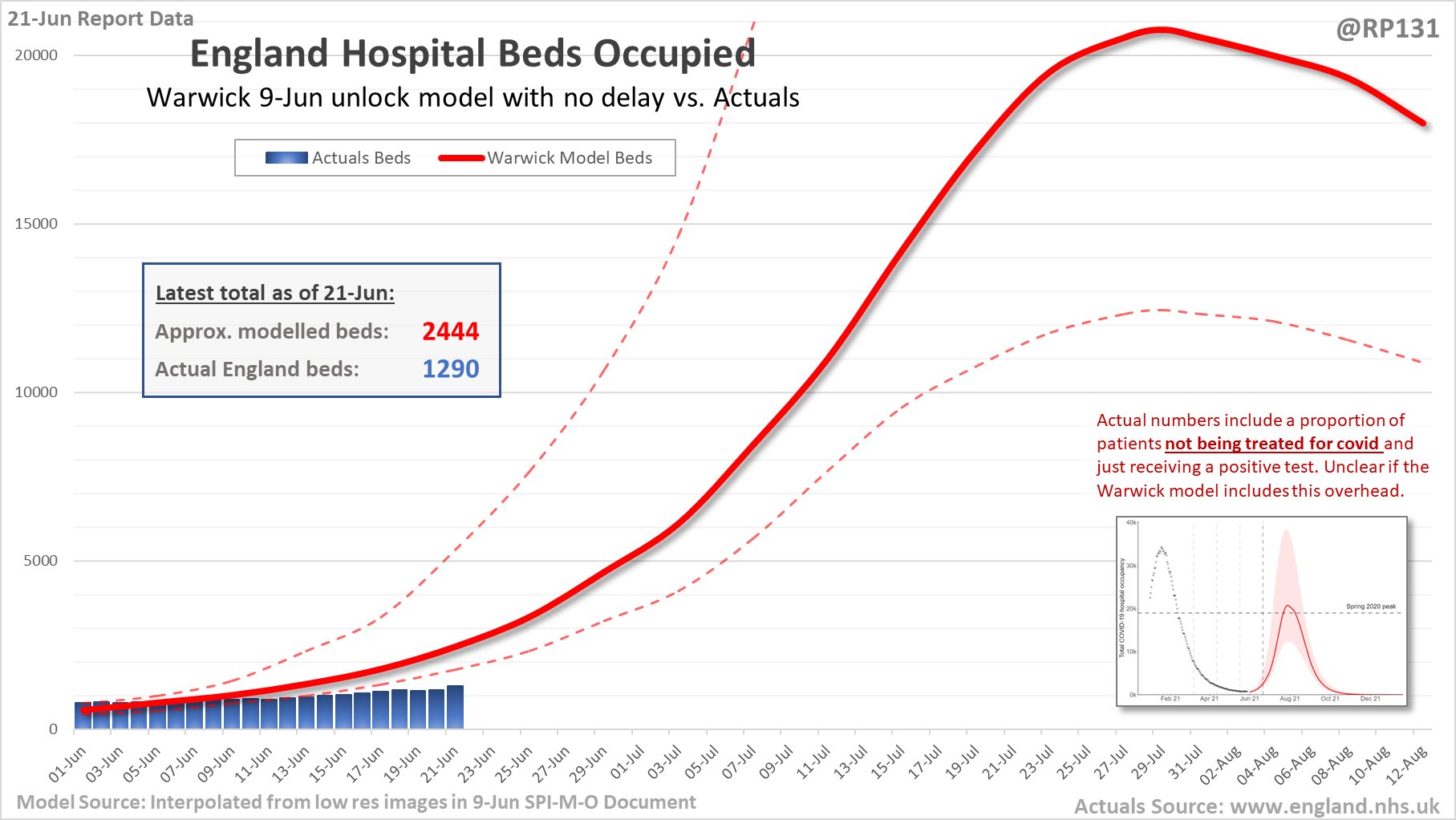
The models the Government is relying on to justify continuing lockdown have not got off to a good start. The projections of the huge summer wave should “freedom day” not be delayed are, as of June 21st (so before any delay could make a difference), almost twice as high for hospital occupancy as the actual number of Covid patients in hospital (see graph above).
Here’s a similar graph from the Spectator with the hospital admissions data superimposed on various SAGE projections (keep track of it here).
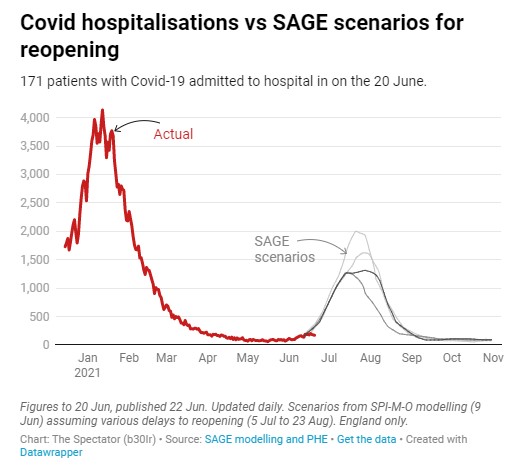
Fraser Nelson at the Spectator seems to share our scepticism at Lockdown Sceptics about Government modelling, reminding readers of the notorious SAGE autumn projections that envisaged up to 4,000 deaths a day by early December, but which were inaccurate the day they were published.
However, he then endorses scarcely less pessimistic modelling from Bristol University, which predicts that “hospitalisations peak at just over 900 on August 20th”.
While he admits that “no scenario points to the NHS being overwhelmed” since “Covid patients would occupy 2.5% of hospital beds” (at most), nonetheless he thinks the Government was right to delay the end of restrictions. This is because:
Under the current Dido Harding regime we’d see pubs shut because a waiter tested positive; entire classes of kids pinged and told to self-isolate, offices closed – and, as far as we can work out, on a scale larger than anything we seen so far. There would be anger, confusion – and no shortage of people willing to blame the June 21st unlocking. This would risk panic, damaging the confidence needed to rebuild the economy and society. It would have been a self-defeating liberalisation.
Without a hint of doubt, he asserts: “If we unlock this summer, a big third wave will get underway: it has started now and will become much bigger in days ahead.” In this he is following Professor Philip Thomas, leader of the Bristol modelling team, who wrote in the Spectator earlier in the month: “My model shows an enormous final wave, peaking during the middle of next month at anywhere between two million and four million active infections.” While vaccines are expected to keep hospitalisations and deaths down, this summer wave is still expected to eclipse the winter surge in terms of infections. Fraser explains:
The Bristol model reckons 85% of adults in England have detectable antibodies, with just two-thirds of whole population (i.e., including kids) immune. It assumes the Indian variant is infectious enough to work its way through everyone who remains susceptible, even if they end up with nothing more than a runny nose. The good news is that this will, at least, rule out a winter wave: by September there will be almost nobody left to infect.
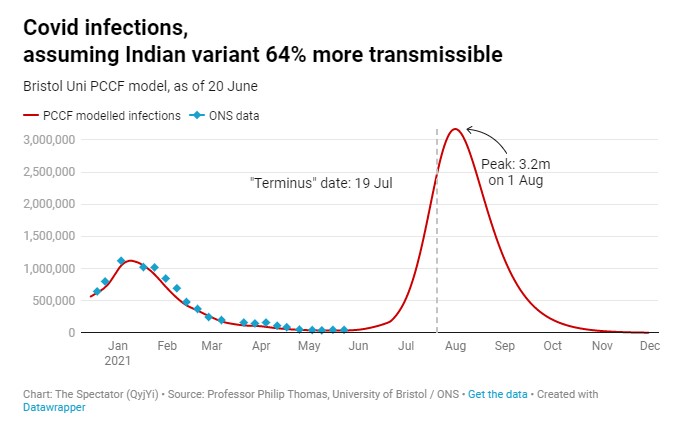
It works on the assumption that the Delta (Indian) variant is 64% more transmissible than the Alpha (British) variant, as per PHE’s claim in Technical Briefing 15.
However, as I noted when the briefing was published, the researchers admit that they did not control for household size. Since there is reason to think the small sample of Delta variant infections is biased towards ethnic groups with larger households, this makes the finding very unreliable (since larger households are more likely to have more secondary infections).
On the other hand, if we look at the secondary attack rate (SAR – the proportion of contacts that infected people infect) of the Delta and other variants as PHE has measured it over time we see that the claims of greater infectiousness fail to account for the fact that this quantity changes over time and tends to decline.
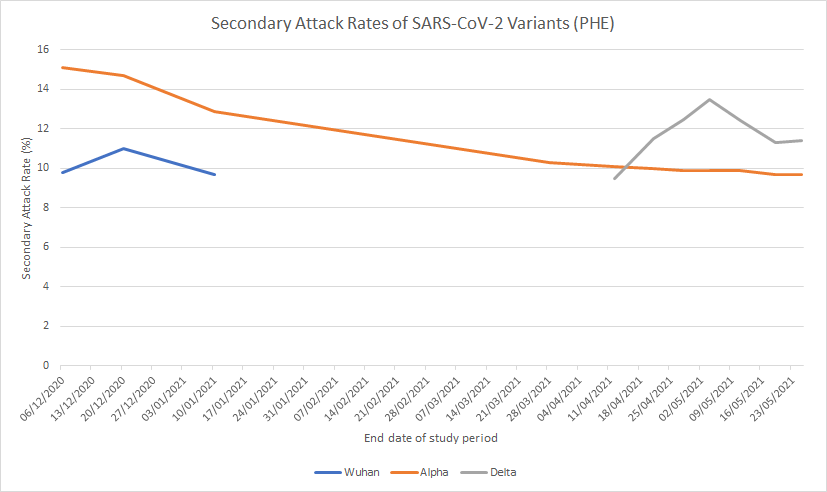
We also see that the Delta variant’s SAR is currently only a little above the Alpha variant’s: 11.4% of contacts infected versus 9.7%, a difference of just 1.7%. In addition, the Delta variant’s current SAR is no different to the Alpha variant’s at the start of March, undermining the idea that it is intrinsically more infectious.
Professor Thomas says he assumes “someone with the Indian variant will pass it on to 6.8 others in a fully susceptible population, a far higher multiple than the Kent variant (4.5 others)”. 6.8 is 51% more than 4.5. However, on the data above, the Delta variant SAR is only 18% higher than the Alpha variant SAR, and 24% lower than the Alpha variant SAR at the start of December. So there is no reason to assume the Delta variant is 51% (or 64% – it appears to have been revised up) more transmissible.
Further countering the idea of a hyper-transmissible Delta variant, Ivor Cummins has shown that the growth in dominance of the Delta variant has not coincided with a spike in infections (see graph below – the green line is positive cases superimposed on a graph of variant proportions, with the Delta variant in purple).
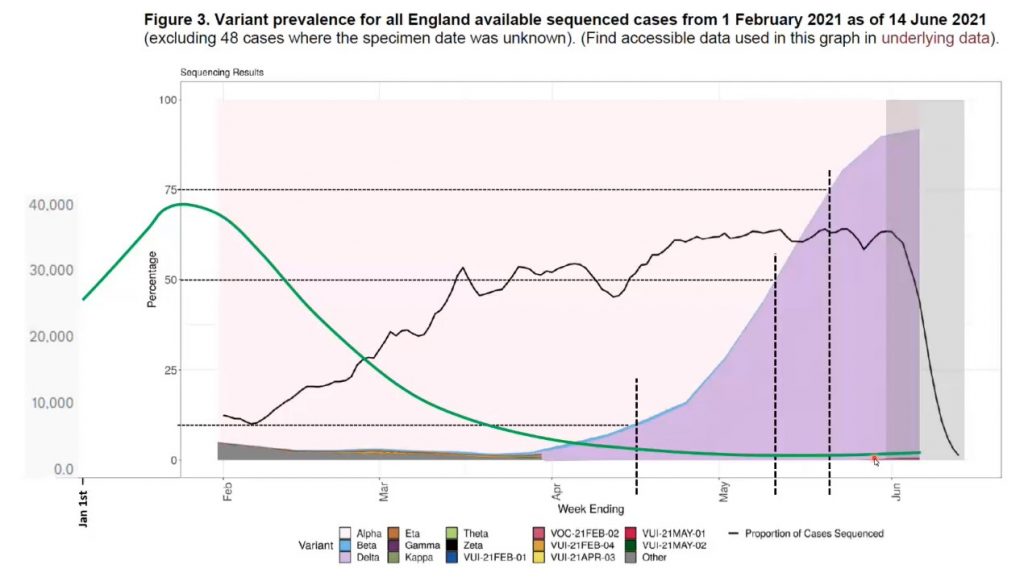
A further big problem with the Bristol model is that it assumes that anyone who does not have “detectable antibodies”, including children, is susceptible to the virus and will inevitably get infected during this summer wave – to the extent that it rules out a winter wave, since “by September there will be almost nobody left to infect”. This is reminiscent of the Imperial modelling from spring 2020 which assumed everyone was susceptible and predicted the majority of the population would quickly be infected.
All such models fail to allow for the fact that even without “detectable antibodies” (and that is an ill-defined concept anyway, as there are different kinds of antibodies and how detectable they are depends on the sensitivity of the test) many people have varying degrees of immunity to viruses like SARS-CoV-2. This is why even at the height of the winter surge, 85% of contacts of those with the new variant in town (then the Kent variant) did not contract the virus. Similarly, according to current data, 85% of those who live with people infected with the Delta variant do not become infected. Why then assume that everyone who does not have “detectable antibodies” will become infected in the next few weeks?
This is not to say that these people are entirely immune and will never be infected by any variant at any time. Viral transmission patterns remain somewhat mysterious, being affected by seasonality (itself likely influenced by temperature and humidity) and by various factors that make people more infectious or more susceptible at a given time. But we have enough data now to know that viral waves and surges will come and go without infecting everyone who is exposed, even if they lack “detectable antibodies”, and even if they may later become infected.
Professor Thomas – and Fraser Nelson – have now nailed their colours firmly to the mast. Professor Thomas is clear that he expects this big final wave regardless of the delay to reopening, as “the model shows that the virus is growing exponentially already; the final step on the roadmap out of lockdown makes little difference”. Within the next few weeks we will see whether he is right that everyone without detectable antibodies (including children) becomes infected. His graph of infections shown above indicates that he expects infections to enter a sustained spike lasting over a month any day now, climbing to over three million people infected by the end of July, so it won’t be long before we know whether his projections are in any way on the money.
If, as I suspect, nothing anywhere like this will come about, will Professor Thomas and Fraser abandon their faith in this simplistic form of modelling that has shipwrecked our country and come round to the more nuanced way of thinking of Professor Sunetra Gupta and others?
We’ll revisit this in a few weeks’ time to see if Professor Thomas and Fraser were right, or whether we need to put these questions to them again.











To join in with the discussion please make a donation to The Daily Sceptic.
Profanity and abuse will be removed and may lead to a permanent ban.