What is the evidence that SARS-CoV-2 originated earlier than December 2019 in Wuhan, and what are the implications of that for our understanding of the pandemic?
The purpose of this article is to provoke discussion about the origins of SARS-CoV-2 by collating a range of evidence from countries around the world – the U.K., France, Ireland, Italy, Spain, the U.S., Brazil and China.
The following table summarises at a glance the information presented in this article. (N.B.: ‘Reliability’ in the right-hand column is an assessment of how likely the evidence is, in this author’s view, to show the presence of SARS-CoV-2.)
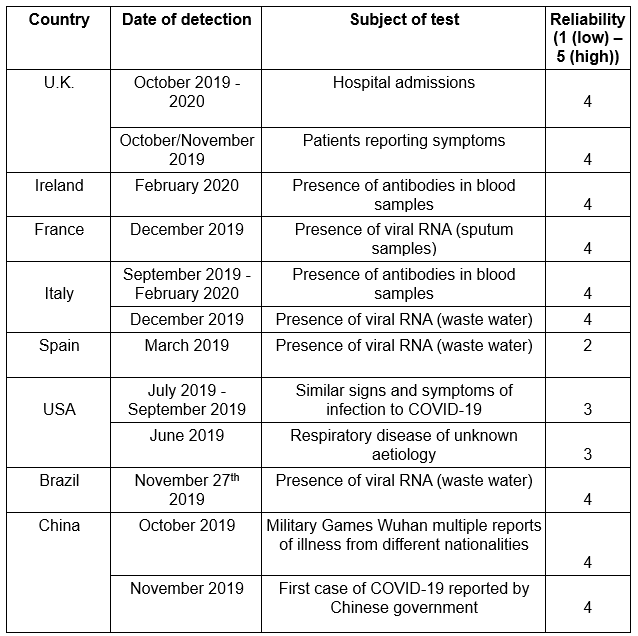
The ‘official’ timeline for SARS-CoV-2 (COVID-19) is that physicians in a hospital in Wuhan, China, reported a number of patients with a viral pneumonia of unknown aetiology in December 2019. In January 2020, it was reported that the pathogen was a coronavirus and had been isolated. The coronavirus was designated SARS-CoV-2 and the associated disease COVID-19. After the World Health Organisation declared a pandemic on March 11th 2020, testing for the virus by Reverse Transcriptase Polymerised Chain Reaction (RT-PCR or PCR) was ratcheted up around the world, with countries closing their borders and restricting the activities of their citizens.
Early on, anecdotal accounts started to surface suggesting the virus was actually in circulation some weeks or months earlier than the official timeline. The present article pulls together a number of these anecdotal accounts along with more scientific observations in the form of antigen and antibody testing that appear to corroborate the anecdotal accounts.
Anecdotal evidence is treated as low grade evidence at level five or six in the evidence pyramid after Sackett (see below); however, that does not mean it is worthless or should be lightly dismissed without investigation to see if it is corroborated by scientific observation.

United Kingdom
In the United Kingdom, I am aware of many people who have reported presenting to an urgent care centre with persistent cough and mild fever in October and November 2019. Some patients reported that the cough had lasted several weeks, up to six in one case. The fever was typically around 37.8-38.0°C. One patient reported a change in taste for seven days after having a cough for the previous five weeks, which resolved itself at the end of the first week in November. General practitioners known to the author working in the same urgent care centre reported parallel experiences from patients in their own practices. Other people from around the country reported similar symptoms around the same time on different websites.
Further evidence from this period comes in the form of hospital admissions for respiratory conditions obtained through freedom of information requests. The data come from the coding added to a patient’s notes after discharge using the International Classification of Disease (ICD; issue 10 was the latest edition at the time).
A graphical representation of the data from one trust, Frimley Health NHS Trust in Surrey, is shown below. The orange line represents all the patients admitted and diagnosed with any respiratory condition, the blue line is patients diagnosed with pneumonia, and the yellow line line is the number of patients with a positive SARS-CoV-2 test used as a proxy for COVID-19. When the medics in Wuhan first reported the outbreak they stated that there was pneumonia caused by an as yet unknown pathogen. The Frimley Health graph shows a steady increase in pneumonia diagnoses over the last quarter of 2019, before falling off in early 2020.
If all or most of the SARS-CoV-2 patients had COVID-19, a respiratory disease, then the orange and blue lines should track the yellow line and should not fall substantially below it. This suggests that the number of COVID-19 patients may be predominantly due to positive tests and not diagnosed disease (this assumes those assigning the codes did not routinely omit other ICD classifications such as pneumonia in COVID-19 cases).

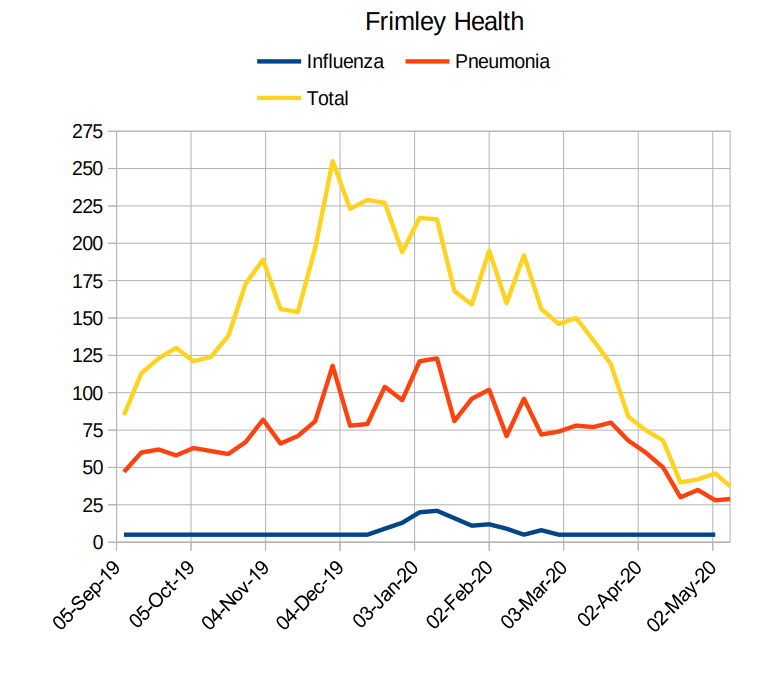
This next graph, also from Frimley Health, shows the number of patients coded with respiratory illness as before (yellow), the number of patients with a diagnosis of pneumonia (orange), and the number of patients with a diagnosis of influenza (blue). As may be clearly seen, there was no large winter peak in this trust for influenza in 2020, with cases trending well below the pneumonia and respiratory disease lines. Whether this is significant is unknown – it may again be a classification issue, and without data from earlier years against which to compare it it’s hard to know whether the discrepancy between the disease categories is standard or anomalous.
France
Deslandes and colleagues in 2020 reported on a patient hospitalised in December 2019 in a north Paris Intensive Therapy Unit who was coughing up blood with no diagnosis of cause. The researchers reviewed retrospectively the records of other patients admitted with influenza-like illnesses to ITU between December 2nd 2019 and January 16th 2020. Since every respiratory sample collected in the hospital is frozen and stored for four years, the researchers conducted RT-PCR tests on samples which originated from patients with influenza-like symptoms (temperature above 38.5°C, cough, sore throat, runny nose or muscle pain) or a ground glass appearance on chest radiography. Initially, 124 samples were available; of these, 44 were excluded as they had tested positive for other viruses. Of the remaining 80 samples, 66 were excluded for atypical COVID-19 medical records (though why the researchers didn’t test all of them just in case is not really clear).
Finally, nine samples from December 2019 and five from January 2020 were tested, 14 in all. Of these, one sample from December 2019 was positive for SARS-CoV-2 whilst the remaining 13 were negative.
This patient predates the first official case of COVID-19 in France by approximately four weeks and had had no recent overseas travel or a link with China.
Ireland
Butler and colleagues in 2022 tested 8,509 samples taken from blood donors in the Republic of Ireland between February and September 2020, screening them for SARS-CoV-2 antibodies using multiple testing devices. The first samples that tested positive were those collected on February 17th, some 14 days before the first official notification. Significantly higher antibody presence was identified in Dublin and in donors under 40 years of age. As antibodies last for up to 90 days, the virus could have been circulating as early as the end of November 2019.
Italy
Apolone and colleagues in 2020 reported that between September 2019 and March 2020 in Italy, 959 patients were enrolled on a prospective lung screening trial that involved the taking of blood samples, with the monthly enrolment as shown below.
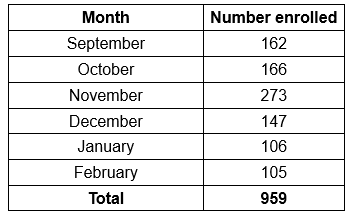
The first cases of COVID-19 in Italy were identified in January 2020. However, the rapid spread and the number of seriously ill patients suggested to the researchers that the virus may have been circulating several months previously. Samples from the 959 participants were tested for the presence of two types of SARS-CoV-2 antibodies, IgG and IgM. Of the 959 samples, 16 were found to have IgG and 97 were found to have IgM (some had both). The data pertinent to this discussion are presented below.
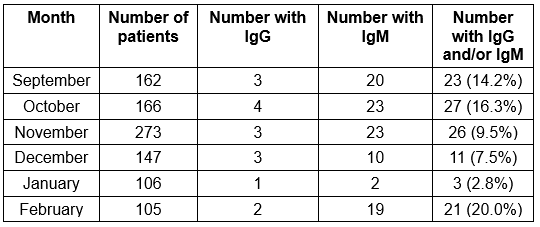
When the weekly data are examined, the researchers show that there are two distinct peaks, one in the second and third weeks of October (18% IgM positive) with the second occurring in the second week in February (30% IgM positive). Between these two dates the number of patients with IgG or IgM antibodies drops significantly.
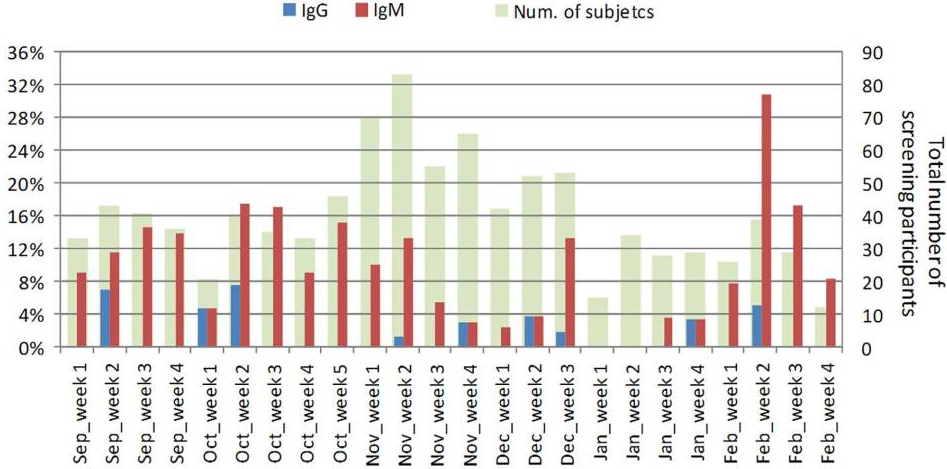
A similar pattern is seen if the Lombardy region is examined in isolation, as shown below. Lombardy is significant as this is the region most affected by the pandemic, according to the Italian Government.
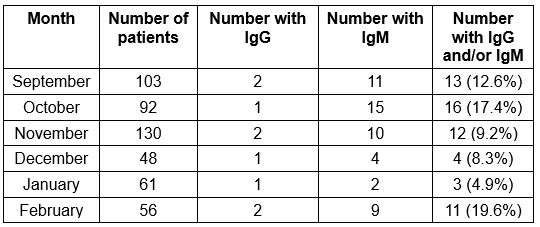
IgM antibodies are significant in that they appear early in the course of infection, reappearing to a lesser extent on further exposure to a pathogen. If IgM antibodies are present in a patient’s serum then he or she has had a recent infection.
IgG antibodies appear after the maturation of the antibody response when B cells switch from creating IgM; thus the presence of IgG demonstrates a later stage in the immune response. Unlike IgM, the presence of IgG is more indicative of a person’s immune status to a given pathogen.
Concern about the possibility of false positive results needs to be addressed. These tests were undertaken using a technique called microneutralisation assay, which according to Manenti and colleagues is the most reliable in terms of the obtained results. However, while the study does not discuss its limitations, other studies have mentioned possible cross-reactivity of antibodies as a limitation. It would also have been reassuring to have seen results for earlier samples, both to see when the antibodies first appeared and as a control.
The authors conclude that SARS-CoV-2 was circulating amongst individuals (asymptomatic at the time of their blood sample, though not necessarily at the time of infection) several months before the first patients were identified in Italy or Wuhan. The first official cases identified in Italy were two Chinese tourists on January 19th 2020.
La Rosa and colleagues in 2021 reported on the testing of waste water samples from five different sites in northern Italy between October 2019 and February 2020, using 24 samples obtained from the same sites between September 2018 and June 2019 as blank controls. Fifteen confirmed positive samples were identified, with the earliest dating back to December 18th 2019 in Milan and Turin and January 29th 2020 in Bologna. The absence of positive samples prior to December is curious given the antibody results above.
Spain
Chavarria-Miró and colleagues in 2020 reported on the testing of waste water in Spain for the presence of SARS-CoV-2. Initially this was for the period April to May 2020, when the virus was known to be active in the country, in an attempt to understand the progression of the virus in Barcelona. These samples were 24-hour aggregations of samples taken from each of two sites that were analysed weekly. Similar assays were undertaken on frozen samples for the first quarter of 2018, the first and last quarters of 2019 and the first quarter of 2020.
The first case of COVID-19 reported in Spain was February 25th 2020. However, analysis of the samples from the first quarter of 2020 showed the presence of SARS-CoV-2 in the sample from January 15th. Of the multiple samples covering 2018 to 2019, only one had a positive result, for March 12th 2019. This could be an anomaly due to cross contamination or it could be genuine.
United States
In 2019 there was an outbreak of severe lung disease in the United Sates that was attributed to the use of e-cigarettes and vaping and is termed EVALI by the CDC. The first cases were reported in July 2019 in Wisconsin and Illinois, spreading to all 50 states and peaking in September 2019. The rates of EVALI reported for the months June to August 2019 in Illinois were twice those for the same months in 2018 (see papers by Layden and Segreto). Of significance are the parallels between EVALI and COVID-19, with a diagnosis of EVALI being one of exclusion (i.e., by process of elimination).
Pitlick and colleagues in 2021 reported on a 34 year-old male who presented with shortness of breath, cough, headaches and other symptoms. A chest X-ray showed abnormalities and he was presumed to have a pneumonia. He was treated with antibiotics but did not improve; in fact, he worsened, requiring supplemental oxygen, and a chest CT scan showed a ground glass appearance. He was treated with further antibiotics without any improvement. He was then treated for EVALI with steroids and he improved, being discharge five days after admission. However, multiple tests for SARS-CoV-2 came back negative. Could this have been COVID-19 instead of EVALI? COVID-19 is a viral infection and hence treatment with antibiotics would be superfluous, whereas steroid treatment would be beneficial. The negative PCR tests count against the possibility, however.
A news report from July 2019 indicates there was a respiratory virus circulating in a retirement community in Fairfax County, Virginia in June 2019, the symptoms of which were cough and fever with pneumonia developing. This was around the same time that the military lab at Fort Detrick was closed after failing a safety inspection; I note that Fort Detrick, MD, is approximately 50km from Fairfax, VA.
Basavaraju and colleagues in 2020 reported on reactive antibodies to SARS-CoV-2 being present in U.S. blood donations in December 2019 and January 2020, when the first reported infection in the USA was reported on January 19th 2020. SARS-CoV-2 reactive antibodies were found in the states of California, Oregon and Washington in samples from mid-December 2019. Antibodies develop after seven to 10 days and may last up to 90 days, thus they could have developed as early as mid-September or as late as the beginning of December 2019. The authors caution that the samples included in the report may not be a true representation of all blood donors and hence their observations should not be taken as a generalisation across all donors in the same time period. Thus, it would be inappropriate to infer the number of infections at a state or national level. Further studies are required to corroborate the findings which are suggestive of the presence of SARS-CoV-2 in the U.S. earlier than officially admitted to.
Brazil
The first official case in Brazil was identified on February 25th 2020. Although SARS-CoV-2 is a respiratory virus, it is known to infect the gut where there are ACE2 receptors; up to 100 million SARS-CoV-2 genome copies are found in each gram of faeces.
Fongaro and colleagues in 2021 tested six samples of raw sewage from Santa Catarina, Brazil. The samples were taken on October 30th 2019, November 6th 2019, November 27th 2019, December 11th 2019, February 20th 2020 and March 4th 2020. SARS-CoV-2 RNA was detected using commercially available RT-qPCR equipment. Negative control tests were performed to ensure sensitivity and specificity. Finally, tests were undertaken in an independent laboratory in a blinded environment using different analysis machinery. These two tests produced similar results, indicating that the samples from October 30th and November 6th were negative, whilst the subsequent samples from November 27th onwards were all positive. This strongly implies that SARS-CoV-2 was in circulation in Brazil some 90 days earlier than reported.
China
In October 2019, 9,000 athletes representing the military from 100 countries attended the Military Games in Wuhan. Several French participants returned from these games with a mystery illness, with one non-participant being admitted to hospital with pneumonia in December 2019. A sample taken from this patient on December 27th tested positive for SARS-CoV-2. Participants from Germany, Italy and Luxembourg all state that they had COVID-19, although the Swedish contingent stated that they tested negative despite being unwell (though which kind of test they are referring to and when they were done is not clear from the press report).
Pekar and colleagues suggest there were cases of COVID-19 as early as November 17th 2019 as recorded by the Chinese Government, although most of the first cluster was associated with a seafood wholesale market in December 2019. Using genome data collected from early cases of COVID-19 and analysed with molecular clock techniques, the time of the most common ancestor to the sequenced genomes is estimated to be late November 2019 (with uncertainty estimates pushing this back possibly to mid-October).
Absent signals
What is missing over this period are reports of excess deaths, which became apparent in the U.K. and some other countries in March and April 2020, when there were significant numbers of admissions to hospitals, usually of older people. Bearing in mind the median age of death with COVID-19 in spring 2020 was 83, one possible explanation for the lack of excess deaths is that the people infected in the last quarter of 2019 were younger and hence less likely to experience severe symptoms or to die. How a circulating infectious respiratory virus would not have reached the older population during the winter is unclear, however.
Conclusion
Although not conclusive proof that SARS-CoV-2 was circulating several months before it was officially recognised, the evidence presented here does give food for thought. It suggests the possibility, for example, that Wuhan was not the original source of the virus but only the place where everything came together. Could it have originated in the USA, bearing in mind that Fort Detrick was closed due to safety concerns in July 2019, or in Europe, with Wuhan simply being where it was first spotted? The apparent artificial origin in ‘gain-of-function’ research needs to be accounted for, of course.
Could it have been the military games that brought the virus into Wuhan in October 2019, as the Chinese Government has suggested? Or could the military games have enhanced its spread from Wuhan across the world?
What does need to be explained is the apparent synchronicity of large numbers of infections in different parts of the world, with significant outbreaks (with large numbers of deaths) occurring within weeks of each other in Italy, Spain, the U.K., France, Sweden and New York, among other places.
It may be significant or it may not be that Frimley Health NHS trust above includes the garrison town of Aldershot in its catchment area.
Some have proposed that the pandemic was a deliberate ploy on the part of the USA or others to besmirch China through a false flag operation. Others have proposed a double bluff by China – noting the financial benefits from, for example, the manufacture of masks, PPE etc. The country’s crippling Zero Covid strategy in recent months would suggest this is an unlikely explanation, however. The standard explanation is that it was something unintended, of course, whether a lab leak or a natural event.
In any case, what does need to be answered is how to prevent the same situation arising in the future, where the actions of one country in imposing draconian public health measures can paralyse most of the world with fear. The WHO carries much of the blame here for becoming an early cheerleader of the Wuhan lockdowns.
What needs to be emphasised is that the information presented here does not mean that the wave of infections reported in March 2020 was non-existent. Many people were clearly experiencing symptoms and reporting them, and they were later found to have antibodies to SARS-CoV-2. Neither should it be presumed that many of the excess deaths reported for March and April 2020 were not due to COVID-19, although data suggest there were a significant number of excess deaths from that time that were not Covid related and are more likely lockdown and policy related.
John Collis is a recently retired nurse practitioner.












Profanity and abuse will be removed and may lead to a permanent ban.