Millions of patients were urged Wednesday not to go to A&E unless they are dying after six trusts warned of waits of up to 12 hours in emergency departments. MailOnline has more.
Trusts across Yorkshire claimed the pressures have left them with no choice but to prioritise patients in “genuine, life-threatening situations”.
West Yorkshire Association of Acute Trusts, which covers 2.5million people, said its casualty units were “extremely busy”. Figures show there has been a “sharp uplift” in patients attending over A&E over the past fortnight, with the total number of visits up 14% on the same time last year.
Meanwhile, in another sign of the constant pressure NHS medics are facing, South Central Ambulance Service – one of the largest trusts of its kind in the U.K. – declared a critical incident this morning, telling patients to make their own way to hospital unless their injuries or illnesses are not serious.
The service, which covers seven million residents across Berkshire, Buckinghamshire, Hampshire, Oxfordshire, Sussex and Surrey, asked the community to only call 999 in an emergency.
Their warnings came as millions of Britons started paying more national insurance from today, with Boris Johnson insisting the 1.25% hike is ‘necessary’ to bail out the NHS and social care in the wake of the pandemic. The Prime Minister insisted it was the “right thing for the NHS”, which has seen waiting lists spiral to a record high after hospitals were forced to cancel thousands of operations during the pandemic.
Ministers insist the tax rise, tagged the Health and Social Care Levy, is needed to help tackle Covid backlogs and reform the adult social care system – raising £39 billion over the next three years.
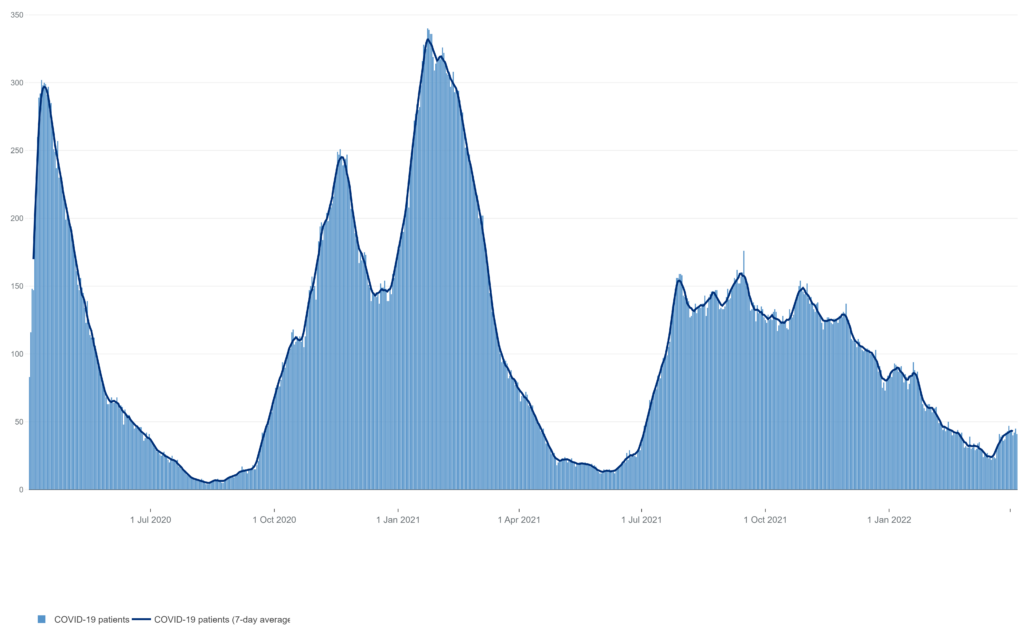
But health chiefs warned the service is already behind schedule in its routine care recovery plan because of rising numbers of Covid patients. More than 16,500 hospital beds are currently occupied by infected people in England, similar to levels seen during the worst part of the Omicron wave in January.
Chris Hopson, head of NHS Providers, said the rising rates – which appear to have finally slowed down – coupled with staff absences “mean that we’re not going as fast as we would like on backlog recovery”.
With over half of ‘Covid’ admissions currently being incidental admissions, i.e., patients being treated primarily for other conditions, the question is why these hospitals can’t cope with slightly higher numbers of patients than normal. The number of Covid patients in mechanical ventilation beds is way down on the second half of 2021. So it doesn’t appear to be COVID-19 that is causing the problems.
So what’s going on? Are too many staff staying at home with a runny nose?
Worth reading in full.














Profanity and abuse will be removed and may lead to a permanent ban.