I have been travelling the past few days, which is the reason for my silence. Now I’m returning home, dodging the mask police on an egregiously delayed train, and the intermittent mobile internet so characteristic of Germany is destroying my ability to research a longer post. Woe is me, I know.
Instead, I’ll address a matter raised by many of the comments to my last post, namely the reliability and significance of polymerase chain reaction diagnostic panels. I’ve wanted to address this for while, because every time I discuss any study that involves PCR in any way, many readers respond with a range of bitter objections.
I get it: Three years of pointless mass testing and the heavily propagandised presentation of disease statistics have made everyone wary of mass testing for viruses. That’s fine. But, propaganda is rarely based on total lies, because outright deception is expensive to maintain and requires a high level of coordination. You are deceived much more often by misdirection and deliberate silence. The (mis)use of PCR during the pandemic is no exception.
A lot of the puzzling decisions made by our public health authorities over the past few years are downstream of a fundamental choice, taken sometime between February and March 2020, to abandon traditional, mitigationist pandemic planning, in favour of Chinese-style mass containment. Public health is supposed to be about improving health outcomes across the whole population, but in 2020, public health bureaucrats decided it would be more fun to exterminate a virus, regardless of what this project meant for anybody’s health. Once you understand this basic shift in mission, a lot of other things fall into place, including the bizarre testing regime favoured by the pandemicists.
Critics of the PCR have three fundamental complaints. These are 1) that viruses aren’t real or are somehow a hoax; 2) that Kary Mullis and others have said the PCR is not appropriate for diagnosis; and 3) that the American CDC said the PCR cannot differentiate between influenza and SARS-2.
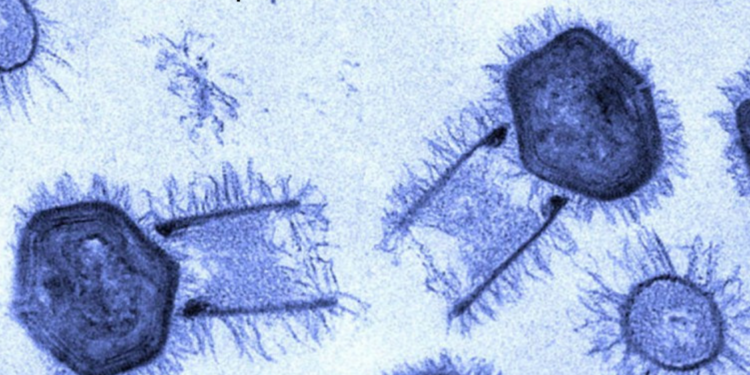
I’m not going to deal with (1) here, because in my experience, people who deny the existence of viruses won’t accept any arguments or evidence to the contrary, and these debates aren’t productive. Viruses, indeed, are real; the largest viruses can be seen with optical microscopes (depicted above); and if you know anything about cell metabolism, you can appreciate why they exist. There’s nothing remarkable or exceptional about viruses.
While (2) is a reasonable complaint for those interested in individual medical diagnoses, it doesn’t really address the population-wide significance of PCR-generated case statistics. A well-validated PCR diagnostic panel (and the tests in use are generally well-validated) doesn’t diagnose current symptomatic infection, but as I typed above, this isn’t really what our public health authorities are after. They don’t care whether anybody is actually sick. They’re locked in pitched battle with a virus, and they want to know how much virus is out there and who is potentially shedding virus, so they can lock them up. This explains the preference for high cycle thresholds, which detect primarily past infections or trace amounts of contamination. In these cases, the PCR really is detecting viral RNA, even if there’s no active infection, and that’s enough for the virus eradicators. When we’re discussing studies about the seasonality of various viruses, or the fate of influenza during the SARS-2 pandemic, it’s also enough for us, because in these cases we’re also not interested in counting sick people or diagnosing anybody. We’re trying to work out when viruses are present in their hosts, which is a different question.
As for (3) and the CDC: PCR tests have gene targets that are selected because they are (believed to be) unique to the SARS-2 virus. These are RNA sequences that, as far as we know, other viruses don’t have. These tests really, honestly won’t light up on other common respiratory viruses like influenza, because the people who develop these diagnostic panels target genetic sequences that do not occur in influenza viruses. There was no little skullduggery involved in Christian Drosten’s Eurosurveillance paper from January 2020 on the Detection of 2019 novel coronavirus (2019-nCoV) by real-time RT-PCR, but any intellectual malfeasance here has limited significance for the actual detection of SARS-2, because the gene targets Drosten’s team chose are found only in the original (extinct) SARS virus from 2003-4, and in SARS-2. Could there be as-yet unknown viruses out there that also have these gene targets? Sure, and rare undiscovered viruses might even cause a false positive here or there. But the widely circulating respiratory viruses are all well known.
In July 2021, the CDC issued a lab alert saying the following:
After December 31st 2021, CDC will withdraw the request to the U.S. Food and Drug Administration (FDA) for Emergency Use Authorisation (EUA) of the CDC 2019-Novel Coronavirus (2019-nCoV) Real-Time RT-PCR Diagnostic Panel, the assay first introduced in February 2020 for detection of SARS-CoV-2 only. CDC is providing this advance notice for clinical laboratories to have adequate time to select and implement one of the many FDA-authorised alternatives.
In preparation for this change, CDC recommends clinical laboratories and testing sites that have been using the CDC 2019-nCoV RT-PCR assay select and begin their transition to another FDA-authorised COVID-19 test. CDC encourages laboratories to consider adoption of a multiplexed method that can facilitate detection and differentiation of SARS-CoV-2 and influenza viruses. Such assays can facilitate continued testing for both influenza and SARS-CoV-2 and can save both time and resources as we head into influenza season. Laboratories and testing sites should validate and verify their selected assay within their facility before beginning clinical testing.
Emphasis mine. It’s easy to misunderstand what’s going on here. The CDC is not actually saying that their PCR tests can’t distinguish between Corona and the flu. Rather, it’s withdrawing a PCR diagnostic panel for SARS-2 introduced in February 2020, because it was at this point 17 months into the pandemic, and many other PCR diagnostic panels were available. Unlike the original CDC diagnostic panel, these new panels are capable of detecting both influenza and SARS-2, whereas the earlier ones would light up only on SARS-2. If the patient had influenza, the test would come back negative.
If our health authorities were genuinely interested in measuring the prevalence of Corona across the population, they’d have used random sampling methods from the very beginning, testing separate pools of people both for the virus and for antibodies over time. Instead, their aim has been to propagandise the population to further their virus extermination agenda, which explains their unsystematic use of PCR. Crucially, though, this doesn’t mean there’s no information in official case statistics. Before Omicron especially, you could use surging case numbers to predict rising hospitalisation and death statistics several weeks into the future, which is the best proof possible that there is real information in these Corona dashboards, however otherwise broken they are. If the results of these tests were wholly arbitrary, they wouldn’t show trends over time, and they wouldn’t correlate with other medical outcomes.
As always, reality is in the difficult middle, rather than at the comfortable extremes of believing that it’s all true or it’s all a lie.
Update: This post has unsurprisingly attracted a lot of vitriolic comments, particularly about the phenomenon of high PCR cycle thresholds and the frequency of false positives. I guess I didn’t address this explicitly enough: The PCR is very good at detecting the genetic sequences that it targets. The problem with high cycle thresholds isn’t that these yield ‘false positives’ (i.e., they find virus where there isn’t any), but rather ‘meaningless positives’ in the context of diagnosis. That is, at high cycle thresholds, the test detects trace amounts of virus that aren’t relevant for establishing whether the patient is infected or infectious. Similarly, you could imagine a hypersensitive metal detector that detects trace amounts of metal being entirely useless for your garden variety weekend treasure hunter. The metal detector is detecting metal, just not in a way that is useful for the questions its user is most interested in.
This post was originally published on Eugyppius’s Substack. You can subscribe here.











To join in with the discussion please make a donation to The Daily Sceptic.
Profanity and abuse will be removed and may lead to a permanent ban.