How do you get people to take pharmacological action against something that hits them on average once a year and lasts a few days, like acute respiratory infections? They have been around since creation and are extremely familiar to everyone around the globe, including animals.
Acute respiratory infections manifest themselves with a range of symptoms – from none all the way to pneumonia and death from respiratory failure. Thankfully this happens only in a small minority of cases.
To sell, you have to have a market, but familiarity breeds contempt. So you have to create a market for your products, be they medicines, opinions, careers, research funds or whatever.
One approach is to confuse a syndrome with a disease. This means using the F-Word ‘flu’, a terrible Anglo-Saxon colloquialism which is used all over the world, even by WHO and the U.S. CDC. Using the F-word, you are bundling up familiar signs and symptoms, fever, ache and pains, tiredness, cough and runny nose due to numerous but uncountable microorganisms (a syndrome) and implying that it is due to a single agent (influenza).
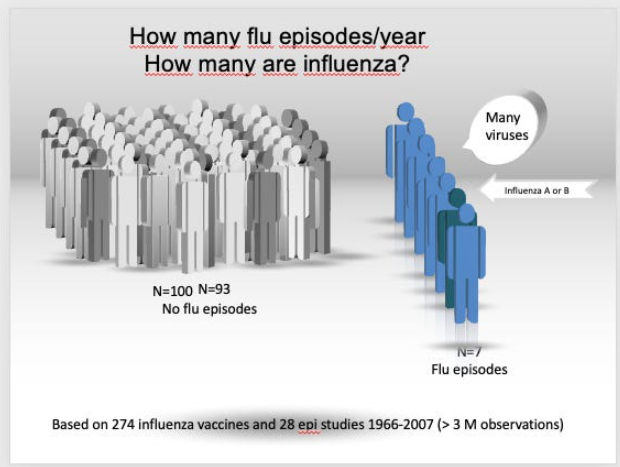
In a pie study, we did nearly 20 years ago, we showed that based on three million observations in an average year, only one out of nine F-word episodes are due to influenza.
When ministers blame winter crises on ‘flu’, we do not really know what they are talking about (neither do they), but they do have a solution: vaccines and antivirals. That is because, up until very recently, influenza was the only seasonal respiratory agent for which licensed pharmaceuticals (antivirals) or biologics (vaccines) were available. Now the tune has changed, they blame it on ‘Flu and Covid‘ (F- and C- words), but it’s just an update of the same manipulation.
Politically this is a helpful strategy. Because instead of admitting there is little that can be done to minimise the impact of the seasonal F-word and the ‘new’ C-word, you can be seen to be doing something like railing about low vaccine uptakes or putting pressure on pharma to produce more antivirals.
A second approach is to frighten everyone into thinking that the yearly death tally for the F-word (influenza) is a lot higher than what is verifiable and that the next pandemic is around the corner.
You do need the media’s help to frighten everyone, but you can always find editors to oblige.

Some media may be owned at least in part by pharma, which makes life a lot easier to get your message across.
We have seen this approach in detail with Covid and the yearly F-word ‘flu’ for at least fifty years. How do you inflate deaths? That’s easy! You start with taking the bundle ‘influenza and pneumonia’ on a death certificate as a true, verified fact. We have explained just how imprecise this method is. For example, in the U.K., in 2015, there were three verifiable influenza deaths per million inhabitants, rising to roughly 24 per million in 2018. Is this a health crisis? Hardly enough to justify doing much. This is why incidentally, influenza vaccines and antiviral trials show an absence of evidence on death prevention: the outcome is too rare even for a large trial.
The next step is to ask modellers to forecast deaths either in what you will call interpandemic or in intrapandemic years.
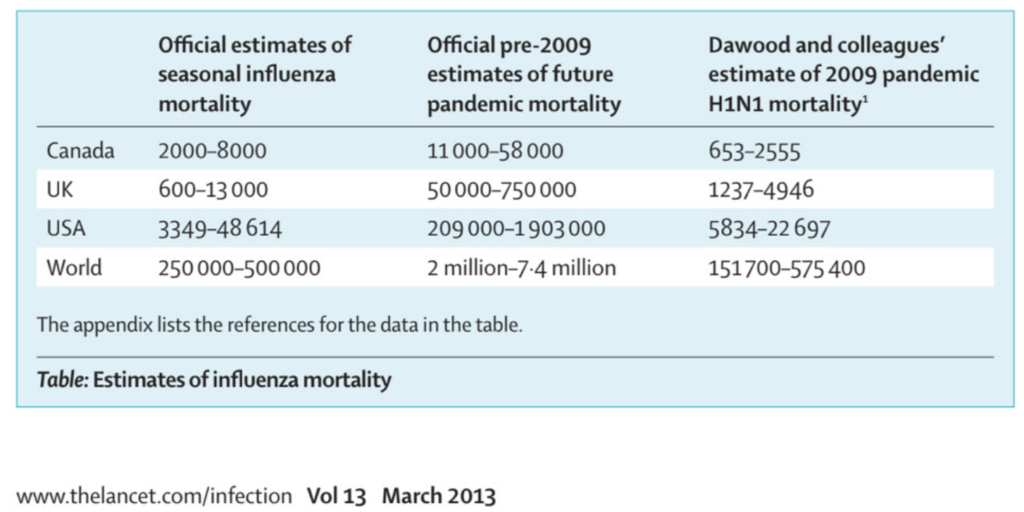
In going back to models, note the use of the two terms (interpandemic and intrapandemic), which subtly introduced the concept of the inevitability of a pandemic. “It’s just a question of time.”
A third approach is to appoint those who most benefit from creating fear to run or inform your Government of ‘protection measures’, as pointed out by Philip Alcabes at the dawn of the 2009 influenza pandemic:
We are supposed to be prepared for a pandemic of some kind of influenza because the flu watchers, the people who make a living out of studying the virus and who need to attract continued grant funding to keep studying it, must persuade the funding agencies of the urgency of fighting a coming plague.
This is why the worst-case scenario is always presented.
A further approach is to create a cartel of key opinion leaders apparently hugely knowledgeable and capable of giving advice even on newly identified agents. This is the case for the European Working Group on Influenza (or ESWI), which is funded by pharma companies and has been hugely successful in influencing opinion and even policymaking. Many of the ESWI member names recur in our series on antivirals.
Keith Duddlestone pointed us to a further refinement: adding ‘community groups’ to the chorus of voices building pressure. Patient involvement is an old marketing technique, but continuous funding by the industry points to their importance in creating demand.
Then you should present your product as the pharmacological equivalent to a Gucci bag or Rolex watch, a designer drug tailored and produced to keep the monster at bay. Yes, such articles exist, written by people who should have known better because they have a long history of doing good work in this area.
Linked to this is the other approach to turn funders and industrialists into saviours. This happens time and time again when politicians are running out of fig leaves – we will publish three of the contracts that states stipulated with vaccine manufacturers in the run-up to the 2009 influenza pandemic.
We would be very surprised if the model had changed during the last pandemic.
Last but not least, you can change definitions such as ‘pandemic’ to fit what is going on rather than the other way around. This way, the facts always fit the definition, and you can keep everyone on their toes and provide the magic button to be pressed to activate sleeping contracts and emergency laws: it’s a pandemic! Panic stations.
Here is a rather blatant example: the 2009 influenza pandemic was nowhere as severe as the marketeers forecast, so they needed to change a few things, better if done without creating too much fuss.
Manipulation apart, the WHO ‘pandemic preparedness’ page shows a further and now discredited equation: that ‘pandemic’ means influenza. In the end, the most perceptive observer of the many transformations, Peter Doshi, concluded that there is no universal definition of an (influenza) pandemic.
So are we sleepwalking into something much worse than the last three years if the WHO is true to form?
But make no mistake: the creation of the market for antivirals has been hugely successful, as a reply to a Parliamentary question shows:
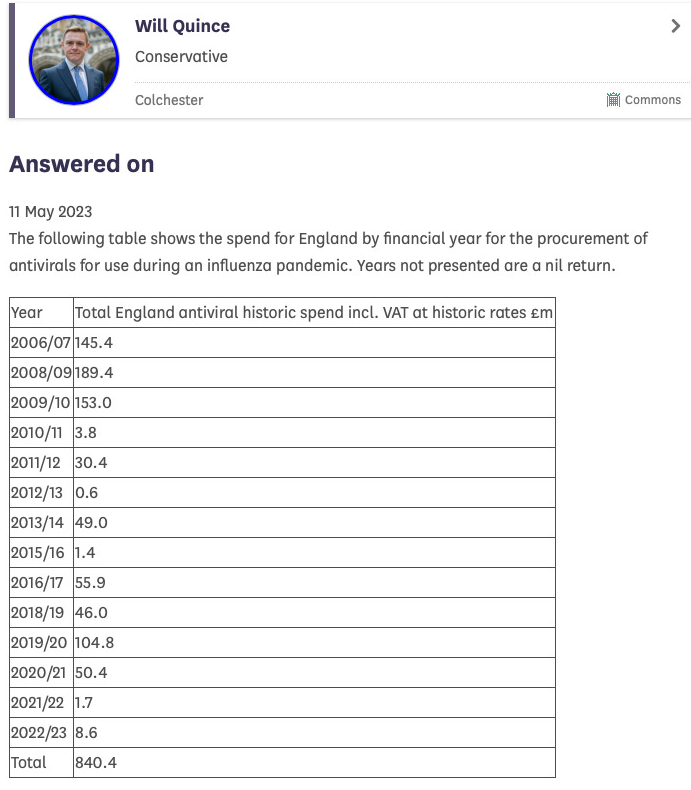
Pandemics are good for the business model of antivirals: £840 million spent so far. Not a bad return for ‘modestly’ performing drugs!
Dr. Carl Heneghan is the Oxford Professor of Evidence Based Medicine and Dr. Tom Jefferson is an epidemiologist based in Rome who works with Professor Heneghan on the Cochrane Collaboration. This article was first published on their Substack blog, Trust The Evidence, which you can subscribe to here.














To join in with the discussion please make a donation to The Daily Sceptic.
Profanity and abuse will be removed and may lead to a permanent ban.