As new mortality data come in, it’s increasingly clear that something abnormal happened in the spring of 2021 when it comes to people dying of causes other than flu, Covid and other respiratory diseases.
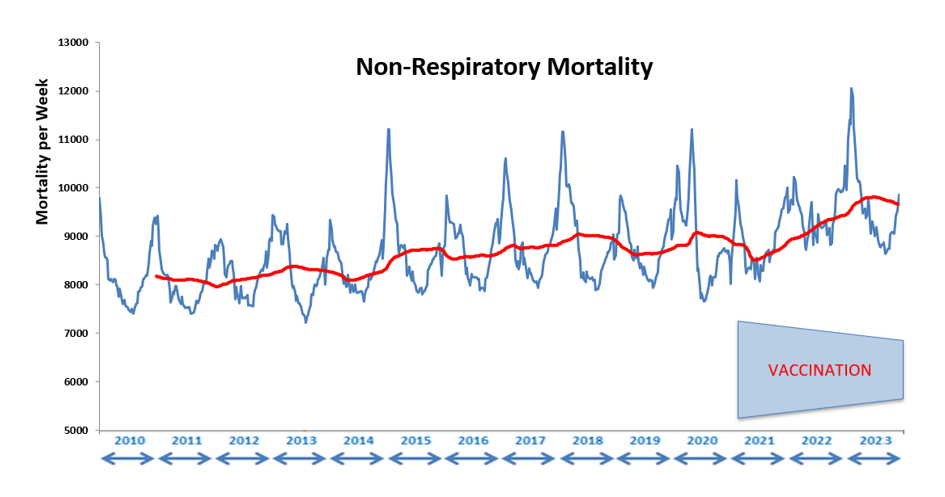
I have updated the non-respiratory data to the end of 2023, so there are now four years of Covid-era data included in it. The progression can however be traced back all the way to 2010, as shown below (the red line is the running 52-week average), and the sharp rise from early 2021 is now clear as day. Whatever is behind this has caused a rising trend in non-respiratory mortality (NRM) that has now stabilised, but at a much higher level than before the whole Covid imbroglio began. In fact, 2023 showed the worst total non-respiratory mortality figures than in any of the three preceding years, at 9.5% above the pre-Covid 2015-2019 average. In recognition of this sorry reality, the ONS this week said that life expectancy has gone backwards by 12 years to 2010 levels.
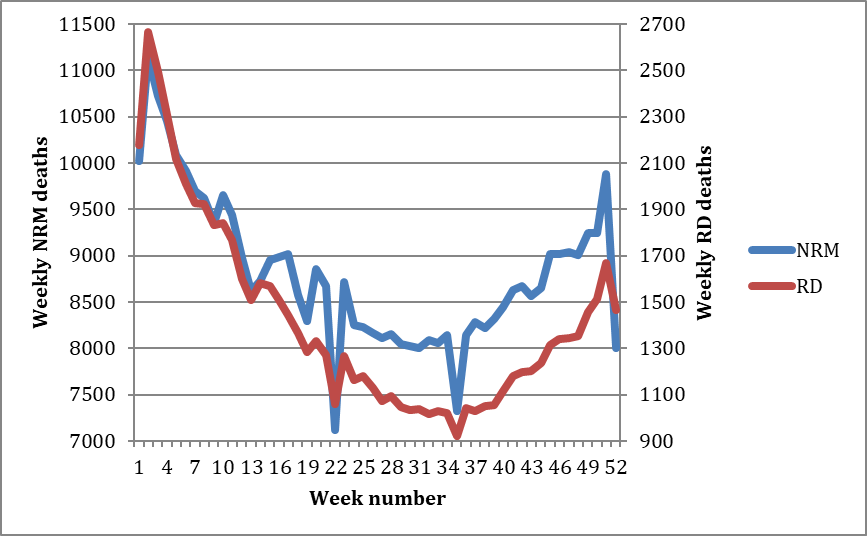
Take a look at the chart below, which shows the NRM pattern during the period 2015-2019 as well as the corollary for respiratory disease mortality (RD). Averages for each week are shown. The deaths from respiratory illness are by definition from acute disease, at least those that were properly registered as ‘died from’ rather than ‘died with’. The two lines match very closely in shape at least, the only real difference being the total numbers involved in each case (note the different range for respiratory disease on the secondary Y axis on the right hand side).
To emphasise this similarity further we can compare the ratio of non-respiratory mortality to respiratory disease mortality for each year from 2010 to 2019. They run like this:
- 2010 6.33
- 2011 6.16
- 2012 6.08
- 2013 5.82
- 2014 6.58
- 2015 5.98
- 2016 6.28
- 2017 6.26
- 2018 6.07
- 2019 6.36
Average for the whole period is 6.18.
The maximum variation in each year from the average proportion of NRM deaths to total deaths (average of 86.1%) is only 0.75% (up or down). This all goes to show that there is a strong consistency to the overall yearly figures, despite the large variation in weekly death numbers for both non-respiratory mortality and respiratory mortality over the course of each year.
NRM is clearly highly seasonal, so even though the bulk of these deaths arise from chronic morbidity, whatever it is that tips an individual over the edge to his or her demise varies over the course of the year.
My working assumption is that whatever factors drive normal seasonal variation in acute respiratory disease mortality are also responsible for a similar variation in the proportion of people dying from chronic disease during any given week of the year. The importance of studying seasonal variation as the main driver of disease variability was emphasised in a recent paper in the peer-reviewed Journal of Clinical Medicine, which strikingly found no noticeable effect on Covid incidence patterns from vaccines and non-pharmaceutical interventions but a clear link with the seasonality of coronaviruses.
The most likely common factor to search for is whatever causes a variation in the vulnerability of people to any form of external shock, e.g. a reduction in their immune defences. In the normal course of events this may for example be something climate related (e.g. cold weather) or perhaps depends on some other natural variables like sunlight intensity.
Could a man-made event that may have had a large influence on the immune status of large sectors of the population have changed the overall picture in a very different way? It may be a worthwhile exercise to look for such a signal in the mortality figures.
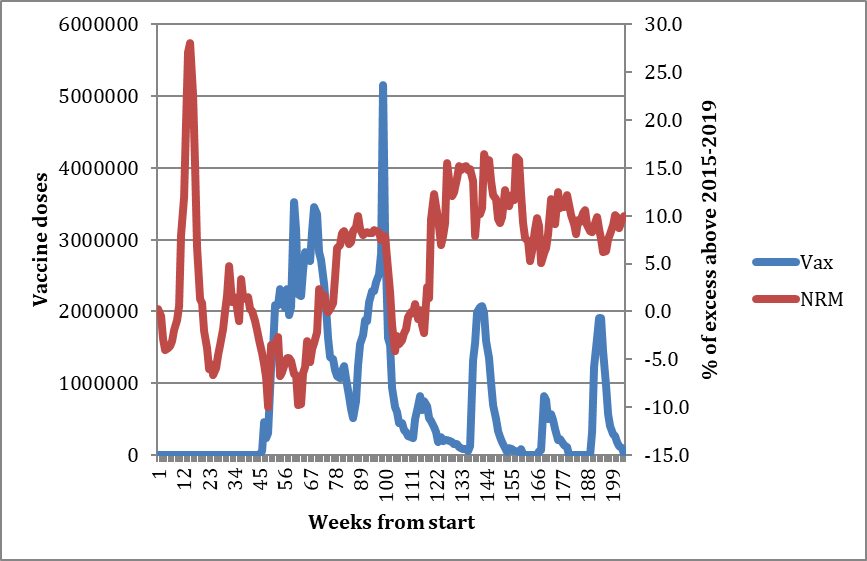
Turning to the Covid years, the chart below shows the excess mortality for both NRM and RD for the period 2020-2023, as well as the number of vaccine doses administered. Here we can see that the usual mortality patterns are at first completely disrupted, and this is consistent with the argument that a new pathogen which had never been encountered before had arrived and consequently had an outsize influence on acute mortality. However, by 2023 we can see that the ratio between NRM and RD has once again settled back to normal:
- 2020 3.27
- 2021 3.88
- 2022 5.86
- 2023 6.16
Average for the whole period is 4.49.
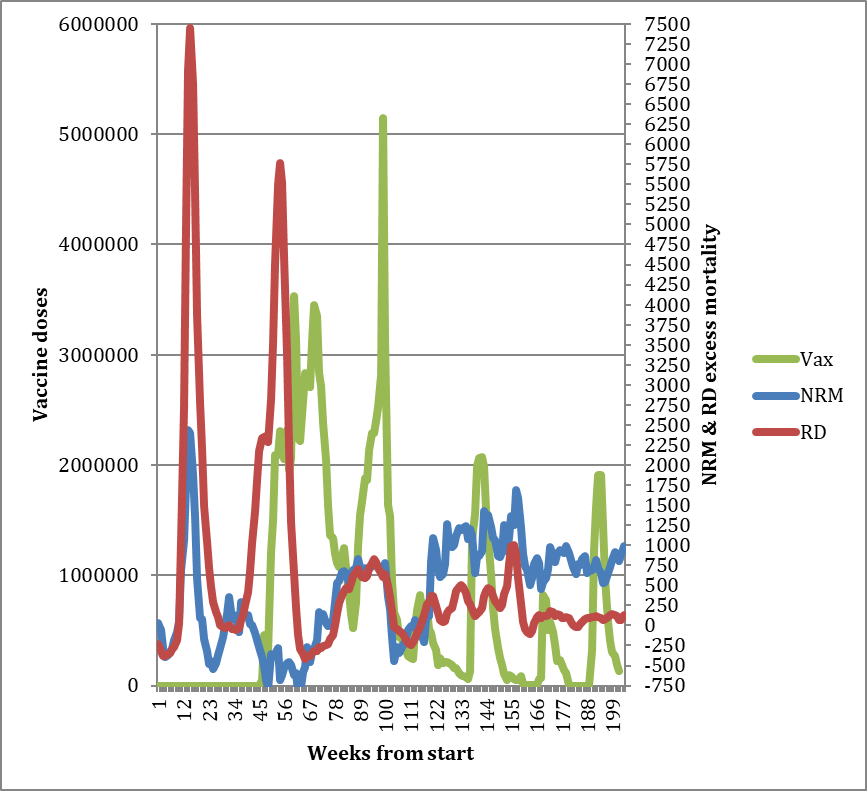
Already with this chart it is possible to see that, by comparing the different way the NRM and RD excess mortality responded to the initial Covid waves, the component of non-respiratory mortality derived from the after-effects of Covid itself (i.e., Long Covid) is probably relatively small. This is because NRM excess (blue line) was falling significantly – as expected due to mortality displacement – after the initial spike of deaths in the spring of 2020, even while the second RD spike (red line) was in full flood. This suggests that the after-effects of the first wave did not markedly increase non-respiratory mortality during the rest of the year.
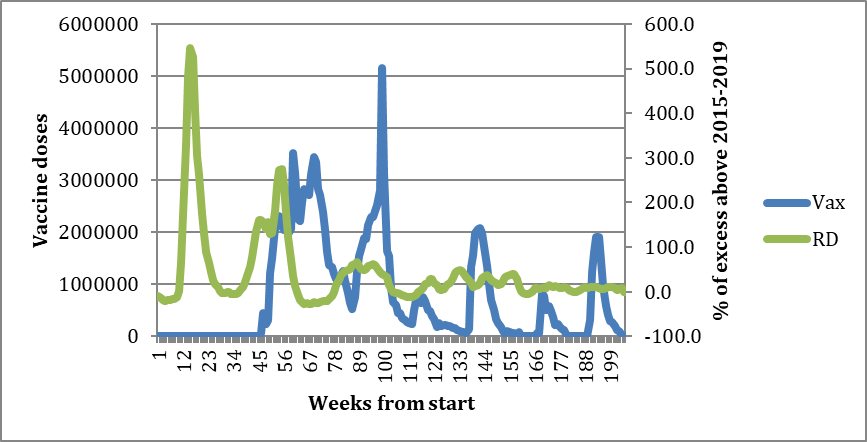
This is not the case with regard to the vaccination campaigns. To illustrate this one can look at the percentage changes from the 2015-2019 pre-Covid baseline for both non-respiratory and respiratory excess deaths (see charts below). NRM excess percentage (bottom chart, red line, right-hand axis) has been increasing year-on-year since the vaccine campaigns, whereas RD excess percentage (top chart, green line, right-hand axis) has been diminishing. The respiratory disease mortality has been falling despite the number of vaccine doses also falling each year. Note the different values on the secondary Y axis (right hand side) in each chart.
Vaccines delivered:
- 2020 75 million (doses one and two)
- 2021 40 million (dose three)
- 2022 25 million (doses four and five)
- 2023 17 million (doses six and seven)
Respiratory disease excess over 2015-2019 baseline (RD):
- 2020 91.3%
- 2021 62.6%
- 2022 13.9%
- 2023 9.9%
Non-respiratory mortality excess over 2015-2019 baseline (NRM):
- 2020 1.0%
- 2021 2.0%
- 2022 7.9%
- 2023 9.5%
The fall in respiratory mortality can perhaps best be explained by the attenuation expected from a gradual increase in population immunity to the new pathogen, and also by a declining virulence of the pathogen itself (e.g. the less deadly Omicron variant). But how does one explain the non-respiratory mortality changes, other than through a general long-term decline of the overall health of a population?
Unfortunately, it is still not possible to state with any certainty which component of the public health measures employed (vaccines or NPIs) can give the most plausible explanation for the bulk of the non-respiratory excess death phenomenon (assuming, as noted above, that the contribution from the virus by itself is relatively small). Many who have commented on these developments believe that the vaccination campaigns primarily caused the uptick. This can only be confirmed once the authorities release full mortality data including the vaccination status of all individuals at the time of their death.
The recent whistleblower data release in New Zealand provided in my view the strongest evidence to date of a temporal association between vaccination status and increased excess mortality. It is now all but impossible for the authorities to deny the link. If they want the public to feel safe about Covid vaccinations again, it is now up to them to disprove that vaccinations were causative in the excess mortality experienced over the last three years.
The key insight to be gleaned from separating overall mortality data into the two components of respiratory and non-respiratory disease is in recognising that both are subject to the same seasonal variability in population health vulnerabilities. They are coupled together such that as one rises, the other falls. This is presumably because they depend on the same pool of vulnerable people who are at risk of dying at any particular time.
Covid was a novel pathogen that in 2020 disproportionately increased respiratory mortality and thus, due to their synergy, pushed non-respiratory mortality downwards (part of the mortality displacement effect). Something then happened in 2021 that increased the size of the pool of vulnerable people over the following two years. The normal relationship between the two mortality types has re-established itself in 2023 (e.g. the proportion between them was restored), but at a level around 10% above pre-Covid mortality.
Total excess deaths for the four years (compared to 2015-2019) have now reached around 225,000, which should under normal circumstances lead to a fall of around 9% (i.e., 20,000) in annual deaths in subsequent years due to mortality displacement as deaths of the old and vulnerable are brought forward by some unusual event. Instead, what we see is excess mortality in 2023 reaching a new peak of 10.6% with currently no signs of slowing up. Once you take into account that instead of 9% fewer deaths we have 10.6% more, this adds up to a huge nearly 20% rise above expected levels. Welcome to the new normal.












To join in with the discussion please make a donation to The Daily Sceptic.
Profanity and abuse will be removed and may lead to a permanent ban.