Researchers inoculated (exposed) 36 people aged 18-29 with SARS-CoV-2 (Wuhan strain) via nasal droplets in the first COVID-19 challenge trial. The dose was similar to that found in a droplet of nasal fluid (which seems on the high side compared to natural exposure – who inhales globules of snot?). What did they find?
First of all, two of the 36 were found to have developed antibodies between screening and inoculation, so although they were inoculated anyway they were excluded from most of the analysis (they didn’t develop an infection, unsurprisingly). That left 34. Of those, 18 (53%) tested PCR positive, 17 (50%) of them with symptoms and one without. This means 16 (47%) never tested positive, despite being heavily exposed via lying on their back for 10 minutes with a blob of infected snot up their nose. Why did they not get sick? The researchers say investigations of these questions are ongoing.
This raises an interesting question of what constitutes infection, as clearly all participants had been thoroughly exposed but for 16 of them their immune system dealt with it in some way without resulting in symptoms or PCR positivity. The proportion infected, 53%, is higher than the proportion of the population typically infected in an outbreak, such as on the Diamond Princess (where 19% tested PCR positive), but that may be owing to the level of exposure or other transmission dynamics.
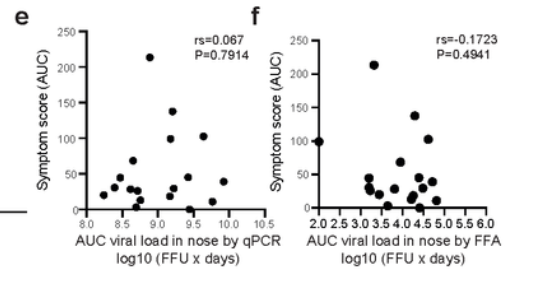
Interestingly, there was no correlation between symptom severity and viral load, measured both using Ct values from a PCR test and viable virus. Note the most symptomatic point in the charts below (the highest on the y-axis) does not have anywhere close to the highest viral load. Significantly, the one asymptomatic infection had no lower viral load or less viable virus than the symptomatic infections (the point sitting on the x-axis). This suggests that infectious asymptomatic infection may be a real phenomenon (though note this study did not test to see whether participants actually infected others).
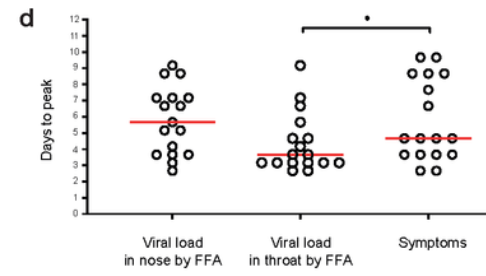
Viral load in the throat peaked on average around day three, a day earlier than the average peak of symptom severity on day four, itself a day earlier than the average peak of viral load in the nose (though the average peak viral load in the nose was higher).
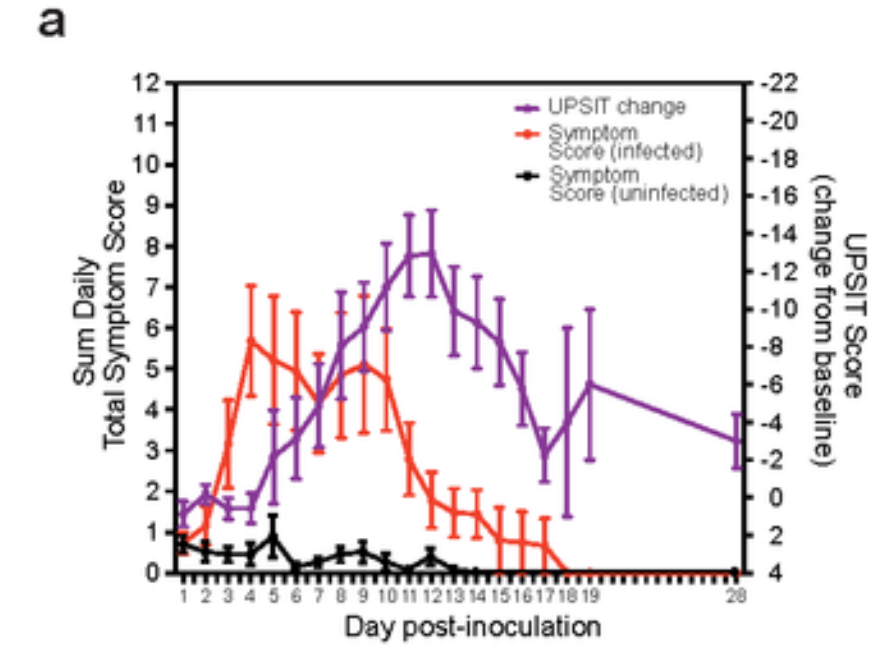
Symptom onset was often earlier, from day two, as can be seen in the charts below. No average value was given for symptom onset; however, the early symptom onset in many cases challenges the common idea that viral load peaks prior to symptom onset and drives pre-symptomatic transmission. That said, the early symptoms here tend to be mild. There are also questions as to how generalisable the results are to a natural infective dose, which is likely much lower.
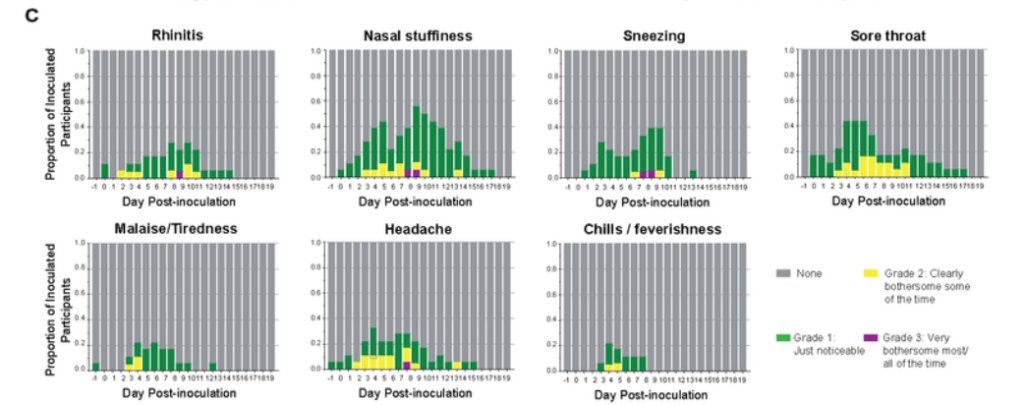
The participants were tested with a PCR test every 12 hours, and also with LFTs daily. The results from the LFTs found that an LFT went positive on average (median) on day four, one to two days after the PCR test went positive and one day after viable virus was detectable. The researchers report that LFTs “mainly” went negative two to four days after viable virus detection had ceased. This suggests LFTs tend to miss the early infectious period by a day and miss the end of the infectious period by two to four days. The researchers felt their results supported the use of LFTs for “interrupting transmission”, but that conclusion seems debatable.
The authors say they intend to do further challenge trials, including with vaccinated volunteers, to ascertain the difference that vaccines might make. However, since it is now generally thought that the chief value in vaccination is protection of the high risk from serious illness, it is unclear how a challenge trial, which uses only young healthy volunteers, can shed much light on this.
Read the full study (which is not yet peer-reviewed) here.











To join in with the discussion please make a donation to The Daily Sceptic.
Profanity and abuse will be removed and may lead to a permanent ban.