There follows a guest post from HART member and Lockdown Sceptics veteran Dr Clare Craig responding to the alarming reports today that, as the Express headline put it, “Kent Covid strain could be twice as deadly”.
Yesterday the BMJ published a new article comparing mortality rates in people with old variant Covid and new variant Covid from October through to the end of January. Their headline conclusion was that the risk of dying was 64% higher in people who had caught the new variant (and perhaps up to 104%, hence the headline that it “could be twice as deadly”).
Before worrying that this may be the case it is worth looking closer at their results. There are a number of odd things about this study:
- Each person with old Covid was matched for sex, age, ethnicity, deprivation, location and date of infection. There were over 214,000 pairs found. However, it turned out that there was extensive duplication in the data and many of these “cases” were the same people. After removing duplicates there were only 54,906 pairs left.
- The two groups were not matched for comorbidities, meaning the study did not control for them. This was unfortunate as many comorbidities increase the mortality rate significantly.
- Their main finding was that 227 people in the new variant group died compared with 141 in the old variant group. This equates to a 99.59% survival rate compared to a 99.74% survival rate. While the difference may – according to the authors’ methodology – have been statistically significant, this does not equate to it being of any practical relevance in terms of the threat of this virus to society.
- Only people testing positive in the community were included which may account for the high survival rates as care homes and hospitals were excluded. However, the CFR was as expected from studies that did include hospitals and care homes in the over-70s but much lower than other studies in the under-70s.
- Mortality rates in Covid are markedly age dependent so it is important to interpret these results in the context of the age of the people in the study. To get a picture, suppose 50,000 members of the public had been randomly selected as a control with no Covid at all. According to the data in this study, this group would have seen the same mortality as old Covid in the first 10 weeks of the year (just as the normal mortality risk of being alive) and the same mortality as new variant Covid within the first 17 weeks of the year. After spring, David Spiegelhalter published on the risk of death from Covid pointing out that the infection fatality rate for someone who caught Covid was the same as their risk of dying this year without Covid. The fact that the mortality risk in this study is only 20-33% of a year’s worth of mortality suggests that Covid, in this study, is less deadly. Case fatality rates (CFR) always overestimate mortality compared with infection fatality rates (IFR) as the latter are based on immune responses and include all the mild cases that may not have been diagnosed as a case. The fact that this was based on case fatalities not total infection fatalities, like the David Spiegelhalter data, suggests it is even less deadly again.
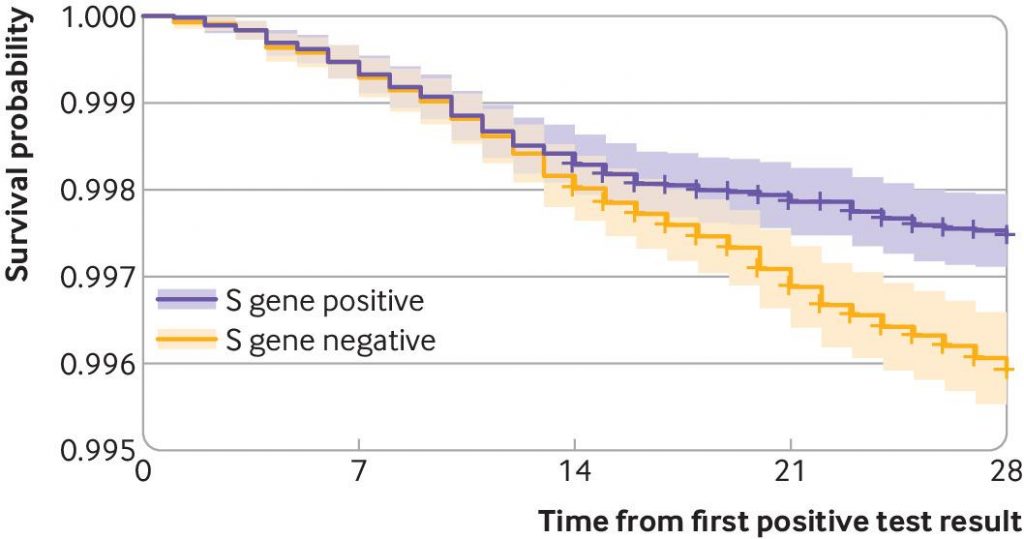
- The distribution of the deaths over time was also odd (see graph above). People with old variant Covid died mostly in the first two weeks and deaths after this time were fewer, reaching a plateau after the risk of the infection had passed. In contrast, deaths from the new variant continued linearly throughout the month of follow up. This is a very odd pattern for an infectious disease. The expected pattern would be that a more deadly variant would have a steeper gradient from the outset with both survival plots plateauing as the risk from the acute infection passed. Where the risk of death is the same the first day after infection as a month later it suggests there are other factors at play. Could a group with more comorbidities see a similar effect of the disease initially but a continuation of deaths from subsequent organ failure?
It should be noted that the difference in CFR reported in this study between new variant and other old variant is of a similar magnitude to that observed between regions for overall Covid CFR. Ultimately, a difference of only 0.15% between two groups where there has been no controlling for comorbidities should be ignored.












Profanity and abuse will be removed and may lead to a permanent ban.