It’s not two weeks since Lockdown Sceptics was casting doubt on Public Health England’s alarming claim that the Delta (Indian) variant had more than double the risk of hospitalisation of the Alpha (British) variant. How long will they take to backtrack after the panic has done its damage, we asked?
Well, it turns out that even before Boris took to the podium on Monday PHE had already released a new study claiming that vaccines after all are more effective at preventing hospitalisation against the Delta variant than the Alpha variant. Here’s the story in the Telegraph:
Vaccines are more effective at preventing hospitalisation against the Indian/delta variant than they were against previous types, once people are double-jabbed, new data shows.
Real world data shows the Pfizer/BioNTech vaccine is 94% effective against hospital admission from the variant after one dose, rising to 96% after two jabs.
The Oxford/AstraZeneca vaccine was found to be 71% effective against hospital admission after one dose, rising to 92% after two jabs.
In both cases, two doses had a greater impact preventing hospitalisations than was the case with the Kent variant.
The new study and the earlier study aren’t quite showing the same thing. The earlier study showed the risk of hospitalisation with the Delta versus Alpha variant for all those testing positive, not just the vaccinated, though subsequently adjusted the results for “vaccination status”. The new study specifically looks at the hospitalisation risk in those vaccinated with respect to the Alpha and Delta variants and compares them. However, the two studies should come to broadly the same conclusion, as they are both looking at how much more serious disease is with the Delta variant. At any rate, given that a large proportion of the vulnerable population is now fully vaccinated, we certainly shouldn’t see a doubling in the hospitalisation rate with the Delta variant if, as is claimed in the new study, the vaccines are better at preventing serious disease from that variant.
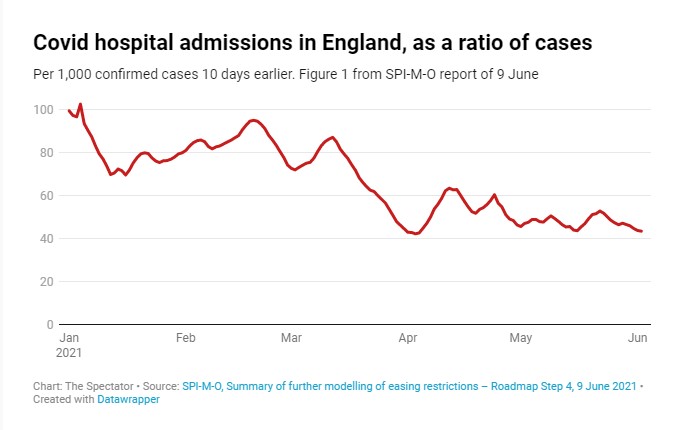
Ross Clark suggests the problem with the earlier data was that the sample size was small and biased. As he notes, PHE’s modelling misses the most obvious data point, that the rate of hospitalisations per case has not increased as the Indian variant has become dominant (see graph below). How then can the Indian variant have twice the risk of hospitalisation?
Is the new study any more reliable than the earlier one? As usual with a PHE observational study, it’s hard to tell, as much of the method is hidden behind opaque statistical techniques with working that is not set out. All the reader knows is that raw data is taken and transformed by some statistical process into hazard ratios and vaccine effectiveness estimates that are all but impossibly to verify. What we can do, though, is look at the results of this largely concealed data-processing and see if it makes sense.
Below is the table from the study (there’s only one, it’s a very short paper), and it shows something very curious.
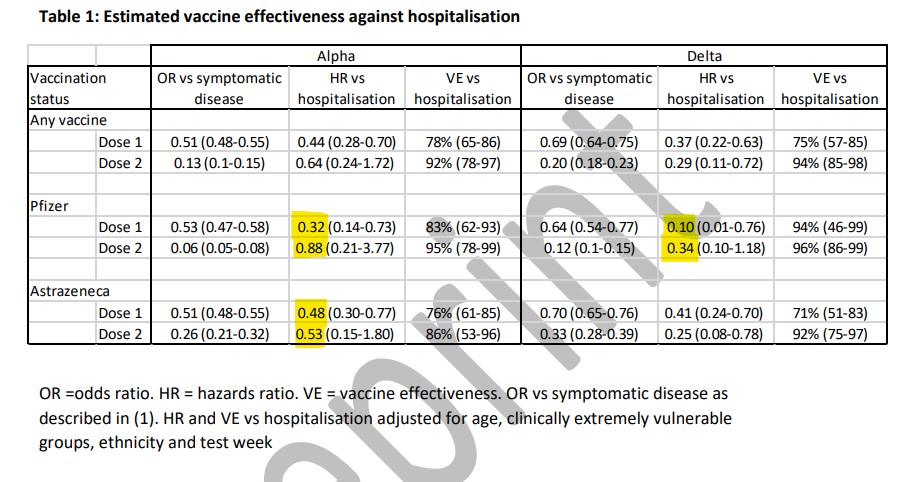
It shows that, once testing positive with the Alpha variant, one dose of Pfizer reduces the risk of hospitalisation by 68% (the 0.32 highlighted), but the second dose only reduces the risk by 12%! That’s 12% in total (the 0.88 highlighted), not 12% on top of the 68%. So the second dose significantly increases your risk of being hospitalised compared to the first dose? That can’t be right. But it’s what it says.
The same thing happens with AstraZeneca against the Alpha variant: the first dose reduces the hospitalisation risk by 52% (the 0.48 highlighted) but the second dose only by 47% (the 0.53). And again with Pfizer against the Delta variant: the first dose reduces hospitalisation risk by 90% (the 0.10), the second dose only by 66% (the 0.34). The only combination where the risk-reductions are the right way round is AstraZeneca against the Delta variant: one dose reduces the risk by 59% (the 0.41 not highlighted under the 0.34) but two doses reduces it by 75% (the 0.25 beneath).
The gaping confidence intervals (0.21-3.77; 0.15-1.80; 0.10-1.18; 0.08-0.78) are also giveaways of a lack of reliability in the findings. For instance, the Pfizer dose-2-against-Alpha confidence interval of 0.21-3.77 means the authors are 95% sure the hospitalisation risk lies somewhere between a reduction of 79% and an increase of 277%! That’s basically meaningless.
How did the authors avoid these blatant red flags in their data and modelling (the hazard ratios are a modelled value) showing up in the headline figures? By keeping the report very short, not discussing the limitations of the study, and only converting to a percentage value (which is readily understood by many people) the overall vaccine effectiveness against hospitalisation (i.e., the risk of hospitalisation-once-infected multiplied by the risk of being infected), while leaving the dubious hospitalisation hazard ratios as an obscure decimal. It seems to have worked: journalists have dutifully reported the headline vaccine effectiveness figures but not queried the strange hazard ratios behind them.
A separate study from Scotland, published as a research letter in the Lancet and reported alongside the PHE study in many places, claims to find the vaccines are a bit less effective against the Delta variant. But it too is heavily adjusted, its positivity figures are all over the place (e.g. the Delta-variant test-positivity for AstraZeneca 13 days after the second dose is nine times as high as for Pfizer) and the confidence intervals again are huge, suggesting a small sample with low confidence.
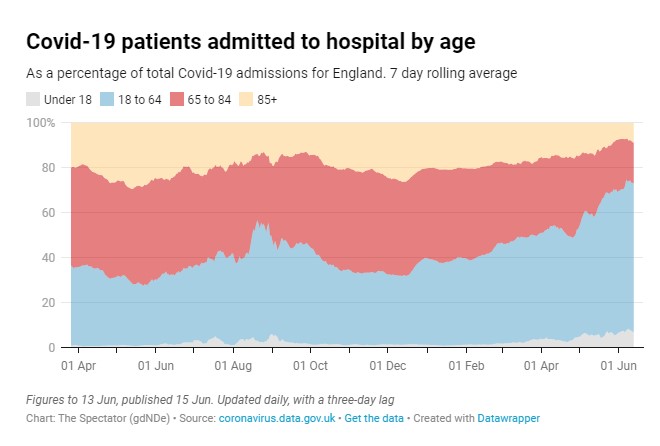
Despite these problems with both studies, I do think the vaccines probably are effective against serious disease to some degree. (Safety is a separate matter.) The reduction in the proportion of Covid hospital admissions in the over 65s in the past few months (see graph below) is perhaps the most striking data point on this. This fits with the detection of antibodies in the blood post-vaccination – if the disease progresses to a systemic stage then the body has additional antibodies to fight it.
I’m less convinced at the moment on how effective the vaccines are against infection and transmission. Almost all the studies on this are confounded by declining background incidence (among other problems). Also, we know the vaccines do not produce mucosal (IgA) antibodies, which have been shown to dominate the early response to SARS-CoV-2. This suggests the defence they offer against infection and mild disease may be less robust. Places with high vaccination rates and high case rates such as Seychelles, Maldives, Bahrain and Chile also suggest the protection against infection may be limited. But perhaps more data and new studies will alter that picture – I’m certainly on the lookout. They’ll have to do better than PHE, though.












To join in with the discussion please make a donation to The Daily Sceptic.
Profanity and abuse will be removed and may lead to a permanent ban.