In a recent viral tweet, Vincent Rajkumar – a professor at the Mayo Clinic – said the following:
South Korea followed the textbook principles of epidemiology. Kept deaths 40 times lower all the way till 75% of population fully vaccinated. This is success.
His tweet was accompanied by a chart showing the cumulative Covid death rate in the U.S., U.K. and Korea, with the line for Korea being much lower than the other two. In a follow-up tweet, Rajkumar identified the measures that supposedly account for Korea’s success, basically masks and contact tracing.
The implication is that if only the U.S. and U.K. had “followed the textbook principles of epidemiology” like Korea, they too could have achieved very low Covid death rates. But I’m not convinced.
First, there’s one small technical detail, which is that the U.K. did try both masks and contact tracing, and neither had much impact on the epidemic’s trajectory.
A recent report by the Public Accounts Committee concluded that Test and Trace (the U.K.’s contact tracing scheme) had “not achieved its main objective”, despite an “eye watering” budget. £37 billion here, £37 billion there, and pretty soon you’re talking about real money…
So far so bad for idea that all we needed was masks and contact tracing. But there’s another reason to doubt the implication of Rajkumar’s tweet: Japan achieved exactly the same outcomes as Korea, and it did almost nothing until the start of this year.
In 2020, Japan had zero days of mandatory business closures and zero days of mandatory stay-at-home orders. The country relied on “limited contact tracing” (a designation given in the Oxford Blavatnik School’s COVID-19 Government Response Tracker). This is in contrast to Korea, which used “comprehensive contact tracing”.
The chart below plots the stringency index for Japan, Korea and the U.K. Apart from a brief period at the start of 2020: the U.K.’s index has consistently been highest, while Japan’s has consistently been lowest.
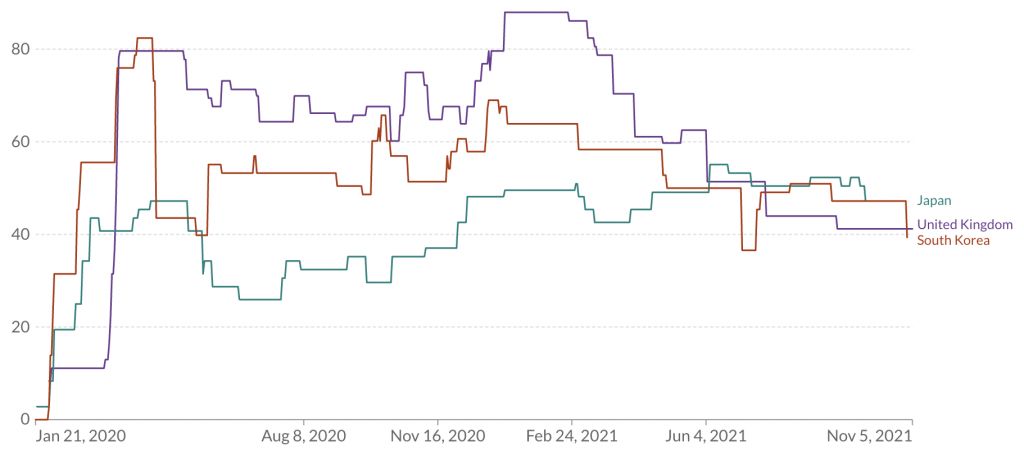
In spite of this, both Japan and Korea have had zero excess mortality to date, whereas the U.K. – the most stringent of the three countries – has had between 6 and 20% excess mortality, depending on how you compute it.
The experience of Japan, combined with the global pattern of excess mortality, suggests that some cultural or biological factor that’s unique to East Asia explains the low death rates – and indeed the low infection rates – in that region. This factor could be more diligent social distancing or perhaps greater prior immunity.
Whatever the explanation, it’s unlikely Korea’s success could have been replicated in Britain – even if we’d ploughed the entire NHS budget into Test and Trace.












To join in with the discussion please make a donation to The Daily Sceptic.
Profanity and abuse will be removed and may lead to a permanent ban.